Positive Health Online
Your Country

Obesity - A Modern, Mismanaged & Misunderstood Malady
listed in weight loss, originally published in issue 232 - August 2016
Obesity is a growing and serious health concern that has, by now, reached epidemic proportions, mostly in the Westernised world. Increased consumption of unhealthy food, coupled with decreased physical activity, in part has led to rising obesity rates over the past three decades. The WHO (World Health Organisation) reports that since 1980, worldwide obesity rates have increased by almost 200%. By the end of 2015 nearly 2.3 billion adults were reportedly overweight and 700 million of these obese. Obesity has been linked to certain cancers, cardiovascular diseases, diabetes and may shorten the human lifespan by eight to ten years.[1] A grim prediction by the government suggests that obesity will continue to rise - up to 50% of women and 60% of men will be overweight by 2050 and up to 25% of children will have weight issues by that indicated timeframe.[2]
Who is Classed as Overweight Or Obese?
In the 17th Century, a Belgian mathematician and astronomer, Lambert-Adolphe-Jacques Quetelet, became fascinated in possible numerical links between different human body parts. After some calculations he concluded that by taking a person’s weight in kilograms (kg) and dividing it by the height in meters (m2), it would give a specific numerical figure which is unique to every individual. He termed it the Body Mass Index (BMI) which, according to some experts, expresses the correlation between the body weight, coronary insufficiencies, cholesterol level and expected lifespan. Even though the BMI does not take into account the differences in people’s ethnic background, ethnic characteristics and the way some individuals store fat, in clinical practice it is still a widely used method for assessing weight/health-related issues. A greater BMI leads to a greater risk of developing co-morbidities such as type 2 diabetes. Anyone’s BMI figure of more than 25 indicates “the level at which there is a significant increase in mortality” and is classified as overweight.[3] In our healthcare system it is a key factor in deciding who qualifies for surgical weight reduction procedures.[4,5]
Many clinicians prefer the Waist Circumference Measure to BMI - a simpler anthropometrical measure which is “also a criterion for the metabolic syndrome”. A waist measurement of more than 35 inches (88cm) for women and 40 inches (102cm) for men indicates a significant health risk.[3] Still, however we weigh or measure it, obesity and its related conditions are costing the healthcare system nearly £6 billion annually. It is estimated that by 2050 the cost will have risen to £50 billion per single year.[6]
Bariatric Surgery - A Promising Solution for Some
According to some opinions “bariatric surgery is currently the only modality that provides a significant improvement in obesity-related co-morbidities.”[7] Despite the widespread acknowledgement that surgical interventions in general are risky on obese patients and may be associated with long-term and sometimes unpredictable complications, they have become more popular throughout recent years. There are now even guidelines of bariatric interventions for obese children under the age of 16.[5]Michel Gagner MD from Florida International University, believes that the time has come for bariatric surgery to become as common as coronary artery bypass surgery.[7] Clinical outcomes show that it does attribute to a rapid weight loss while at the same time significantly reducing the risks of possible co-morbidities and therefore improving overall health and life expectancy in general.[8]
On the other hand, clinicians have also noticed that bariatric surgery seems to contribute to the loss of bone mass and change in bone metabolism and structure, causing fractures at sites that are classical of osteoporosis.[9] The weight losses achieved by the surgical interventions are not always sustainable long-term; statistics say that bariatric reoperations are on the increase. There are also reports of post-bariatric depression, attempts of self-harm and suicide.[10] The overall aim of bariatric surgery is to restrict the volume of food and absorption of certain nutrients, especially fat. However, it does not address or resolve accompanying psychological or cultural aspects of certain human populations, characteristic traits and personal circumstances, emotions, thoughts, habits and most of all food trends and addictions.[4]Despite clinical success and profits for the medical institutions, it is clear that surgical solutions are not suitable for everyone. Obesity is a far more complicated issue than meets the eye.
What Causes Weight Issues?
