Positive Health Online
Your Country

Acid-Base Balance: Indispensable for Our Metabolism
by Dr Helga Handschuh(more info)
listed in cellular chemistry, originally published in issue 133 - March 2007
Acid-base balance is one of the regulation systems needed by the human organism for its survival. Thanks to a finely-attuned interplay between acids, bases and buffer systems, it creates a balance, without which cell functions and metabolic reactions would not be able to run smoothly. In addition to disturbances in the body’s buffer systems, there are other influences that can upset this sensitive balance, resulting in manifest or latent acidosis. Thanks to scientists such as Ragnar Berg and Friedrich Sander, even latent acidosis can now be diagnosed in good time.
“We should eat five to seven times more potatoes, fruit, root and other vegetables than all other foodstuffs put together, eat a portion of raw vegetables every day and drink no more than half a litre of milk a day”.
These health-maintaining recommendations do not stem from any modern scientist; in fact, they were drawn up at the beginning of the 20th century by the Swedish nutritional researcher, Ragnar Berg (1873-1956). Berg was not concerned with secondary plant compounds which are nowadays so intensively studied, but rather the absorption of alkaline mineral substances needed to regulate acid-base balance. Thus, he was the first scientist to recognize the significance of acid-base balance in the human organism’s ability to function.
Moreover, modern Natural Medicine has to thank the Doctor and Chemist Friedrich Sander for most of the knowledge it possesses today, in terms of categorized forms of acidosis and acid-base phenomena occurring within the body. Based on his comprehensive biochemical, physiological and clinical trials in this field, he was able to demonstrate that a metabolic shift toward latent acidosis can be seen not only in a high percentage of acute pathological processes, but also in the majority of chronic degenerative diseases, as well as many chronic Western diseases. Sander summarized his research findings in a book published in 1953 under the title Der Säure-Basen-Haushalt des menschlichen Organismus (Acid-Base Balance in the Human Organism), which, even today, is still considered to be the gold standard for acid-base research.

Acid Metabolites
During every second of our lives, countless biochemical reactions occur in the human metabolism, in which fats, proteins and carbohydrates are consumed to produce energy. These processes are catalyzed by enzymes, which can only work flawlessly in the presence of certain optimum pH values within our cells. These values vary from organ to organ. As acid metabolites constantly accrue during cell metabolism, a finely-attuned interplay between various buffer systems ensures that the physiological pH value is nevertheless accurately maintained.
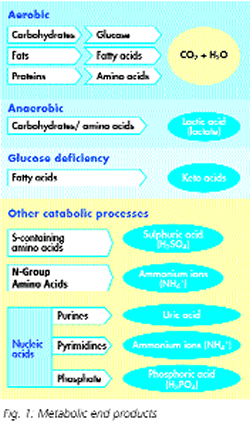
During normal metabolic processes, the following (often acidic) metabolites are formed:
- Carbonic acid, also known as carbon dioxide (CO2) and water (H2O), formed during aerobic combustion of carbohydrates, proteins and fats;
- Sulphuric acid, formed during the breakdown of amino acid containing sulphur;
- Phosphoric acid, formed during the breakdown of glucose phosphate structures by nucleic acids;
- Uric acid, during the breakdown of purines;
- Ammonium ions, or ammonia, formed during the breakdown of pyrimidines and amino acids.
There is increased acid production when changes in metabolism occur. For example, lactic acid levels increase in cases of muscle overload, and anaerobic conditions therefore prevail. Furthermore, large amounts of keto acids are produced as a result of hunger or glucose deficiency, due to the breakdown of fatty acids. In cases of poorly managed diabetes, this metabolic process can cause a serious condition known as ketoacidosis, whereby the organism perceives disturbances in glucose consumption as glucose deficiency and proceeds to break down fats (see Fig. 1: Metabolic end products).
In addition, the intestinal environment has an influence upon acid stress within the organism. If, due to a protein-rich diet, there is a rise in intestinal proteolytic microorganisms and a subsequent shift of pH values to within the alkaline range, microbial metabolites of faecal bacteria can no longer be protonated to ammonium ions and excreted in the faeces. Instead, they are absorbed by the body and have to undergo detoxification in the liver.
