Positive Health Online
Your Country

The Hospital and I - Excerpt
listed in medical conditions, originally published in issue 227 - January 2016
Between January and November 2014, I was a patient at one of the biggest and most modern hospitals in Europe, in a country whose language I did not speak.

* * *
Since the mid seventies when I was treated for migraine by a homeopath who was also a doctor, I have been a more or less fervent believer in homeopathy . I have had Type II diabetes for nineteen years now and I have tried to the best of my ability to treat myself for this condition. I am still alive, have both my legs and haven’t yet had a heart attack, nor have I gone blind. I can’t say these things, however, without being honest and telling you that I have lost considerable feeling in my feet and my hands before I settled into my own treatment protocol.
At the beginning of 2014, I suddenly suffered from urine retention as a consequence of which, my bladder swelled up and was very painful. I retired to bed for a few days and before the condition began to seriously affect me, I attended my GP. A few days after this appointment, nothing having changed, I attended hospital as an emergency outpatient; within a short period the doctors suspected and then diagnosed an enlarged prostate which was blocking my urethra. From this point onwards, under the care of the hospital I was slipped into their conveyor belt programmes for both an enlarged prostate and, on their decision entirely, my Type II diabetes.
I accepted the treatment for my enlarged prostate; with my condition at a crisis point I didn’t feel confident about reducing it quickly enough with alternative therapies. But after 18 years struggle with my diabetes during which I had brought down my blood sugar levels from between 20 and 30 to between 8 and 10, I was determined not to give in to pharmaceutical treatment.
The following essay, a record kept as a diary of my trips to hospital and the local community health centre, is an edited part of a much longer essay about the difficulties that I encountered in my dealings with the allopathic hospital and its professionals.
It was February when I first attended the hospital as an emergency. I was to be kept there for a period of four or five days; it was during this time, up against the heavily authoritarian regime, that I reformulated many of my ideas about the hospital. To base these ideas on the Emergency ward was perhaps slightly unfair, but then again it is perhaps always more instructive to examine the most extreme and resolved part of any system in order to lay the foundation for beliefs about the whole.
The emergency wards of the city’s biggest and most modern hospital is a foreign country with its own borders, its own language and most significantly its own political regime. The emergency wards through which hundreds of bodies pass every day is ruled by a ‘zombie oligarchy’. The oligarchs, the small group of powerful leaders, are the doctors and the zombies are the ‘patients’, nurses and auxiliary workers. The regime is tyrannical.
I had actually forgotten what The Hospital was like, it having been so long since I entered one. This time it was harder because I wasn’t in England and I didn’t speak the language. The industrial nature of the hospital is not confined to the ‘simple’ task of repairing bodies; the hospital is the last major point of delivery of industrial medicine.
The struggle to control my diabetes has taken up much of my time and energy over the years; predictably it was this that brought to the fore the most serious confrontations between myself and the Oligarchs. You might ask, “Why? Were you not in hospital for, or as a consequence of your diabetes?” No, I wasn’t, but a precursor to diagnosis and treatment for anything in an emergency ward, is complete compliance with a normative programme, in my case a normative diabetes programme.
Type II Diabetes is likely to enter the individual’s life in late middle age. The mechanistic reason that it develops can be described as long term damage to either insulin production or its receiving cells, leaving sugar without insulin or with non-functioning excessive insulin caroming round the body like a pin ball damaging organs. For a number of reasons I decided from the beginning to treat my diabetes with nutrition, life style changes and vitamin and mineral and herbal supplements.
What were the ‘number of reasons?’ Well, let’s see.
One of the first most popular pharmaceuticals for Type II diabetes was the GlaxoSmithKline drug Avandia. This medication was designed to replace Rezulin, a similar drug that was pulled from the market in 2000 after studies revealed it causes severe liver failure. In May 2007 the FDA announced that information obtained from clinical trials demonstrated that Avandia had the potential to increase the possibility of heart attack by 43 percent and may increase fatalities from general heart disease by 64 percent. In 2010, the lead author of another study, Dr David Graham, an FDA scientist, claimed that Avandia could have caused as many as 100,000 heart attack, heart failure and stroke deaths since it came on the market in 1999. Despite this study and others, Avandia has stayed on the market.
In April 2008 the Archives of Internal Medicine determined that patients who had been prescribed Avandia for at least twelve months were almost twice as likely to suffer a bone fracture as those who did not take the drug. More disturbingly, among patients who had treated their diabetes with Avandia for at least two years, bone‐fracturing levels had almost tripled.
Perhaps that is enough to give you an understanding of the primary reasons I did not adopt a medication regime. The approach of alternative medicine to type II diabetes is more complex than the approach of orthodoxy. Alternative medicine rarely sees health phenomena as simple mechanical equations, but tries in both diagnosis and treatment to deal with the whole person, physically and in terms of history, psychology and life style.
