Positive Health Online
Your Country

Rise in Private Healthcare, in Part Driven by Covid
by Hannah Whitehouse(more info)
listed in insurance, originally published in issue 275 - January 2022
After 19 months of stress, uncertainty and seemingly endless restrictions, the world is gradually opening up again. Lockdown rules, such as caps on indoor gatherings and mandatory mask-wearing in enclosed spaces, ended on the 19th of July 2021. Since then, the government has eased travel restrictions, and hospital admissions for Covid-19 have steadily declined. But while most of us start to enjoy some much-needed normalcy, there’s one area that shows no such signs of recovery – The NHS waiting list.
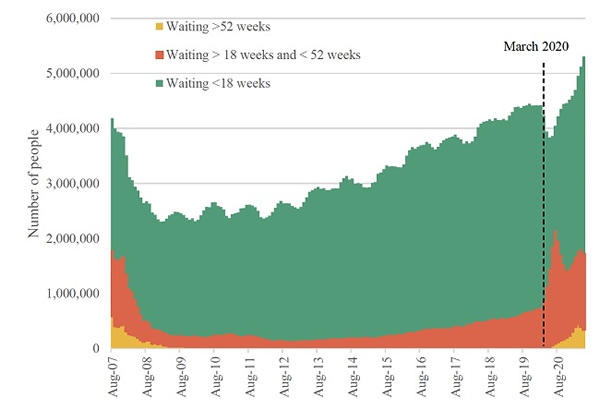
The Current State of the NHS Waiting List
While there's no denying that the National Health Service has done an incredible job responding to the Covid-19 crisis, the NHS waiting list has long been a sticking point. Prior to the pandemic, as many as 4.4 million people were awaiting treatment in the UK. In September, the media reported that this figure had climbed to 5.6 million – the highest record since numbers were first taken in 2007. An inevitable side effect of such a large backlog is that people face long waits to be seen by a specialist or admitted for surgery. According to the most recent data, 1.8 million people waiting for care in July had already waited at least 18 months, while 7,980 had been waiting for more than two years.
As a result, the government has been tasked with answering difficult questions, including how much longer the waiting list could get. According to Health Secretary Sajid Javid, the answer is that the backlog will “get a lot worse before it gets better”. In terms of what that could look like, the statistics indicate that the waiting list could double by the end of the year, while future predictions cap it as high as 13 million.
Among the government’s plans to tackle this problem is paying private healthcare providers to administer treatments to non-Covid patients. Indeed, it’s not the first time we have seen this come to pass. In March 2021, NHS England partnered with the private sector to carry out millions of emergency treatments for cancer, stroke and heart patients and free up NHS capacity to treat patients with Covid. This deal, the first of its kind, included the provision of 8,000 beds, 1,200 ventilators and nearly 20,000 staff.
However, even with support from private hospitals, the grim reality is that patients on the NHS waiting list are unlikely to receive the treatment anytime soon. Perhaps the hardest pill to swallow is not the prospect of a long wait but spending so many months or years in pain and discomfort. While a patient is waiting for a non-urgent procedure such as a cholecystectomy, they might suffer frequent gallbladder attacks that cause severe pain, sometimes lasting several hours. Those waiting for joint replacement surgery, such as arthroplasty, might be in agony every day, which impacts their quality of life.
Added to that is a harsh disparity between NHS treatment times even for common procedures such as knee, hip and eye surgery. Covid does play a part, with areas badly hit suffering larger queues, but deprivation, age and population are also sizable factors. The result is that patients are left playing a postcode lottery and face longer waiting times based on their location, even when operations are more readily available just a few miles away.
It’s perhaps not surprising, then, that independent hospital groups are seeing demand soar.
According to David Hare, chief executive of The Independent Healthcare Providers Network, many can no longer afford to wait months, if not years, for treatment.
We know that the global pandemic has been a major contributor to waiting times. During the recent wave in January 2021, 4,134 people were admitted to hospital with the virus. The need for many frontline workers to self-isolate has only compounded the shortage of NHS staff.
Several hospitals were also forced to cancel planned operations due to an influx of Covid patients.
