Positive Health Online
Your Country

Massage and Cancer-Related Fatigue: Benefits and Cautions
listed in massage, originally published in issue 213 - April 2014
One of the most common symptoms associated with cancer and its treatment is fatigue. For many people, it is the major troubling symptom and the primary cause of distress, being even more problematic than pain, nausea, or vomiting. Fatigue can interfere with the completion of treatment, lower quality of life, and reduce the ability to function fully.
| Cancer treatment leaves a footprint on nearly everyone who experiences it. Many interventions, such as massage, can soften the indent of the marks left behind. Fatigue is but one of many side effects that can be helped through touch therapies, as well as chemotherapy-induced peripheral neuropathy, cording, lymphedema management, scarring and adhesions, and emotional and body image issues. |
The majority of those in treatment, not surprisingly, must contend with fatigue. However, cancer-related fatigue (CRF) also can persist for months or years following treatment, even being present in high numbers of people five years and more afterwards. Patients often perceive fatigue as something that must be endured or cannot be addressed by their doctors, therefore, they underreport it, which leads to under-treatment.[1-4[ While there are medications that reduce or control some of the side effects of cancer and its treatment, such as nausea, pain, and neutropenia, there is no ‘fatigue pill’.
Massage and other complementary and alternative therapies (CAM) have an important contribution to make in the area of fatigue. Some scientific research has explored the efficacy of massage on fatigue during cancer treatment, particularly chemotherapy. As well, a great number of anecdotes from patients indicate that massage, properly adjusted to meet their specific needs, improves energy levels in addition to other symptoms, such as pain and anxiety, and sometimes nausea, insomnia, and appetite.
The purpose of this article is three-fold: to examine
- The prevalence of cancer-related fatigue;
- How massage might be beneficial to people affected by fatigue and;
- The adjustments that need to be made to the massage sessions for people experiencing CRF.
Defining Massage
Before continuing, let’s define massage. A typical definition states that massage involves manipulation, rubbing, and kneading of the muscles and soft tissue to enhance function of these tissues and promote relaxation. Bodywork such as this is too vigorous for many people affected by cancer treatments. For the sake of this article, massage is defined as “any form of systematic touch.” A broad perspective, such as this, allows all people to receive some sort of touch therapy, no matter where they are in their cancer experience - treatment, recovery, survivorship, or end of life.
There is no clinical reason ever to refuse massage to a person who has had cancer or is in treatment for it. Some therapists may not feel well enough trained or experienced to work with these clients, which is a fair reason to decline massaging someone affected by cancer. The hope, however, is that the therapist would refer the client onto another practitioner who is appropriately schooled in the needs of people living with cancer. To be turned away, when booking a massage session, is very hurtful to people wanting to ‘feel normal’ for a day. If a therapist feels poorly trained to work with these clients, the best action is to explain to the person wanting massage that, “Touch therapies are very beneficial to people with a history of cancer, but that I am not experienced or trained in the adjustments needed in this situation.”
Unfortunately, many years ago, a misconception grabbed hold within the bodywork profession, which believed massage could cause cancer cells to spread. For the most part, this myth has been dispelled. It is now known that cancer starts and spreads because of genetic mutations. Cancer cells do not spread because of the mechanical force of a massage or exercise or even the activities of daily living.
No one needs to be prevented from receiving the nurturance of touch therapy because of the treatments or the disease. What is needed is adjustment to the components that make up a massage session. The pressure usually needs to be decreased, especially where fatigue is present, certain areas may need to be avoided due to incisions, medical devices, or pain, and clients may need to experiment with finding a position on the massage table that is comfortable for them. But, everyone can receive massage therapy in some way or form, even if it is only a foot or head massage.
Let’s explore fatigue at three varying points along the cancer treatment spectrum - treatment, recovery, and long-term survivorship. The adjustments at each stage will differ to some degree, depending on where the person is along the timeline.
Fatigue During Cancer Treatment
The causes of fatigue during treatment vary. It may be due to inflammation, a low red blood cell count and thus poor oxygenation, organ toxicity, endocrine imbalances, or an over-burdened lymphatic system, just to name some. Breakdown of the tumour via chemotherapy or radiotherapy releases the constituents of the cells into the circulatory system, which must then be cleared through the normal metabolic pathways. Healthy cells are also affected by each of the three forms of treatment, requiring repair to the tissues. All of these metabolic processes call for an energy output, whether the cause is surgery, chemotherapy, or radiation. Other factors, such as medications can contribute to fatigue, decreased activity can create lethargy, and there are a host of psychological variables that bring a person’s energy down, such as fear, hopelessness, or feeling out of control.