The first nutritional doctor that I consulted about my diabetes warned me that if I was intent on lowering my blood sugar levels, the regime was a rigorous one, not just nutritionally but also in terms of exercise. He quoted me the regimen of his most successful patient, an ex SAS member who put himself through a rigorous daily physical training session while regularly eating oily fish. After he said he doubted my capacity to stick to such a regime, I stopped seeing him - my disease was undermining me sufficiently without his help.
But it was then I think that I realized the most important difference between the pharmaceutical approach and the nutritional or alternative approach: the pharmaceutical approach was a quick fix with an indeterminate outcome while the alternative approach meant significantly changing the way you lived your life. My greatest regret about my diabetic self-management, eighteen years after I began it, is that I failed to begin a ‘new life’, forget about my writing for awhile and concentrate on a rigorous regime. Instead I began amending my life a little at a time, fitting in learning about approaches between work. Consequently I made many mistakes and there is no doubt that I lost ground to the illness in the first decade of dealing with it.
* * *

When I entered the emergency ward the oligarchs decided on a regime change for me and my type II diabetes. Nothing was discussed with me and I was expected to accept everything they did to me as if it were in my own interest, when in fact it was primarily in the interest of the conveyor belt smooth running of the ward. Every large hospital replicates an industrial or factory model of health care – failing bodies in, wellness or failed products out.
Despite the fact that I was knowledgeable about my own condition, more knowledgeable than some of the doctors, each of my confrontations resulted in loud and sometimes quite furious arguments.
The use of a pharmaceutical to control my diabetes: It is taken for granted by the oligarchs that anyone who has diabetes is taking a pharmaceutical; there is no space in the mind of a doctor for consideration of self-management. This is not necessarily because such treatments don’t work, but simply that the doctors know nothing about treatments other than pharmaceuticals. Consequently, from the moment that I was in the emergency ward I was asked obsessively what diabetic medication I was taking. It didn’t matter how many times I said I wasn’t on a pharmaceutical medication, I was asked again. This bind resulted in one of the most interesting conversations of my stay. I could just understand what the nurse was asking me when she came round to take my blood sugar and other details; it seemed to be a question about what drug I took for my diabetes at home. I replied as carefully and as succinctly as I was able that I didn’t take any.
The nurse became increasingly frustrated, more or less insisting that I must be taking something. Eventually when the exchange came to a grinding halt the nurse called over another nurse who seemed to speak more English, she said to me, "She wants to know what medication you usually take for your diabetes.’ I became quite angry, “I don’t take any pharmaceutical medication.” The nurse lowered the mask she was wearing and looked at me with a dawning comprehension, as if I was a species she was seeing for the first time.
“I know,” she said as if diving an oddity in my character, “you manage your diabetes with diet and life style changes” and she smiled broadly. These were the first intelligent words I had heard after coming onto the emergency ward. I thanked the nurse profusely. She smiled again and then said, “It doesn’t make any difference to the fact that she has to write on the form the name of the pharmaceutical you take, there is no box for diet and life style management.” I shrugged my shoulders, “She’ll just have to make something up then.”
The drips: Despite the fact that my kidneys appeared badly affected by the urine retention, that had brought me into the emergency ward; I was not encouraged to drink water, nor was I given any water. I was fitted with a saline drip from the first moment I was on the ward.
The use of glucose in a drip: Some hours after I had been on the ward, I read the label on the saline drip, only to find that there was glucose in one of the drips. I was a diabetic and being given intravenous glucose without permission.
The finger prick test: The finger prick test was carried out twice a day and initially the figure was not shared with me. This, of course, made me feel impotent and inadequate.
The use of insulin: When my blood sugar level was high, for whatever reason, the doctor in charge ordered a nurse to inject me with insulin. From the first occasion I fought this, although I didn’t manage to establish my complete objection to its administration with the doctors in charge. The night before I was discharged, I fell asleep early and was woken suddenly in the shadow of night by a nurse already holding my arm with the syringe in her other hand about to inject me. I did not disguise my anger.
Perhaps the hospital diet should not be included in this list because it was not compulsory. However, it led to at least one serious disagreement between one of the doctors and myself.
Forty per cent of all the food I was given consisted of white bread or white toast made with refined flour (I had stopped eating bread completely). The fruit I was given was always a large single fruit like an apple or an orange (I tried to eat berries and only occasionally had small amounts of other fruit). The second main meal that I was given was a plate of potatoes – potatoes although they consist of complex carbohydrate, are renowned for quickly rocketing blood sugar levels.
For one meal I was given white rice with a vegetable. What concerned me about these meals was that the doctors in charge didn’t seem to recognize or understand the relationship between type II diabetes and refined simple carbohydrates. This was clearly because the drug protocol that 98% of Type II Diabetics are ‘pushed’ into, assumes that as the medication is always effective the patient can eat exactly what they want.