But waiting lists have always been long, which begs the question, is there another reason?

The Change in Attitude Towards Health
A recent study by GSK Consumer Healthcare and IPSOS has revealed that attitudes around self-care and overall health consciousness have shifted during the pandemic. In the UK, 77% of those surveyed considered it important to take charge of their health to relieve pressure on the NHS, while three quarters are now more concerned about the health of their loved ones. Overall, it becomes clear that patients are no longer willing to wait for the care they need, nor do they want to burden our health service at such a critical time.
Of course, we’re still not out of the woods with Covid, either. We don’t know what the future might hold, especially as we approach the winter months, and legitimate fears still exist over accessing public healthcare.
In contrast, private hospitals are uniquely equipped to handle increased demand, thanks to higher budgets. Many also boast “Green Zone” status, denoting that there has been no new local transmission of coronavirus for at least 14 consecutive days.
For our now more health-conscious public, the benefits of private healthcare outweigh the cost. At a private hospital, an individual can have an operation and be on the road to recovery in mere weeks – or even days – while freeing up capacity for the NHS to treat Covid and non-Covid patients alike.
Other benefits include more one-on-one attention from consultants and luxury settings, such as a private room. For those who need surgery but are concerned about the risks of going to hospital, access to private facilities can be a deciding factor.
It’s important to note that the rise in private healthcare is in no way related to perceptions around quality of care. Many medical professionals operating in the private sector work simultaneously within the NHS, and while the level of care in a private setting may be perceived as “better” due to modern and comfortable facilities and doctors’ increased capacity to build rapport with their patients, all doctors, regardless of where they work, are bound by the same strict regulations.
How Patients Are Funding Private Healthcare
Amid a pandemic that has changed the world economy, how are people financing private treatment?
Despite treatment costs potentially running into the thousands, self-paying is an increasingly popular option, especially where patients have pre-existing conditions that most health insurance plans don’t cover.
Others are also cutting treatment costs by mixing and matching, such as going private for a much-needed operation and receiving physiotherapy via the NHS during recovery, or having diagnostics done by the NHS and then being referred to a private hospital for surgery. While cost is still a crucial consideration, for many, it’s one worth paying, and the benefits of people taking charge of their health during an especially turbulent time cannot be understated.
Whether a two-tier system, where the NHS is a residual service for those who cannot afford to pay for their own treatment, is a likely scenario in the future is unknown. However, one thing is certain: with the NHS backlog continuing to grow, the trend of more patients opting for private healthcare shows no signs of slowing.
References
- Daily summary | Coronavirus in the UK, https://coronavirus.data.gov.uk/
- Record 5.6m people in England waiting for hospital treatment, https://www.theguardian.com/society/2021/sep/09/record-56m-people-in-england-waiting-for-routine-hospital-treatment
- Sajid Javid’s warning of a 13 million NHS waiting list is well within the realms of possibility, https://ifs.org.uk/publications/15560
- NHS England » NHS strikes major deal to expand hospital capacity to battle coronavirus, https://www.england.nhs.uk/2020/03/nhs-strikes-major-deal-to-expand-hospital-capacity-to-battle-coronavirus/
- NHS backlog disproportionately affecting England’s most deprived, https://www.theguardian.com/society/2021/sep/27/nhs-backlog-disproportionately-affecting-england-most-deprived
- Paying for private surgery: how much common operations cost if NHS waiting list is too long, https://www.lovemoney.com/guides/113052/private-healthcare-uk-costs-to-expect-nhs-package-plans-fee-per-service
- COVID-19 prompts increased focus on self-care, https://www.gsk.com/en-gb/media/press-releases/covid-19-prompts-increased-focus-on-self-care-with-europeans-taking-their-health-more-seriously-to-relieve-pressure-on-healthcare-systems/
- Private hospitals profit from NHS waiting lists as people without insurance pay out, https://www.theguardian.com/society/2021/sep/18/private-hospitals-profit-from-nhs-waiting-lists-as-people-without-insurance-pay-out
Comments:
-
No Article Comments available