The main contributing factor to side effects such as loss of vigour, pain, reduced function, or low blood cell counts, is treatment, rather than the disease itself. This is not to say that the cancer doesn’t, at some point, cause such symptoms as fatigue, blood clot risk, or low blood counts. However, for much of the time, the massage adjustments centre around the side effects of treatments. The three main forms of treatments still are surgery, chemotherapy, and radiotherapy.
Surgery
Surgery or a tissue biopsy is often the first part of the treatment process, although sometimes radiation or chemotherapy is the starting point so that the tumour can be shrunk, making the surgery less invasive. Those whose treatment only involves surgery will experience fatigue and require rest for an undetermined period of time. A fast surgical recovery is five to six weeks, but many people take months and months to recover, even a year. Until clients return to their pre-diagnosis energy level, the massage pressure should be adjusted downwards to match the person’s degree of vigour. The goal is help them feel more energetic, not as if they were flattened by a steamroller, which is what can happen when the massage pressure is too forceful.
Chemotherapy
Chemotherapy treatment causes energy patterns to wax and wane over a long period of time. Usually, fatigue accumulates over the months, dropping lower with each round of drugs, especially with intravenously (IV) administered cancer-killing medications. A chemotherapy schedule may consist of four to eight rounds, also known as ‘cycles,’ over many months. A chemo cycle is often three weeks in length, but it may also be one or two weeks long. Following chemotherapy, the patient’s level of energy will decrease in a pattern that is associated with blood count drops. If the cycle is a three-week in length, the low-point in the blood counts, or nadir, will occur near the mid-point on days 10 and 11, after which time the person will experience a partial improvement in their energy. However, it is seldom the client’s usual level of energy.
Radiotherapy
Radiotherapy affects people differently with regard to fatigue. Some people breeze through, while others find radiation affects their vitality more than chemotherapy. The field of treatment is one influencing factor. For instance, patients receiving radiation to the head and neck, or to the area that includes the gastrointestinal tract, will find their ability to eat and digest food is diminished, which leads to fatigue. If the field of treatment includes areas such as the hips or sternum, where significant amounts of bone marrow is produced, the red blood cell count can be affected, which leads to poor oxygenation.
When can Patients in Treatment Receive Massage?
Surgery
Surgical patients often benefit from massage just before going to surgery. It reduces anxiety, which in turn affects a person’s energy. And, they can have gentle touch after returning from the recovery room to their hospital room. In either of these cases, before or after surgery, massage does not look the same as a session in which the person books in with a private therapist. The touch may just be to the hands, feet or head. As session of light bodywork following surgery can make people feel more alert as well as reduce discomfort caused by the position of their body on the surgical table. Because there is an interrelationship between pain, anxiety, and nausea and fatigue, an intervention that lowers one will affect the other. Reducing pain, reduces fatigue. Reducing nausea, reduces fatigue. Notice Figure 1, this patient had surgery to her right foot in the morning, by the afternoon she was having massage on the one available part of the body, the left foot.
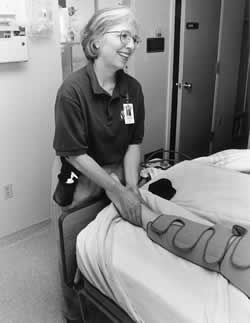
Figure 1
Chemotherapy
Chemotherapy patients can receive massage at any part of the chemotherapy cycle. Some people like to receive massage during the infusion process. The patient in Figure 2 is receiving chemotherapy and foot massage at the same time as crocheting. Gentle massage induces relaxation during a stressful process, leaving people more energetic afterwards. One client found it was helpful to come in for a full-body massage immediately after chemo infusion. Her energy improved by about 50% versus the times when she received no massage after chemotherapy treatment. This extra energy was important to her, as she was the mother of a 4 year-old.

Figure 2
Some people prefer to wait for a few days after receiving chemotherapy while others like to have massage at the very end of the cycle because they feel at their best at this time and can enjoy the session more.