Buffer Systems
As even small deviations from optimum pH values can seriously interfere with enzyme activity and protein-dependent transport and support functions, the resultant acids have to be transported from the cell to the excretory organs (see Fig. 2: Excretory organs).
In order that this process can unfurl whilst at the same time maintaining intracellular, extracellular and blood pH values, the organism is equipped with various buffer systems. These systems are found on an organic, intracellular and extracellular level, and work closely together. In addition to the buffering done by organs such as the lungs, kidneys and bones, buffer substances play a particularly important role.
The most important buffer substances are bicarbonate and haemoglobin, which are extracellular and intracellular erythrocyte buffers, respectively. In addition, there are other protein buffers and various phosphate buffers (e.g. ATP, ADP). Extracellular and intracellular buffers work in close synergy to ensure that resultant acids are eliminated as quickly and as effectively as possible.
An impressive example of the close cooperation between intra- and extracellular cells is the elimination of carbon dioxide. This gas, which is constantly produced in cells due to the combustion of foodstuff, is exhaled via the lungs. During its transit to the lungs, carbon dioxide penetrates erythrocytes, where it is converted into bicarbonate and a proton (H+) by the enzyme known as carbonic anhydrase. The high proton concentration within the erythrocyte is immediately intercepted by the intracellular haemoglobin buffer. At the same time, bicarbonate – in the form of a buffer substance – temporarily migrates from blood plasma, in order to buffer surplus protons. In the lungs, the opposite process takes place: once again, bicarbonate diffuses into erythrocytes, and carbon dioxide is again produced, which is subsequently exhaled.
As, in the case of both these so-called respiratory protons, bicarbonate – the buffer substance needed for neutralisation – is also formed. They do not normally pose any problems for the body; however, it behaves differently in the case of fixed acids. These are produced e.g. as a result of glycolysis activity and during the breakdown of proteins. In order to avoid intracellular acidosis, fixed protons produced during cell metabolism have to be taken out of the cell into the extracellular space. However, in return, there is an influx of sodium into the cell. For this, sufficient levels of potassium are needed. If these sodium ions, assisted by Na-K-ATPase, are not removed from the cell, the cell starts to swell and it can, in extreme cases, explode. Such swelling can be responsible, among other things, for pain (muscle cells) and circulatory disturbances (erythrocytes).
In addition, the kidneys play an active role in
acid-base balance, as they reabsorb bicarbonate, which is lost during filtration of primary urine
as a result of active H+ ion secretion, in the form of CO2.
Connective Tissue – A ‘Storage Zone’ for Protons
During transit from the cell to the blood and down to the excretory organs, acids pass through connective tissue. This is an alkaline substance which, according to the insights of histologist A Pischinger, surrounds organs and tissues, and – in its role as a function unit – is responsible for cellular nutrition and waste disposal. Histochemically speaking, connective tissue consists of proteoglycans and glycoproteins, which have such a high acid-binding capacity that they are capable of temporarily storing protons.
When the blood’s buffering capacity is unable to absorb any further protons, surplus protons can be temporarily stored here. As soon as free capacity in the blood becomes re-available, the interstitial fluid, now equipped with a sufficiently high buffer capacity, flushes out acids stored in the connective tissue, and they are subsequently excreted. As this process rids the body of all temporarily stored acids on a daily basis in persons with a healthy metabolism, F Sander also calls connective tissue by another name, viz.: ‘Vorniere’ (literally, pronephron). In the case of large amounts of acid or impaired excretion, protons remain in the connective tissue, and the temporary storage zone becomes a permanent one. Thereafter, in a gradual process, connective tissue structures lose their elasticity, become rigid, and swell, whereby numerous chronic complaints and diseases may be induced or exacerbated.
Excretory Organs
Several body organs are responsible for eliminating resultant acids. In addition to traditional excretory organs (lungs, kidneys), the liver is now also considered to be one of the most important organs for acid-base balance, in light of the latest knowledge in the field.