One of the doctors remarked to me that I should feel better now that I was eating regular meals. I remarked that the meals seemed to consist mainly of white bread made with refined flour, which “I did not eat.” The doctor responded angrily to me, “Of course you can eat bread, don’t be silly.”
The matter of food led to another quirky and interesting conversation with two auxiliary workers. My partner brought in some walnut biscuits, which together with almond biscuits had at that time replaced bread in my diet. The biscuits are made with fresh (raw and unsalted) ground almonds or walnuts, a small amount of butter, an egg, a pinch of salt and another of bicarbonate of soda. As I was eating one of these, the two auxiliary workers stopped at the end of my bed and began talking to my partner. They asked, looking at the colour of the biscuits if they were wholemeal and when my partner replied that they were actually made from nuts without any flour one worker told us she was a coeliac but found it difficult to buy things without flour. She asked for the recipe.
February: Having left the hospital emergency ward, where I had spent a week and gained two new urology doctors, a very attractive, personable and intelligent young woman and a handsome and personable just married younger man, I became an outpatient, existing in a kind of shadow land between illness and orthodox medical diagnosis.
Yesterday at the hospital was a day of waiting, serious pain and humorous illogicalities from my doctor and her nurse. With regard to the pain, this was caused initially by the catheter, which now ran from my bladder to a bag on my lower leg. One thing though which I have never understood is the approach of nurses and others who try to deal with the patients' pain by insisting that it doesn’t exist, that the patient simply has to relax. Surely if you could relax when someone was pushing a wide catheter up your penis, you would, wouldn’t you - well I would!
This is of course a professional conundrum; it is after all difficult for any feeling person to happily cause another person pain. I remember once having my leg stitched up after acquiring a wound. As I grimaced, the doctor performing the procedure said, “Does that hurt?” when I said “Yes,” he said, “Funny I can’t feel a thing.”
The illogicalities that come from Pilar my female doctor, said with a straight and dead pan face are mostly to do with alternative medicine. Here are three of them, spoken over a period of weeks.

ME: Tell me, in the Urology department do you work with natural therapies as well as pharmaceuticals.
DOCTOR: No, we only use treatments that work. DOCTOR: I took a look at your web site yesterday, it’s hilarious. www.slingshotpublications.com/
ME: But it’s meant to be very serious critique of orthodox medicine. DOCTOR: Yes, hilarious.
ME: Can you tell me what foods adversely affect your prostate?
DOCTOR: What foods affect your prostate? (Looks puzzled)
ME: Come on, it’s a simple question which foods shouldn’t you eat if you have an enlarged prostate?
DOCTOR: Well, I don’t know about foods but there are herbs and other things you can buy in a health food shop that you shouldn’t take.
ME: Wow, that’s convenient. But then doctors don’t know anything at all about nutrition do they?
DOCTOR: No, nothing. (smiling)
The most illogical thing, however, I only saw when I got home after they had put a second catheter in me. I did relax to some extent and for a moment I took my eye off the ball. Getting undressed that night, which is scary enough with a bag and a catheter strapped to your leg, I found that I couldn’t get my boxer shorts off because the nurse who kept telling me to relax, had run the catheter from my cock, through the flies of my boxers and down to the bag strapped at my ankle, so there was no way I could take off my boxers. It was all too much of a struggle last thing at night and I finally had to cut my boxers in half with scissors.
April: Hospital again today. My male doctor is overly concerned about me having a diabetic crisis when I have my prostate operation - stress of all kinds affects your blood sugar levels, this is why my readings are always high when I attend hospital. But this time it's my heart that's worrying 'them'. On the conveyor belt for my prostate operation, my doctor insists that I go and talk to the anaesthetist and discuss my worries over the type of anaesthetics.
The anaesthetist looks at my screen record and her face falls like a rock in a pool. She could hardly speak. Apparently unbeknown to me I had had a 'major event'; such a shame I didn't know to feel it, I gather it's something like a Buck House garden party.
I couldn't have an operation, I couldn't have an anaesthetic, I couldn't have F’all until this was sorted out. I was fixed up with an emergency appointment with the heart people; about the exact time and date they would telephone me. Time went by without a phone call. All the time of course I was scared shitless that I was about to have another 'major event'.
After days of ringing the hospital, someone somewhere in the deep recesses eventually picked up a phone. I can have an appointment with the ‘cardigan’ person in June; three months away. An argument ensues, voices are raised and they find me, like a lucky dip winner, an appointment for the next day, in the morning.
April: I have spent a week teetering on the edge of a suspected heart attack, my mood created by sheer fear. I could see from first sight that the person I had come to call the 'Cardi' man, was not greatly pleased to see me. For a start the cardiman was a woman. If she had learnt smiling at senior school she had by now forgotten it like other foreign languages. I sat down and she asked me for my medical narrative, which I gave her. She asked me if I had any chest pains, I told her that I did not. She asked me if I was short of breath, I told her that I was not.
