Positive Health Online
Your Country

Complementary Therapies for the Menopause - Research Study
listed in women's health, originally published in issue 105 - November 2004
Background
UK medical education delivered to trainee doctors has traditionally devoted little time to the study of complementary medicine. With over one-third of patients now using complementary and alternative treatments at some time in their lives,[1] one medical school has attempted to change this. Encouragingly, all medical students at Newcastle University are given a focused resource day of teaching in their third year of study. Furthermore, those with a particular interest in this area can elect to spend an additional seven weeks exploring this field. Teaching is coordinated by Dr Anand, a GP at Elmfield Health Group, Newcastle upon Tyne. Students visit the members of 'Health 2000', a group of North-East complementary practionners, and experience therapies including Kinesiology, Homeopathy, Osteopathy, Yoga, Crystal Healing, Shiatsu and Acupuncture. Students are able to meet patients, participate in therapies and witness their integration into mainstream medicine at Dr Anand's surgery.
Having just completed this course, I can conclude that it provides a very valuable learning experience. It has enabled me to make an informed evaluation of the merits of different therapies and to reflect upon the limitations of 'conventional' medicine and the NHS. I hope that I will take a more holistic approach to my practice and to use complementary therapies to put more emphasis on preventative medicine. During the course, students are encouraged to conduct a small research project. I hope to become a GP and felt it would be appropriate to look at complementary therapies and the Menopause.
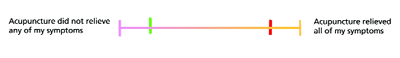
Figure 1. Analogue Scale Used
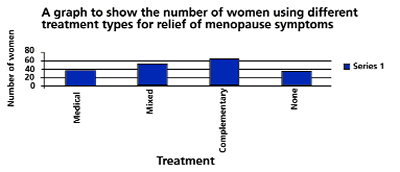
Figure 2. The Number of Women Using Different Treatment Types for Relief of Menopause Symptoms
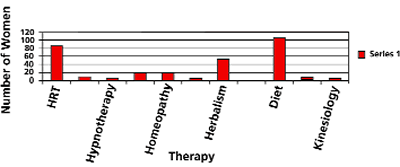
Figure 3. Number of Women Using HRT and Each Complementary Therapy
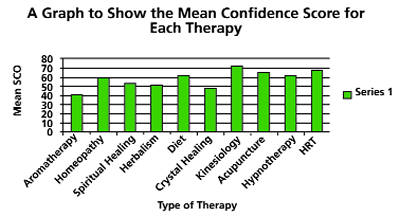
Figure 4. Mean Confidence Score for Each Therapy

Figure 5. The proportion of people who have used more than 2 therapies, who have used and not used HRT
Research Study: An Assessment of the Value of HRT and Complementary Therapies in Symptom Relief for Menopausal Women
Introduction
Whilst the Menopause could be viewed as a natural part of a woman's life for which interference is unnecessary, others believe that it is a true state of hormone deficiency. Those 20 per cent of women who suffer badly at the Menopause and perhaps 60 per cent of those who suffer milder symptoms are those who present themselves at doctor's surgeries.[2] Hence, it's easy to see why the medical profession has adopted the attitude that the Menopause is a condition requiring treatment. Complementary therapies are said to have a great deal to offer at the Menopause, making use of naturally occurring substances and utilizing a human's natural capacity to heal. Therefore the aims of this research were:
1. To audit the use of HRT and Complementary Therapies for control of Menopausal Symptoms;
2. To assess the benefit of these therapies for symptom relief, from the patients' perspective.
Method
The mean age of the Menopause in the UK is 51.3 Therefore all women aged between 45 and 60, registered at Dr Anand's surgery, Elmfield Health Group, were asked to participate. This was a postal survey; each woman was sent an information letter, questionnaire, consent form and return sae. Participants were given a list of examples of menopausal symptoms such as hot flushes, night sweats, depression, loss of libido, vaginal dryness, insomnia and thinning skin and hair and asked if they believed they had experienced them. If they had not experienced them they were still asked to return questionnaire. If they had, they were asked if they had consulted their GP about menopausal symptoms and whether they had used HRT and a variety of complementary therapies, obtained either over the counter or by visiting a therapist. For therapies that they had used, they were asked to complete a visual analogue scale to demonstrate how they felt about the role of the therapy in relief of their menopausal symptoms. For example, if a patient had used Acupuncture. (See Figure 1). The line on the questionnaire measured 100mm, therefore allowing a 'confidence' score to be calculated between 0 and 100.
Results and Discussion
225 viable surveys were returned, giving a response rate of 42.3 per cent. The mean age of those with symptoms was 53.7 yrs. A limited number with no symptoms replied – 15.3 per cent with a mean age 49.75 years. 63.5 per cent of those with symptoms visited their GP. This figure is high when research suggested that only one-third of women visit their GP.[2] It seems that women who have symptoms and visited their GP, made up the largest group of respondents.