Several factors can be indicative, including environmental toxins or pollution, life style, food trends, eating habits and a lack of sufficient physical activity. Toxicity can have consequential effects on cellular, metabolic, mitochondrial and endocrine system functioning. These are widely believed to be responsible in the development of weight issues in both sexes of adults and children.[11]
Though increasing prevalence of obesity is partly attributed to a lack of physical activity and the popularity of high-calorific foods, there are other significant factors which play an important part in the widespread development of obesity. For example, a modern lifestyle in our current Western society seems to ensure that every generation is heavier than the last. This is called ‘passive obesity’. There is some evidence that humans are predisposed to weight gain by their biology and are overwhelmed by the effect of today’s so-called obesogenic environment, with its abundance of energy-dense food, motorised transport and sedentary lifestyles.[2]
Obesogens
A well-researched link exists between a dysfunctional endocrine system and several environmental toxins which act like endocrine-disrupting chemicals. These are called obesogens and affect the endocrine system by mimicking the effects of the body’s own natural hormones. The brain’s messages disrupt hormones by altering appetite and lowering metabolism thus forcing the fat cells to grow and multiply. As a result of this, adipose tissue becomes very difficult to control. Adults of average weight can have about 25 billion fat cells. However, severely obese individuals may have up to 6 times more - 150 billion fat cells - which are at the same time enlarged as well.[12]
Obesogens interfere in all sorts of different cell activities and in many different ways. One of the most important interactions is with the heat-producing brown fat cells, making them lazy which stops them converting food into heat so that calories are retained in white adipocytes as fat. One particular powerful obesogen is high-fructose corn sweetener which is found in many processed foods and popular drinks.[13]
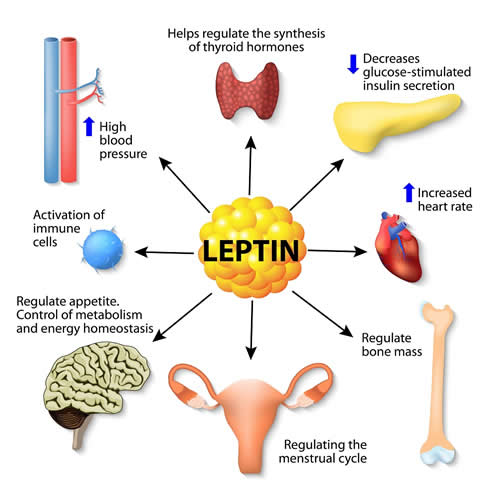
Photo credit: ©iStock.com/ttsz
Leptin, Insulin & Mitochondria
In his book Hormonal Balance Dr Scott Issacs discusses how scientists over the past thirty years have developed a better understanding of how fat produces hormones that control appetite, cravings and metabolism. Fat produces many hormones but in terms of obesity, the most important is leptin. This particular hormone targets the Limbic System and especially the hypothalamus, where regulation of weight and food intake occurs.
Leptin sends the brain specific information regarding the amount of fat the body has and is therefore responsible for the body weight set point. In a lean, healthy body it acts as a protector against starvation, stimulating appetite and motivating search for food. However, once the obsessive search for an ideal body shape starts or yo-yo dieting takes over, the brain receives mixed messages from disrupted and fluctuating hormone levels. The majority of overweight individuals produce far too much leptin due to the body’s previously developed resistance to it. Leptin resistance can cause a false alarm in the limbic system’s appetite, motivation and pleasure circuits. This can lead to increased cravings, specifically for high-calorie sugary foods, which are sometimes referred to as comfort foods. In an attempt to overcome leptin resistance, the white fat tissue increases the overall leptin production. Even after a proper meal and full stomach, an extra amount of this powerful hormone is not enough to satisfy the food cravings and stop over-eating. Excess fat, especially around the abdominal area, coupled with inflammation caused by adipokines - polypeptide chemicals which are also produced by white adipose tissue - are key contributors to body’s leptin and insulin resistance.[12]
Insulin is an integral hormone produced by the pancreatic cells which carries out the important task of metabolising blood sugar and transporting it to cells, either to be used as fuel or to be stored in the body’s fat reservoirs for the future usage. Imbalance of this hormone can lead to disruptions in the endocrine system, resulting in excessive appetite, carbohydrate cravings, weight gain and consequent co-morbidities. Insulin resistance and its closely related cousin - Type 2 diabetes - reduces mitochondrial function in the brain which can in many cases lead to a development of dementia, another condition on the increase.[13]
People with high levels of insulin tend to suffer from various chronic inflammations - arthritis, eczema, upper respiratory and ear infections, to name but a few, and which lead to a constant lack of energy. Energy is produced by mitochondria in the cells. Long-term chronic conditions and accompanying inflammation lead to a general mitochondrial dysfunction and in many cases permanent cellular damage. In turn, this may accelerate the natural biological ageing processes and further development of chronic age-related disease.[14]