She tested my blood pressure and showed me the digital result, suggesting that it was high. She looked seriously concerned about the level and went back to her screen where I presumed she was looking again at the results of my electrocardiogram.
She said, "You didn't have a heart attack or anything like it." Oh well that’s that then, utter false alarm.
She asked me to remove my shirt and she smeared gel on my chest from the end of a small handheld digital ultra sound pen with which she carried out an 'echogram' - was she looking for that missing plane or maybe she going to tell me the name of my baby. Having listened to my heart to her satisfaction, she said, “Well that's OK,” Then, “There is a little damage to your heart, a little hardening of the left ventricle; it may be caused by high blood pressure.”
She went back to her computer screen, wrote in some notes and looked up at me as I wiped the gel off my chest with the tissues provided - the only point at which hospitals and massage parlours meet! I was quite angry at what had happened. At having been told I had had a major event. I tried not to raise my voice, but rather made a joke of it.
“Well, it certainly could have given me a heart attack the amount I've worried about it!” She looked at me as if she was trying to remember how to smile.
I sat down opposite her, “What are we going to do about the high blood pressure?” "Medication" she said, before the words had completely left my mouth, and it wasn't a question.
She began writing out the prescription. “I would like to talk about the medication,” I said, fluttering my eye lashes in a vain attempt to get her interested in an exchange of some kind.
She carried on writing. “I would like to know if there are other choices and if this medication has any adverse reactions.” Her voice was now as flat as a billiard table, “This is the only one and it has no, absolutely no, adverse reactions.”
“Oh, OK” I said. I was a little non-plussed, I watched in silence for a moment while she finished the prescription.
Then I thought, I might as well go for the big one, so I cleared my throat and raised my voice “Are there any foods that I should steer clear of, or any that might help my heart?” She was looking down at the table, with thunder in her eyes, “Salt,” she said.
After I had caught up with the translation, I said, only tentatively, “Yes but surely there are other things I can do?”
She looked at me as Leonardo Da Vinci might have looked at a piece of charcoal, “Salt ... stop using salt.”
I was on the edge of being rude but I remembered my left ventricle, expressed my sincere gratitude, took the prescription and the paper work for delivery with the 'anaesthesiologist' and left.
Returning home I felt strong enough to do a little research. A look in the medical literature revealed that there was an academic and scientific row raging about the med she had prescribed me, one paper suggested that it might increase the chances of heart attack by around 45%.
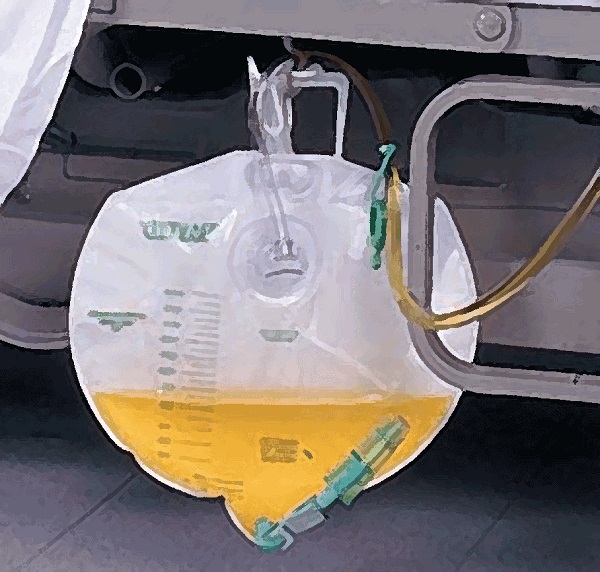
May: Three days ago I had a bad blockage in the catheter but after jumping up and down a little and drinking a lot of liquids I unblocked it. It came back and by last night I had gone for a day and a half without anything entering the bag. So, concerned about the deleterious effects of this urine retention, which by the middle of the night was causing me some pain, I decided to go as early as possible to the hospital and see my female doctor.
Don’t ever go to a hospital without a plan, even if you come away without having accomplished it. My plan was to see my doctor with whom I have some understanding - I try to gain control of my own ‘case’ and she takes the piss out of me (literally and metaphorically) for my alternative views. The relationship is, however, slightly better than this makes it seem, because I sense in her a real desire to listen to the views of her patients, well, me at least, and what is perhaps more important, I actually trust her. And she had sussed that I needed to be involved in my treatment so she tried to do this. So, my plan was on seeing her, to ask her to clean the catheter and, if she thought it necessary, to change it. I had no way of knowing that my doctor would be in today, so I just had to take the chance. I got the 6.30 am bus to the interchange in the city and then got a second bus to the hospital. I had not been on the bus long before the catheter unblocked and the bag at my ankle started to fill up, I put this down to the jogging of the bus over speed bumps - perhaps this is something that orthodox medicine should consider.
The hospital is a closed world, bordered by non-opening windows and smooth marble style walls. An impenetrable institution, within which orthodox medicine, doctors, nurses, clerks and technicians live out a soap which bears no relation to real life or the outside world.