Radiotherapy
Except during the actual administration of the radiation, a person can receive massage at any other time. Many people prefer to receive touch therapy after their radiotherapy session. This allows them to release the tension in their body after lying so still during the treatment. Relaxing the muscles increases a person’s energy by allowing deeper respirations, which increases oxygenation. A relaxed musculature also allows fuller circulation within the body and delivery of nutrients. Gentle massage stimulates the parasympathetic nervous system response, slowing the heart and the breath, encouraging digestion, calming the adrenals, and many other responses. The patient in Figure 3 has just come out of the radiotherapy suite after undergoing treatment to the brain. She is receiving a gentle 15-minute seated massage to help her rest and relax.

Figure 3
Scientific and Anecdotal Evidence
While there is not yet overwhelming scientific evidence that massage has a positive effect on fatigue, clients frequently report increased energy for a handful of days following bodywork sessions. They report being able to run errands, shop, exercise, clean the house, garden, and spend time with family. Massage also provides clients with a sense of participation in and control of the healing process, and for some, it helps them get through the rigours of cancer treatment.
Neither mainstream medicine nor complementary and alternative medicine has sufficiently researched the problem of fatigue to find interventions that might improve a patient’s vigour. The massage research bears this out. The majority of studies have looked at pain and anxiety, followed by nausea and vomiting. The effect of touch therapy on fatigue has received minimal research with people in treatment, almost no study with those in recovery, and no examination of massage and the fatigue of long-term survivors.
One of the most strongly designed studies is by Post-White et al.[5] A sample of 164 patients receiving chemotherapy were divided into four groups - Swedish massage, Healing Touch, presence, and standard care. Only the Healing Touch group had a decrease in fatigue Other studies proved to reduce fatigue, however, the experimental designs were lacking. Cassileth and Vickers[6] reported a 41% improvement in fatigue in 1290 Memorial Sloan-Kettering patients whose data was examined retrospectively. Yang,[7] Hernandez-Reif et al.,[8] Kite et al.,[9] Ahles et al.,[10] Tsang et al.,[11] Pruthi et al.,[12] and Currin[13] also produced positive outcomes, but each lacked strength in the research or analysis design. Only Wilkinson’s team[14] found no difference in fatigue levels between a usual care group and an aromatherapy massage group.
An examination of the above studies to one another is like comparing apples to oranges. A variety of modalities were used: Swedish massage, aromatherapy massage, Reiki, seated massage, and reflexology. Some of the subject groups were hospitalized patients, others were outpatients, many in one group were receiving radiotherapy, another group was receiving chemotherapy. Most of the interventions were delivered by professionals with the except of Zick et al.[15] In their study, cancer patients were taught to administer a reflexology treatment to themselves. All three experimental protocols were affective on fatigue.
An optimistic trend does seem to be surfacing where fatigue and bodywork are concerned. One thing that the existing studies show, despite their lack of rigour, is feasibility; it is possible for people in cancer treatment to safely receive massage from practitioners trained for the individual needs of people affected by cancer. Many years of experience by myself and many colleagues, shows that the following adjustments are necessary for people receiving massage during the treatment phase:
|
Massage Adjustments for People in Cancer Treatment
|
Fatigue During the Recovery Period
The oncology literature contains a clear definition of the word ‘survivorship’ but it does not spell out the ‘recovery period’ in the same way. For our use in this article, it will be considered the time after treatment ends until a person’s symptoms have begun to abate significantly and a new normal has been found. This is subjective at best, but gives some boundaries to this time period.
Patients and their family anticipate the end of treatment, assuming that they will be able to return to their old life, only to discover that their former life no longer exists. Disappointment, uncertainty, and depression can set in. It takes time to realize that a new normal must be found, that there is no moving backward, only forward into who they are now.
Massage practitioners, too, must realize that it takes time for a client’s side effects to heal and that at first, touch therapy sessions must continue on with nearly the same adjustments as during the treatment period. Just because treatments have stopped, it doesn’t mean the side effects have stopped. Think about the time it takes for a cut finger to heal, a simple cut finger. Immediately after the injury, platelets gather to form a clot. Inflammation occurs as bacteria and debris are disposed of. New blood vessels form, collagen is deposited, granulation of the tissue occurs, all of which require complex biochemical processes. Accidently slicing a finger can take months and months to fully heal. Imagine how long it takes the body to heal after the removal of an organ, multiple sessions of radiation, or months of chemotherapy.
Bodywork has much to offer the depleted person, but it requires the right adjustments to the pressure. It is important that client and therapist approach massage at this point as an intervention to build and support the recovery rather than one that tears down or detoxifies. Eventually the person will recover enough vitality to be able to participate in more demanding methods.
