Positive Health Online
Your Country

The Osteopathic Approach to Bursitis
listed in osteopathy, originally published in issue 186 - September 2011
Inference
The bursae lie usually where a mobile structure - usually a tendon/skin - crosses bone or hard connective tissue, especially where the route of a tendon bends around bone or its associated retinaculum. The bursae around the hip, knee and elbow tend to provide a dual function. As well as providing protection to the tendon over a bony prominence, they also allow the skin to move freely over the underlying bone. Bursae tend to be sacs of synovial membrane with a film of fluid between them, surrounded by collagenous/fatty tissue and tethered to the periosteum and sub-dermis by connective tissue. This allows for total freedom of movement and reduces friction between the two surfaces. They can also lie between tendons and between a muscle, tendon, bone and ligaments.
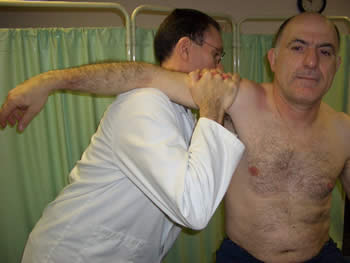
Shoulder Bursitis
Common Bursae Sites
There are a large number of bursae throughout the body and some become more symptomatic than others. This includes:
- Sub-acromial;
- Olecranon;
- Metatarsal;
- Calcaneal;
- Poplitial, Pes Anserine, Semimembranosus, Supra & infra, pre& post patellar;
- Trochanteric;
- Psoas/illiopsoas.
Causes of Bursitis:
- Repetitive/chronic strain injuries (mechanical);
- Acute tissue trauma;
- Infection;
- Arthritis (Osteo & rheumatoid);
- Gout;
- Tendon calcification;
- Tumour (rare).
The signs and symptoms of bursitis include local pain, swelling, heat, redness and occasionally muscle spasm/hypertonia. Diagnosis is usually made through direct palpation of tissue where point tenderness is usually noted directly over the affected bursae. In severe cases visible swelling is noted and palpable.
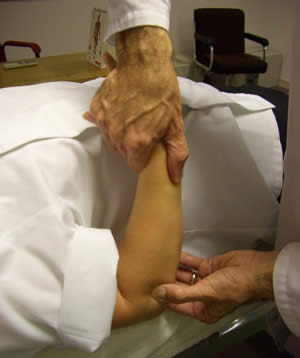
Elbow Bursitis
Sub-Acromial Bursitis
This condition is usually noted with painful arc syndrome (80° → 120° abduction) The cause is mainly of mechanical origin and is associated with supraspinatus tendonitis, which in severe cases becomes calcified. This direct irritation results in swelling and enlargement of the bursae, which becomes entrapped between the sub-acromial surface and the greater tubercle of the humerus during abduction of the gleno-humeral joint.
Treatment
Assess movement of the A/C joint and HVT if necessary.
↑ Kyphosis of thoracic spine + ↓ ROM → articulation / HVT/MET.
Assess Cervical Spine
Assess for anterior contracture of gleno-humeral joint muscles → soft tissue/MET.
There is usually fibrotic shortening of supraspinatus. This requires deep soft tissue inhibition, MET along with the external rotators (infraspinatus / teres minor) of the gleno-humeral joint.
Articulation to the gleno-humeral and periscapular joints.
Ice / NSAIDs/dry needling in acute phase.
Fig 8 exercise to thoracic spine.
Stretching exercises to the rotator cuff & periscapular muscles.
Olecranon Bursitis
Most commonly caused as a result of rheumatoid arthritis, gout, infection and repeat strain/chronic micro-tissue trauma/ irritation.
Bursitis from gout, the patient has a history of this condition and usually has tophi (sodium bi-urate crystals) in other areas notably earlobe and 1st met-phal joint. The olecranon bursa is swollen, red and painful which can also include the humero-ulnar joint having a limited painful range of movement.
Treatment
Aspiration, urease, painkillers and NSAIDs
Ice pack 10mins 4 x day.
Lymphatic drainage to the upper extremity + gentle articulation to ? joint dysfunction.
Advice on diet to avoid rich food.
Bursitis from infection commonly occurs in the sports arena following trauma / laceration allowing bacterial infection to gain hold, result hot swollen and painful bursae.