I walked along the corridor to the reception for the Urology department. I knew as soon as I saw the receptionist that it was going to be a bad day. She was a partially blond young woman, who although she wasn’t at that time, probably chewed gum. She read the note written by my partner, that I had brought - it told the receptionist that I was without her language and that I wanted to see my doctor Pilar. The receptionist smiled at me sadistically before jabbering on fifty to the dozen. When she stopped she smiled again this time at my dazed incomprehension and waved me to the empty chairs in the waiting area.
The waiting began, like a Sergio Leone movie. Little things crossed my mind which took it off the fear of having the catheter changed, I sat in the waiting area for two and a half hours. A young woman doctor in a green lab coat beckoned me from inside the reception area - she wasn’t my doctor, but she was a doctor and she looked fairly relaxed and pleasant. I looked at her like a small boy trying to make up his mind whether to take sweets from a stranger. I stood up and walked towards the open door.
Only inside the lair of orthodoxy did I find out two things; firstly that this doctor didn’t speak any English, a pre requisite for me being even partially in control. Secondly and much more alarmingly, she had a nurse aiding her whom I had caught a glimpse of before; she looked like she ate rocks for breakfast, used her hands for chopping up wood and had a face of unpolished granite. Her eyes reflected a kind of dark hatred, perhaps for the human race, maybe for me in particular, men, or even ‘the English’.
It was too late to turn back; before I could even call for help I was in the treatment room. There things went downhill so fast I couldn’t keep my balance. Despite being so young the doctor was ‘old school’ as was the nurse. Realizing that they were going to get nowhere using language, the doctor tried to communicate with sign language while the nurse decided that I had to be pushed around like a rag doll and when it came to lying on the recliner, she pushed me down like a male actor in a bad porn movie.
When I revealed the full bag of urine which was, as it had almost always been, coloured with the darkest red of oxidized blood, the doctor was peculiarly shocked “That’s terrible,” she said, in a sudden concession to broadly accented English “It’s green!” Well, I’ve been an artist for most of my life and unless diabetes has done something terrible to the cones in my eyes, the colour was undoubtedly a brownish muddy red. Of course you always doubt things and I stared at the bag again remembering the green tea I had been drinking over the last week.
They began to get their instruments ready for cleaning out the catheter and my bladder - I should emphasize that, my bladder. The first thing that the doctor tried to do was take off the rubber tube end at the start of the catheter, where it joined with bag piping. However hard she pulled, she couldn’t get it off. Whenever she pulled, I leaned forward and tried to show her how to do it. She wouldn’t hear me. She kept making hand motions for me to lie down. If I had had the language I would have told her in no uncertain terms that on the question of my genitalia, there was no way I wasn’t going to oversee these two. When she began to tire of pulling at the catheter joint, I pushed her out of the way and did it slowly myself, by rolling it off. She watched like a first year student but didn’t smile and showed no gratitude. When that was off, the two of them exchanged enormous plastic syringes and some purified water with which the doctor proceeded to wash out my bladder. I didn’t notice at the time, but she didn’t syringe out this water after she had put it in. I only realized later on the bus back to the interchange, when I began worried about the ballooning ultra-small bag that they had given me. It was filling up so fast that I suspected that it might break sending a sudden tsunami of urine crashing down the central isle of the bus to drown the driver.
So everything was cleaned up and the doctor spoke the words I had been dreading since I awoke at five that morning and for this her English seemed fine, the nurse just looked on gleefully,
“We are now going to change the catheter.” I doubt whether either of them had seen many UK music hall acts of the early 20th century of the “Oh Yes I am” “Oh No you’re not” variety. But they certainly got a good preview now.
She said “We’re going to have to change the catheter.”
I said “Yes but not today.”
She said “Oh Yes, Today.” “Oh No,” I said loudly,
“Oh Yes,” she said faintly,
“Oh No,” I said even more emphatically.
“Why not?” she said with authority but no real interest, I squinted disparagingly at Granite Face, and pointed covertly in her direction, but then realized that I didn’t have the words to express the fact that it would be a frozen night in hell before I let either of them pull out the catheter and stuff another piece of plastic up my penis.
I started to make a move off the ‘couch’ and when Granite Face looked in my direction I shot her a glance that would have stopped a charging elephant. As I started to get dressed I asked the doctor when my female doctor Pilar would be in, and she told me “tomorrow”, so I asked her to make me an appointment because I had to attend tomorrow anyway. I stood around and when I next saw her I asked her what arrangement had been made. “Nine o’clock, here” she said and walked off. So with an early morning appointment with Pilar and then a later one at 15.00, with endocrinology, I knew that I was in for a long day at the hospital tomorrow.
May
Yesterday’s visit to the hospital ended, I thought with the doctor who saw me making an appointment for me to see my female doctor, Pilar, at 9.00 am the next morning. With her I wanted to discuss the changing of the catheter. It was then going to be a long day at the hospital.