Task distribution is dependent on the acid type: the liver is responsible for ammonia detoxification and the breakdown of organic acids. Depending on the metabolic state, work carried out by excretory organs is accelerated, restricted or supported by another organ. For example, the CO2 elimination rate is regulated by the respiratory rate, which in turn is regulated by the partial pressure values of CO2 and O2, as well as pH values in blood and cerebrospinal fluid. In addition, the kidneys play an active role in acid-base balance, as they reabsorb bicarbonate, which is lost during filtration of primary urine as a result of active H+ ion secretion, in the form of CO2. Depending on pH values, the liver and kidneys work closely together in the detoxification of nitrogen. Under normal conditions, i.e. if sufficient quantities of bicarbonate are present, two ammonia molecules – together with one bicarbonate molecule – are bound to urea. Urea, as a neutral compound, does not affect pH values. However, in the presence of any bicarbonate deficiency, the liver requires assistance from the kidneys, in order that ammonia can be eliminated from the body. Via this reaction pathway, ammonia is incorporated into glutamine in the liver and conveyed to the kidneys, where it is again separated and excreted as ammonia. As bicarbonate is produced as a result of the breakdown of organic acids (e.g. lactic acid), the liver is hence one of the most important suppliers of bicarbonate.
Dual Function of Border Cells
Although all excretory organs – like buffer systems – have only a certain capacity for detoxification, there is a balance between the production and excretion of acid metabolites in healthy humans on a healthy diet; i.e. the body has at its disposal buffer substances, which are required for buffering resultant acids. Border cells within the stomach play a key role in this biochemical process. These cells, thanks to their dual function, produce both hydrochloric acid and sodium bicarbonate in accordance with the following formula: NaCl + CO2 + H2O —> NaHCO3 + HCl
In practice, this means that when border cells start producing hydrochloric acid for the purposes of digesting food, sufficient amounts of sodium bicarbonate are also produced at the same time. Concurrently to hydrochloric acid reaching the gastric lumen, bicarbonate is also released into venous blood, thereby supporting the base pool within the blood during the time in which food is present in the stomach. This process, which F Sander calls a ‘Base Flood’ within the body, can be demonstrated by urine pH measurements. Thereafter, bicarbonate serves to alkalinize the acidity of partially digested food, so that pancreas enzymes (whose optimum pH value is between 7-8) can work effectively, and digestive disturbances do not occur within the small intestine.
However, in order to keep the bicarbonate pool constant and hence to maintain the body’s acid-base balance, amounts of bicarbonate (produced during physiological processes in the kidneys, stomach and liver) are not sufficient. It is therefore essential that base valences be absorbed in sufficient numbers with food. Whilst the diet of our ancestors met these requirements thanks to large amounts of fruit and vegetables, our modern-day fare contains an excess of acid-forming foodstuffs. The result is latent acidosis, which – during the course of time – can manifest in the form of chronic complaints and diseases. In addition to an incorrect diet (acidic, lacking in vital nutrients), the following can all lead to latent acidosis: diseases of the excretory organs, failing renal function, a number of medications, insufficient movement, stress, metabolic disorders such as diabetes mellitus and other chronic diseases.
Reference
R. Bachmann, C. Schöllmann. Der Säure-Basen-Haushalt (Acid-Base Balance), Forum Medizin, 1998
Did You Know?
Acids are all organic and inorganic compounds which release hydrogen ions (H+) in solutions.
Bases are all organic and inorganic compounds which absorb hydrogen ions in solutions. They are proton acceptors. A conjugated base is the remainder of the molecule of a dissociated acid (z. B. HCO3-).
The pH value (potentia hydrogenii) is the negative decadic logarithm of the hydrogen ion concentration in a solution. On a scale of 0-14, it indicates the acidic (pH < 7), neutral (pH = 7) or alkaline (pH >7) reaction of a solution. In a neutral liquid, the amount of acidic (H+) and alkaline ions is in equilibrium.
The pK value is the negative decadic logarithm of the dissociation constant of an acid or base. pK values make it simpler to calculate pH in buffer systems, whereby pKa and pKb are used for acids and bases, respectively.
A chemical buffer is formed from a weak acid and its dissociated form (i.e. a base). The mixture can release or absorb a certain amount of protons, without altering the pH value.
The measurement for this is buffer capacity. Optimal buffering is attained when the pH value of solutions is equal to the pK value of acids.
Comments:
-
No Article Comments available