Different Treatment Types Used
The following 'Treatment Types' were created to permit clear analysis of the results: 1. Medical – i.e. HRT; 2. Mixed – i.e. HRT and Complementary Therapies; 3. Complementary alone; 4. No treatment. (See Figure 2:)
Only 19 per cent of women took HRT alone; 63 per cent took HRT and Complementary Therapies or Complementary Therapies alone, indicating that these therapies are popular with women at the surgery; 34.7 per cent of women had used Complementary Therapies alone, forming the largest group. Perhaps the 18 per cent of women who have had symptoms but not taken anything, are only experiencing mild symptoms.
Figure 3 shows the number of women using each therapy.
More women used Diet, which in this study included healthy eating and phytoestrogens than HRT. Diet, followed by Herbalism and then Homeopathy, are the most commonly used therapies and it is interesting to note that these are the therapies that involve ingestion of a substance. 89 per cent of women who used Herbalism also used diet.
Value of Therapies in Symptom Relief
See Figure 4. Each of the therapies had a large range in confidence scores, indicating that the benefits of each therapy are largely dependent on the individual. For example, HRT scores ranged from 2 to 100. All of the mean scores were between 39.5 and 71.5. Interestingly the mean score for HRT was 66.5 (n=86) and for Diet 60.7 (n=103). This is a significant finding. Although Kinesiology had the highest mean score of 71.5, only three people used it. The therapies with lowest scores are 'healing' therapies, i.e. Crystal and Spiritual Healing.
The Biggest Users of Complementary Therapies
See Figure 5. Despite 28 per cent of the total number of women using complementary therapies and HRT, women who have not taken HRT have tried more complementary therapies. The fact that fewer women on HRT try a range of complementary therapies could be due to the fact that they feel that HRT works and do not seek alternatives, or they are not interested in complementary therapies. Furthermore, it is interesting to note that 69 per cent of women who have visited their GP about menopausal symptoms have taken HRT. This figure could indicate that the GPs in this practice are promoting complementary therapies or perhaps it could be due to the media scares about HRT.
Summary of Conclusions
A majority of women, 63 per cent, have tried some form of complementary therapy for relief of menopausal symptoms. The most popular complementary therapies among participants were Diet, Herbalism, Homeopathy and Aromatherapy. Women who have not taken HRT try a larger range of therapies and more women in the study have used Diet than HRT. The study found a similar mean confidence score for Diet and HRT (66.5, HRT 60.5 for Diet). Other confidence scores ranged between 39 and 70, indicating that complementary therapies have a valuable role in relief of Menopausal symptoms.
Limitations
The results may be limited by the 'types of women' who replied to the survey. Data show that the majority of women who replied were those who had sought advice from their GP. Few women who had not had symptoms replied. A further limitation is the possibility that women may not have been able to tell the difference between the benefit of two therapies if used at the same time. Furthermore each woman will have experienced the Menopause differently. A woman with severe symptoms may not have gained as much relief from a therapy as a woman with mild symptoms.An important point is that complementary therapies may be a significant cost to the individual, restricting use.
Future Recommendations
If the study were to be extended it would be interesting to attempt to gauge the perceived severity of an individual's symptoms and relate this to use of HRT and complementary therapies. Ideally, this study should have included more therapies; a few participants made extra comments about the benefits of yoga.
Implications for Practice
The study provides valuable and positive points of reflection for health professionals who are promoting Complementary Therapies at Elmfield Health Group. The confidence scores for symptom relief may be of value to individual women and to health professionals who recommend therapies. Perhaps the data could influence GPs to learn more about Diet and Herbalism, i.e. therapies that are popular and that GPs could potentially advise on. Finally, the research could potentially be of value to those applying for funding for Complementary Therapies in general practice.
I would like to thank Dr Anand, Dr Anthea Anand and all the members of Health 2000 for their help with this research.
References
1. Vickers AJ, Vickers Andrew, Zollman CE, Zollman. ABC of Complementary Medicine. BMJ Books. London. 2000.
2. Hall J and Jacobs R. Menopause Matters. Element. Shaftesbury. 1991.
3. Morris E and Rymer J. Menopausal symptoms. Clinical Evidence. 9: 2074-2086. 2003.
Editor's Note
The above study should be viewed in the context of a student research project. The sample size was limited, the range of treatments surveyed perhaps too wide for the small numbers involved. Much of the research data shown here is in its raw form. Therefore in order to extrapolate the results, further and larger scale research is needed with more sophisticated statistical analysis.
Comments:
-
No Article Comments available