Gauging the level of demand massage has on a cancer client’s body is difficult for both the client and the therapist. Patients who have received massage prior to cancer treatment mistakenly believe they can tolerate the same type of bodywork sessions as before. Usually, that is never the case, ever. Even the most robust of clients find that they must modify their activities as they are recovering from treatment. But, by finding just the right amount of pressure, length of session, and pace, the therapist can provide the most beneficial level of support.
Remembering that many of the side effects of treatment cannot be seen on the surface, the therapist must use other guideposts in order to gauge the appropriate level of demand. Appearance often cannot be used as a signpost because some patients can appear healthy on the outside. In fact, bodyworkers must be cautious not to read too much into a client’s bright facade. Instead, the following three areas can be more precise in gauging how demanding the massage can be:
- Activities of daily living. Are they preparing meals again, resuming work or volunteer activities? Part-time? Full-time?
- Housework capacity. As energy improves, people are able to return to housecleaning and gardening. However, it is like exercising, the return is in increments and the step they are on will indicate their level of recovery;
- Exercise level. This can tell a practitioner a great deal about how much the body can tolerate. However, do not assume that if the client is able to walk several miles or that she is working out in the gym, that it means the massage does not need to be moderated. It still needs to be tempered.
There is very little in the oncology massage research to direct therapists working with clients recovering from cancer treatment. Listing et al.[16] tested 30-minute massages twice a week for two weeks in a randomized, controlled trial of 86 German breast cancer patients who were at least three months out of chemotherapy or radiation. Immediately following the intervention period and six weeks afterward, the massage group had a significant drop in fatigue.
An accumulation of anecdotal evidence offers the best guidance for now. A few simple guidelines have surfaced as a result of many years of massage with people recovering from cancer treatment:
- Start at the low-impact end of the spectrum;
- Inch forward in incremental steps;
- Less is more.
|
Massage Adjustments for People Recovering from Cancer Treatment
|
Fatigue and Long-Term Survivorship
Fatigue is a universal problem for people with cancer, not just for those undergoing treatment but also for long-term survivors. There is a lack of understanding of the reasons behind cancer-related fatigue (CRF). The list of possible factors is long and includes anaemia, pain, endocrine problems, medications, insomnia, lack of exercise, poor nutrition, a chronic inflammatory process, depression, and permanent vital organ complications.
One often-cited study by Bower and her team of researchers[4] looked at the incidence of fatigue in 763 women treated for breast cancer who were subsequently disease-free. One to five years later, 35% were classified as fatigued. Of another group of breast cancer survivors who were five to ten years post-treatment, Bower et al. found that 34% were classified as fatigued. In their review of the literature on cancer-related fatigue, Campos and colleagues[17] report on a group of Hodgkin’s Disease patients who had been disease free for five years. Sixty percent in the survey were fatigued. A British multi-site survey also found 60% of cancer patients affected by fatigue, which was nearly three times greater than the reports for pain and nausea/vomiting. Half of the patients surveyed had never reported the fatigue to their doctor, thinking it was something they just had to live with.[2]
Not just quality of life is affected by cancer-related fatigue. Studies have linked increased levels of depression, anxiety, and mood disturbances to CRF. It has been shown to have significant effect on employment and financial status. Not only is the economic impact felt by the cancer survivor, it also extends to caregivers and family members who have to reduce work hours in order to provide care.
Because CRF is not well understood and because patients often underreport it, health care providers are not able to treat it with any precision. Some, but not all causes of fatigue may be improved through medications, nutrition, exercise, psychological interventions, or the use of CAM modalities. Clients regularly report their energy is improved as a result of bodywork. However, no scientific examination has been made of the effect of massage on people who are long-term survivors. Nothing is known about the immediate influence touch therapies might have on fatigue or how long the affect might last. In light of the life-altering effects of fatigue following treatment, clients who are one to five years post-treatment, and five to ten years, need to be studied to see what contribution manual therapies can make in improving their quality of life.