Treatment
Aspiration and antibiotics;
Lymphatic drainage to the upper extremity + follow up articulation to humero-ulnar and radio-humeral joints to ↓ joint dysfunction.
Olecranon bursitis from RA is usually non-painful swelling, joint dysfunction and all the classical signs and symptoms of RA and is usually aggravated by minor trauma.
Treatment
Strong NSAIDs
Lymphatic drainage to the upper extremity + gentle articulation to ↓ joint dysfunction.
Assess triceps and anconeous, gentle soft tissue if necessary.
Assess biceps; this may become shortened in chronic cases.
Contrast bathing to ↓ swelling.
Use of an elbow guard / pad to prevent further injury.
Olecranon bursitis due to repetitive strain/micro-tissue trauma occurs frequently in office/computer workers, racket sports and weight lifting. Irritation to the olecranon bursae from the tendon of triceps results in it becoming swollen and painful.
Treatment
Deep soft tissue to triceps / anconeous including Inhibition/MET.
Assess carrying angle, dysfunction of radio-humeral / humero-ulnar joints. Articulate/HVT where necessary.
Assess for fibrotic contracture of biceps and any fixed flexion deformity of the elbow joint as this can lead to excess tension on triceps tendon insertion at the olecranon.
During acute phase ice packs 10 mins 4 x day to ↓ swelling.
Stretching exercise to triceps.
1st Metatarsal-Phalangeal Joint Bursitis
This usually occurs as a result of Hallux Valgus (bunion) The prominence of the bone makes the area liable to friction and hence development of inflammation & bursitis.
This can be a particular problem in diabetic patients as the tissue is susceptible to infection and possible development of gangrene and eventual limb amputation.
Treatment
A soft gel pad over the area is sufficient usually to alleviate symptoms.
Ice pack to reduce swelling.
Lymphatic drainage to the lower extremity.
Advice on soft upper footwear.
Assess joints of the medial border of the foot HVT if necessary.
Calcaneal Bursitis
This is frequently caused by poor foot wear / hard backed shoes rubbing the calcaneal and Achilles area and commonly occurs in runners and young women (high heels). The constant friction causes inflammation and thickening of the calcaneal bursae and tends to be very painful. Plus there is usually associated shortening of gastrocnemius and soleus.
Treatment
A soft gel pad placed over the area is usually sufficient to reduce symptoms.
Advice on footwear. To include shock-absorbing insoles/heel pads.
Soft tissue / MET to gastro / soleus.
Exercises to stretch gastro / soleus on a regular basis. Hold 15secs x 3 per day.
Pes-Anserine Bursitis
This bursa is situated beneath the con-joint tendons of Sartorius, Gracilis & Semitendonosis where they insert on the medial aspect of the tibial plateau.
Usually found in patients with pes planus causing torsion through the knee and pelvic torsion anterior rotation of inominate, long leg resulting in semi-flexed knee and chronic shortening of the hamstrings notably semi-tendinosis. This results in friction of the bursae with associated swelling and pain, easily diagnosed on palpation as point tenderness.
Treatment
Orthotics
Deep soft tissue / MET to hamstrings etc
Deep friction to the bursae to create a healing crisis.
Appropriate dry needling to the area.
Ice packs in acute phase.
Correct pelvic torsion through HVT.
Stretching exercises to hamstrings.
Anterior Knee Bursitis
Supra-patellar Bursitis
Situated between the quadriceps tendon and the distal end of the femur proximal to the patella. Can become swollen and painful in patients who have to kneel in a fixed place hence the old term clergyman's knee. However the patellar can also be driven up into the supra-patellar bursa through maltracking problems associated with a weak vastus-medialis over developed quads esp vastus lateralis through over training.ie; runners, footballers and weight lifters.
Prepatellar Bursitis
Placed superficial to the patellar itself.
Infrapatellar Bursitis
Beneath the ligamentum patellae and the proximal part of the anterior tibia, with manifest pain and swelling noted over the tibial tubercle. In younger patients be aware of your differential diagnosis; Osgood Schlater's, Osteochondrosarcoma. & Ant cruciate.