I started off at 7am to get the first bus into the city. As I walked to the main road, I began to wonder whether or not I needed to go in to see Pilar. I was happy that my catheter, having been cleaned out, did not need changing. I began to see going in this early as a sign that I was being dragged along in the undertow of the hospital’s plans, rather than making my own.
I got lost in the hospital. When I got to urology it was 9.45 and I was flustered. Pilar was nowhere to be seen. I spoke to one of the nurses, who it turned out didn’t speak a word of English, she spoke to other nurses who also didn’t speak English and gradually I began to lose it.
After about fifteen minutes, as I was nearing breaking point and she was on the edge of throwing herself from one of the unopenable windows, a pleasant looking guy who seemed to be a patient, or a relative stepped up and suggested he translate. He seemed very good and before long we all knew that Pilar was on holiday for a week, so I had woken at 5.00, left the house at 7.00, avoided writing, travelled for almost two hours for absolutely no reason at all.
Just as we were winding up our language seminar, my male doctor, who I thought was in America at a Urology conference, appeared. I quickly went through the whole thing with him; he reassured me about the catheter, that there was no need to change it and when I put it to him that I didn’t really want to sit around until 15.00 hours in the hospital waiting for my consultation in the endocrinology department, he said, “Don’t worry, I’ll get it moved forward for you, just give me a minute”. And that’s what he did; a quarter of an hour later he told me to go to the waiting area of the endocrinology department and wait for another Pilar.
About an hour and a half later I was called into the consulting rooms and found myself sitting opposite three doctors of ages descending from thirty or so to their early twenties. The new Pilar said, “None of us speak English that good, so we thought three of us might be better”. They were all charming although the youngest one seemed to have learned ‘command’ English from Germans, rather than simple conversational English. As I entered the room she said, “Sit”, pointing to a chair; when later I was weighed, she said “stand here”. I wanted to say something to tell her that a looser and warmer approach to the language might show better results, but time went too quickly.
I was totally unprepared for the interview that then began. Pilar was the first person to take a full diabetic case history from me for almost 20 years. At first, having begun my diabetic journey seventeen years ago, I was a bit annoyed at having to go back over everything but when I thought of the relevance I became more relaxed. Could I remember the first symptoms and how they occurred?
When this enquiry was all over they started the more serious business of looking at my blood and urine analysis and the doctor began to give me an opinion. I thought it best to tell them that I wasn’t going to entertain any meds until after my operation. This was the key to my game plan, I would get diagnostic information, have the surgery for my prostate and then do a runner back into my alternative world.
Her first diagnostic statement rocked me back on my heels: “You have your blood sugar reasonable under control”. All I could think is that she had made a mistake in transcribing the figures. After all, I thought, if you don’t believe them when they tell you something bad why should you when they tell you something good. Then she started ticking off things on her fingers - always a bad sign - while the other two younger doctors looked worriedly at me. “Your kidneys have been slightly damaged by your diabetes, you’ll need a med for that.” “Your heart is slightly damaged, you’ll need meds for that.” “Your eyes have probably been slightly damaged, you’ll probably need meds for those.”
After each statement I nodded and said, “Well, let’s get through the operation and then I’ll think about it,” she looked at me suspiciously. “I don’t suppose that there is any point in talking cholesterol,” to which I replied, “Go on, just mention Statins and I’m out the window.”
It seemed it was all over and I wanted to end the session on a lighter note, so I said, “With all this ‘slight damage’ is there any for which you could prescribe me a large quantity of cannabis?” The three of them looked at each other quizzically, unable to quite believe the translation they had done in their heads. “I thought not,” I murmured and then made a more serious point. “I would really like to have my eyes examined.” Pilar immediately made me out a ‘transfer to another department form’ and they all instructed me where to go with it.
This conveyor belt, factory production line seems incredibly efficient for those who have arrived as outpatients or like me were doing a whole body tour of the hospital departments. This, of course, was why your papers are so important; only these and the hospital computers tracked your journey. I was reminded of The Prisoner with Patrick Macgoohan, the late 1960s cult television drama series, of which one web page says: “A man is abducted and taken to what looks like an idyllic village, but is really a bizarre prison. His warders demand information. He gives them nothing, but only tries to escape.”
From the moment you enter hospital as an emergency outpatient, not only does the outside world recede, but both your body and your mind are controlled by the prevailing hospital ideology. Your self and your individuality are abandoned and you are treated as if part of a productive process - ‘faulty’ bodies in, ‘healthy’ or sometimes dead bodies out. Whatever is said, you know that all your relationships and treatments are governed by cost and the efficiency of transit.