|
Massage Adjustments for Long-term Cancer Survivors Bodywork has a great deal to offer the person with cancer-related fatigue if the session is appropriately adjusted. No matter if the fatigue is treatment-related or is a lingering side effect, it is a pressure caution. Determining a client’s energy level, and thus the appropriate pressure, is complex. Levels of exercise, house or garden work, the ability to participate in employment or social life, can be an indication of vitality. Enquire if the client has to manage or monitor their energy output more closely than before treatment. Therapists need to be aware that when asked about their level of vigour, clients will often answer with, “Good,” or “Fine.” However, they are sometimes comparing it to their energy during treatment, which was very low. Try to hone in on their present activity level. |
Final Thoughts
Cancer treatment leaves a footprint on nearly everyone who experiences it. Many interventions, such as massage, can soften the indent of the marks left behind. Fatigue is but one of many side effects that can be helped through touch therapies, as well as chemotherapy-induced peripheral neuropathy, cording, lymphedema management, scarring and adhesions, and emotional and body image issues. Other side effects cannot be helped by massage, such as osteoporosis, heart damage, bone pain, or ascites, but neither do these side effects get in the way of a client receiving some type of massage. Everyone with a history of cancer or cancer treatment, wishing to, can receive touch therapy.
References
1. Holley SK. Evaluating Patient Distress from Cancer-Related Fatigue: An Instrument Development Study. Oncology Nursing Forum. 27(9):1425-1431. 2000.
2. Stone P, Richardson A, Ream E, et al. Cancer-related fatigue: Inevitable, unimportant, and untreatable? Results of a muti-centre patient survey. Annals of Oncology. 11(8):971-5. Aug 2000.
3. Hofman M, Ryan JL, Figueroa-Moseley CD, et al. Cancer-Related Fatigue: The Scale of the Problem. Oncologist. 12Suppl 1:4-10. 2007.
4. Bower JE, Ganz P, Desmond KA, et al. Fatigue in Long-term Breast Carcinoma Survivors. Cancer. 106(4):751-758. 2006.
5. Post-White J, Kinney ME, Savik K, et al. Therapeutic Massage and Healing Touch Improve Symptoms in Cancer. Integrative Cancer Therapies. 2(4);332-44. 2003.
6. Cassileth BR, Vickers AJ. Massage Therapy for Symptom Control: Outcome Study at a Major Cancer Center. Journal of Pain and Symptom Management. 28(3):244-249. 2004.
7. Yang JH. The Effects of Foot Reflexology on Nausea, Vomiting and Fatigue of Breast Cancer Patients Undergoing Chemotherapy. Taehan Kanho Hakhoe Chi. 35(1):177-85. 2005.
8. Hernandez-Reif M, Field T, Ironson G, et al. Natural Killer Cells and Lymphocytes Increase in Women with Breast Cancer Following Massage Therapy. International Journal of Neuroscience. 115:495-510. 2005.
9. Kite SM, Maher EJ, Anderson K, et al. Development of an Aromatherapy Service at a Cancer Centre. Palliative Medicine. 12:171-180. 1998.
10. Ahles TA, Tope DM, Pinkson B, et al. Massage Therapy for Patients Undergoing Autologous Bone Marrow Transplantation. Journal of Pain and Symptom Management. 18(3):157-63. 1999.
11. Tsang KL, Carlson LE, Olson K. Pilot Crossover trial of Reiki Versus Rest for Treating Cancer-Related Fatigue. Integrative Cancer Therapies. 6(1):25-35. Mar 2007.
12. Pruthi S, Degnim AC, Bauer BA, et al. Value of Massage Therapy for Patients in a Breast Clinic. Clinical Journal of Oncology Nursing. 13(4):422-425. 2009.
13. Currin J, Meister EA. A Hospital-based Interventions Using Massage to Reduce Distress Among Oncology Patients. Cancer Nursing. 31(3):214-221. 2008.
14. Wilkinson SM, Love SB, Westcombe AM, et al. Effectiveness of Aromatherapy Massage in the Management of Anxiety and Depression in Patients With Cancer: A Multicenter Randomized Controlled Trial. J Clin Oncol. 25(5):532-539. 2007.
15. Zick SM, Wyatt GK, Murphy SL, et al. Acupressure for persistent cancer-related fatigue in breast cancer survivors: a study protocol for a randomized controlled trial. Epub 2010. Available at: www.ncbi.nim.nih.gov/pubmed/22909076 . Accessed Oct. 16, 2013.
16. Listing M, Reisshauer A, Krohn M, et al. Massage Therapy Reduces Physical Discomfort and Improves Mood Disturbances in Women with Breast Cancer. Psycho-Oncology. 18(12):1290-1299. 2009.
17. Campos MPO, Hassan BJ, Riechelmann R, et al. Cancer-related fatigue: a practical review. Annals of Oncology. 22(6):1273-1279. 2011.
Comments:
-
No Article Comments available