Predisposed by repetitive direct friction in patients who move about on their knees. Therefore seen in carpet fitters, builders, and plumbers. Also excess friction from ligamentum patellae in over used/developed quadriceps muscles, athletes, runners, and footballers.
Occasionally caused by knee injury on a pitch/field/court, that becomes infected.
Treatment
Ice during acute phase, plus antibiotics if infected.
Assess for pelvic torsion. Anterior rotation of inominate (on the side of the bursitis) will result in a functional long leg. Hence to maintain balance the knee becomes semi flexed. In the physically active/sportsperson this can lead to excess friction on the Infrapatellar bursae resulting in swelling and pain. This can be corrected by a posterior HVT to the dysfunctional sacro-iliac joint to ie; Chicago technique. (Hartman)
Correct hypertonicity of quadriceps, through soft tissue/MET.
Direct inhibition to the chronic bursae creating a healing crisis, followed by lymphatic drainage techniques to the lower extremity.
Dry needling to the area.
Trochanteric Bursitis
The Trochanteric bursae is situated between the greater trochanter and the tendons of tensor fascia late (TFL)/gluteral muscles. Commonly caused by friction of the above tendons irritating the underlying bursae. It results in pain and swelling over the lateral aspect of the hip and is most commonly noted on walking and running.
Frequently it is predisposed by short leg on the side of the bursitis either organic (short tibia/femur) or functional (pes planus / posterior rotation of inominate). This results in chronic shortening of the above muscle/ tendons which then 'cut into' the Trochanteric bursae resulting in pain and swelling to the lateral aspect of the hip.
Easily diagnosed through pain noted on direct palpation of bursae.
Treatment
Orthotics to correct pes planus / short leg.
Correct pelvic torsion/ functional short leg through sacro-iliac MET/HVT to anteriorize inominate on the side of bursitis i.e. modified semi-sims HVT.
Soft tissue MET to TFL and gluteal muscles followed up by patient self-directed exercise programme to maintain the stretch especially in runners and athletes.
NSAIDs/dry needling.
Psoas / Illiopsoas Bursitis
The psoas bursa is situated beneath the psoas tendon and anterior to the hip capsule. When irritated usually by direct friction of the psoas tendon, local pain and swelling are noted in the groin along with palpable tenderness, effusion and anterior thigh pain due to irritation of the femoral nerve, plus associated weakness/pain on hip flexion.
Occasionally it is associated with psoas abscess/infection.
Treatment
NSAIDs
Antibiotics if infected
Correct any pelvic torsion through MET/HVT.
Soft tissue/inhibition/MET to psoas.
Bibliography
Chaitow L and Delaney JW. Clinical application of neuromuscular techniques. Volume 2: The lower body. Churchill Livingston, England. 2002.
Greenman PE. Principles of manual medicine. 2nd Edition. Lippincott Williams and Wilkins. Baltimore, USA. 1996.
Kreider RB, Fry AC and O'Toole ML. Overtraining in Sport. Human Kinetics, Leeds, UK. 1998.
Magee DJ. Orthopaedic physical assessment. 2nd edition. W. B. Saunders, Philadelphia, USA. 1992.
Pecina MM and Bojanic I. Overuse injuries of the musculoskeletal system. 2nd edition. CRC Press, London, UK. 2004.
Subotnick SI. Sports medicine of the lower extremity. 2nd edition. Churchill Livingston, England. 1999.
Ward RC. et al. Foundations for osteopathic medicine. 2nd edition. Lippincott Williams and Wilkins, Baltimore, USA. 2002.
Comments:
-
Eva Goes said..
Hi David,
This is very helpful and practical information.
I am suffering from a calcaneal bursitis, which hurts, but still allows me to run long distances. I was suprised to read that a gel pad covering the painful area could help me. Do you mean a blister patch, such as "Compeed"?
Thank you so much for you advice.
Best wishes,
Eva
-
Pat Horton said..
Hi David, I am almost 64, have been recently diagnosed with arthritis and Tronchanteric bursitis. I really do not want a cortisone injection, my GP has not recommended it only given me Nsaid's. I have almost no pain when I walk, a very little when I am sitting but at night the pain is chronic. My question is please, do you think Therafex will help. Money is an issue for me and I must make sure I use what I have wisely. I have also considered acupuncture. Thank you so much for your time.