On entering The Hospital you are no longer an individual living conscious or sentient organism but simply a body, a mechanical entity. While the rational for this is usually that your condition is an emergency, or you are a lay person, because illnesses are often based on a lifetime of poor conditions and because it is your body that is in question, neither of these rationalizations are exactly true. Ultimately the rational of order within the hospital is as it is with all actions of professionals and all large institutions - firstly: ‘Time and information are of the essence and it is not possible to discuss everything’, secondly, ‘This is our protocol. We do things in this way and we do not allow individuals to break the routine’.
The first conflicts of the mechanisms of orthodoxy with the individuality of the patient occurs with any arguments about treatment modality occurring as a consequence of religious or personal health philosophies. If you are a Muslim, how are you going to raise the alarm about animal derivatives in certain pharmaceuticals? If you have used herbal or homeopathic remedies all your life, how are you going to argue your case, knowing that the hospital will not condone the use of these remedies on their property?
Any argument about alternative modalities is likely to elicit the response I received from a female oligarch: “If you don’t agree with the way we do things, you know where the door is”. How can this be seen as anything other than a paternalistic denial of a patients’ and citizens’ personal freedom of choice, especially when the doctors salary is paid for by the patients tax?
The first sign that your body is no longer your own and its state not to be discussed is when you are given a battery of tests. It’s not so much the tests, it’s the fact that they are given to you without discussion, and the reasons for them, and the results of them will probably not be shared with you. This ‘conflict of interest’ is evident in much smaller ways when, for instance, you routinely have your temperature, blood pressure or blood sugar levels taken. Having taken these measurements the nurse or ancillary worker often walks away without sharing them.
What happens to patients in the modern hospital is that their information is stolen from them. Is this statement absurd? Not in a world where personal gene patterns can be owned by corporations and when one considers the contemporary row in Britain as to whether all patient GP records should be shared with pharmaceutical companies and used for research without the specific patients’ consent.
While medicine is an apparently independent profession, it is actually locked into corporate science and the pharmaceutical industry. Both the profession and the industry share power and in order to protect its hegemony the profession has developed an authoritarian aspect which doesn’t recognize the views of those beyond the profession, most particularly the person whose body is in question. This state of affairs, is partially the arrogance of science, which today feels that it has every answer, and partially a weird leftover from the doctors competitive protection of the 19th century. Of course, it would all be understandable were we considering the workings of the auto engine, but it has a hollow ring when the subject is my, our, or your understanding of and choices over our own health.
Is there a place in a modern health care system for modalities other than corporate pharmaceutical science? Should patients who have used herbs or homeopathy all their lives be subject to the forcible treatment with chemical elixirs when they enter public funded health care? Is socialised medicine simply confined to pharmaceutical treatments or can socialised medicine include any number of modalities that can be chosen by the patient? George Vithoulkas the Greek homeopathic teacher and practitioner, has suggested what others have suggested for diverse use of taxation and choice, that instead of blanket access to State organized health care, individuals should be issued with vouchers which can be exchanged for treatment in a variety of modalities.
It is perhaps important in any discussion of medical orthodoxy to make clear those areas in which it excels. High on this list must be the administration of crisis or emergency care following accidents of all kinds. This is followed by the onset of a health crisis in circumstances where there has been little or no warning of a developing illness. After this, even within the hospital, there is clearly a place for combining or solely using alternative health care modalities in many circumstances.
‘Scientific and pharmaceutical medicine’ gradually gained a determining role in this paradigm in the years after the second world war. For the pharmaceutical companies, the oncoming universal structure of the health service with its network of General Practitioners and centralised hospitals, was a Godsend. The infiltration of the NHS in Britain was achieved by a number of different covert routes. The early Medicines Division, for instance, the first regulatory department of the NHS, worked hand in glove with the pharmaceutical companies and had a revolving door policy on staffing.
In the 1970s and 1980s, the pharmaceutical companies had infiltrated parliament and begun to influence policy and by the end of the century, the privatization of the NHS was in full swing with chunks of it being handed to health care and pharmaceutical corporations. The charities campaigning on behalf of individual diseases are mainly funded and organized by pharmaceutical companies which influence, and mediate trials and treatments between individuals and hospitals, ensuring that only pharmaceutical medicines are used in most illnesses.
This developing health care system, although appearing to be a beacon of altruism, actually exhibited all the signs of socialist or even communist organization. This form of organization deprived the patient of choice, self-education and makes them dependent subjects without initiative.
While it is possible to blame the corporate producers of pharmaceuticals and health care for the still developing lack of modality choices, a note has to be made about the inability of alternative health modalities to create an independent cohesive health care system which contains centralised institutions like hospitals or even community health centres. There are two sides to this: lack of initiative on behalf of ‘alternative’ practitioners and an overweening lust for power and profit on behalf of the medical profession and their corporate industries.
The modern national health care system in Europe grew out of the intention of socialists to create a universal health care system which was free at the point of delivery and which catered for everyone, regardless of their financial circumstances. Of course, although this was principally an altruistic progress, it was pushed forward originally by the state - the more cynical might say - to ensure a healthy workforce and more recently by pharmaceutical corporations whose main consideration is profit. Over the last one hundred years there has been a progressive and quite positive strategy of the state, corporations and medical professionals, especially in the UK, Europe and the US to wage war with alternative treatments, from homeopathy to chiropractic, and to ensure hegemony of ‘orthodox’ pharmaceutical medicine.
The gradual erosion of the homeopathic model was aided by the decline of the aristocracy, who had throughout the 19th century been the major patrons of the practice and of the idea of private and personal medical care. The aristocracy of the nineteenth and early twentieth century had the same distain for a State medical system that Sherlock Holmes had for the State police force.
The survival of organized alternative health care, using modalities which are in conflict with orthodox scientific medicine grow and develop most energetically where they are a function of community. This can be seen in relation to a number of practices within communities like the Amish or certain South East Asian indigenous cultures and Cuba which has been forced mainly for financial reasons to consider alternative practises. Even in some European countries, such as Germany, a large percentage of doctors embraces holistic practices. The second factor, is that in the UK and other European countries, alternative practitioners have tended to be too concerned with their own professionalization, too timid and respectful of the law and personal status to be offensively propagandist.
Practices such as homeopathy will only begin to embed themselves socially again, becoming viable alternatives, when adherents form communities with alternative values, covering the whole spectrum of life style, nutritional and social organisation. Just as ‘scientific’ medicine is embedded in bourgeois ‘scientific’ society, ‘alternative’ medicine has to be embedded in an organic alternative society.
Quiet clearly, globalism and the advance of technology and science present a formidable opposition to community and alternative community practices like alternative health care. Ultimately the same spare part will be used in London and Moscow, the same mechanistically affecting pharmaceutical in Paris and Hong Kong. Scientific medicine works without intimate knowledge of the patients individuality and the hospital can be seen as a warehouse for a damaged nomadic population seeking repairs.
Centres for alternative medicine will need to be based in health safe residential communities where practitioners have, known, tracked and continuously worked with patients over long periods, perhaps even with the same practitioners, who rather than a computer is familiar with the citizens’ personal information.
* * *
The hospital I attended is one of the biggest and most modern in Europe; light rebounds from all its shiny surfaces, there is no humanity in the building, its materials or its structure. But perhaps most frustrating, there is no room for individuals in such a hospital. There is no time for discussion or the seeking of personal truth. Because of the method of treatment implicit in scientific medicine, most especially the principle of treating bits of the human body quite separately from the whole, there is no room in the hospital for individual treatments. And because of the reliance of doctors and the economy of the hospital on chemical drugs, there is no room for alternative treatments of any kind.
Being English, born in the baby boom years after the second world war and growing up independently as a socialist, (now an anarchist), I had as I began my adult life a particularly English view of the socialised medicine and the National Health Service (NHS). This view suggests an idea of a health system, which financed by taxpayers, made UK health care universally available and free at the point of delivery.
Initially, despite low level disruption from surgeons who wanted to remain ‘private’ the people were offered an accessible health service across the board. However, increasingly less mentioned was the content of the health care provided, As corporate society grew and public spending was diverted in numerous ways, the content of health care, no longer free at the point of delivery began a descent into the deep pockets of the pharmaceutical companies, corporations that were to become the richest in the world and whose edict stretched through medical education and into the soil of medical culture and whose products became the coinage of all treatment.
In the NHS that developed in the seventies, self-health was frowned upon and in some circumstances forbidden, while expressing opinions in opposition to professional medics and general practitioners became something which ‘just wasn’t done’. No longer any mention of the effect of food or nutrition, except that which was advocated by the food corporations, no longer any mention of herbs or herbal remedies and increasingly less availability of them. Self-health in the UK was reduced to commercial ideas about exercise, gyms, and the avoidance of toxins apparently found in alternative medicines.
To an anarchist, a homeopath or even an individualist who believes in community, the initial response to being faced with the corporate state in all its forms is fairly simple, and that is to exempt oneself as far as is possible from the texture of the corporate State centred society and live with as much rational individuality as seems possible. The problems and confrontation, however, occur when urgent or unforeseen needs cannot be remitted within the community and only the State has the facilities to be helpful.
The struggle for alternative, socialised health care is in part a struggle against advancing technology and the robotization of the human form. It is part of the struggle against the corporate control of our lives on a number of different levels. It would be difficult to pursue alternative socialised health care without forming communities that rejected harmful advanced technology and poor quality health-draining denatured foods. Massive questions raise themselves in a globalizing world, such as the need to form communities in which members relinquish the need for constant travel or the need to settle in foreign parts for long periods. Those who believe in alternative modalities have to begin to break out of the medical ghetto into which we have been forced by Allopathy and begin consider socialised holistic health as an aspect of community, rather than as a mechanism for private profit. Ultimately those who believe in alternative medicine have to think politically.
Comments:
-
No Article Comments available