Excess of insulin inhibits the breakdown of stored fat resulting in increased waist-hip ratio, or central obesity, which makes the obesity in actual fact, a structural issue.[13] Structure, it has been found, has a direct effect on function. It is important to know what the building blocks are and how they work. Until the underlying structural issues are resolved, the problem itself remains. Here the obesity-related building blocks in question are the fat containing cells called adipocytes. For a long time medicine did not pay very much attention to fat cells other than acknowledging the fact that these cells store fat. Recent research however, has shown that adipocytes produce and distribute messengers called adipokines. Adipokines, such as previously mentioned leptin, adiponectin and resistin send signals to the body, some of them ‘friendly’, some ‘angry’. In response to a high sugar, high calorie meal the adipocytes release angry adipokines, which race around the body influencing the heart, arteries, liver, brain, kidneys and the pancreas - where, of course insulin is produced. In his book, The Disease Delusion Dr Bland explains how angry adipokines can cause inflammatory conditions throughout the body involving every organ system. Because the original signal comes from the gastrointestinal immune system, most angry fat is stored around the midriff. High levels of oestrogen and cortisol, the well-known stress hormone, also contributes to fat storage around the waist.[12,13,14]
Though out of balance, waist-to-hip ratio is a valid indication of possible future issues; it is worth mentioning that the amount of fat around the waist is still not a cause of illness itself. It all depends on how ‘angry’ are the messages from the adipokines. It is found that many toxic, environmental chemicals are capable of disrupting mitochondrial function by directing excess calories to be stored in adipose tissue for possible rainy days. There is a confirmed link between persistent organic pollutants in the body, Type 2 diabetes and weight gain. Persistent organic pollutants can cause significant damage to the mitochondria, disrupting the basic function - energy production from our daily food - and directing excess calories to be stored in adipose tissue thus leading to functional and pathophysiological changes in structure and causing development of many chronic maladies.[13]
To summarize, insulin and adipokines are partners in crime in many ways. Whatever affects insulin does the same to adipokines, including leptin and vice versa. So far, we know that the worst offenders are sugary, high calorific, processed foods and a certain level of environmental pollution. These cause disruptions on a cellular level, affecting mitochondria which, in turn, results in chronic inflammatory processes and long-term ill health, early ageing and persistent problems with weight.
Ghrelin - The Hunger Messenger
Another culprit in case of adiposity is a hormone called ghrelin, produced by the stomach and to the lesser amount, in the duodenum. It is also coined the ‘hunger hormone’. Hunger is one of our basic life-saving sensations. An empty stomach produces ghrelin, which, as a hunger messenger, directly stimulates the hypothalamic feeding centre.[16] However, in obese individuals, it is suggested that a dysfunction between the gut, adipose tissue and brain-hypothalamic axis (via the ghrelin-leptin hormonal pathway) may play a contributory role in abnormal appetite control and excessive energy intake.[11]
Ghrelin remains active around the clock, playing an important role in sleep-deprived individuals. Dysregulation of ghrelin secretion is implicated in the mechanism through which sleep disturbance contributes to obesity. Subjects with short sleep duration have elevated ghrelin levels, reduced leptin, and high BMI compared to subjects with sufficient sleep duration. It should be also noted that a specific area, the supra-chiasmatic nucleus of the hypothalamus, is responsible for the body’s internal biological circadian rhythms, influencing the sleep-wake patterns.[15,16,17] Therefore, sleep plays an essential role is a healthy weight control.
The Hormonal Brain
Body organs and tissues are not sole contributory factors to hormonal activities. Psychological responses can also affect weight. The brain produces several hormones which are capable of regulating appetite, metabolism and satisfaction. So far it is known that neuropeptide Y, produced in the hypothalamus, is the most powerful appetite stimulator influenced by leptin. Leptin, in normal circumstances keeps neuropeptide Y levels under strict control. However, failure to do so leads to neuropeptide Y overproduction, promoting appetite and slowing down physical activity in response to dropping blood sugar levels. It also increases the constriction of blood vessels and stimulates the growth of fat cells. High Neuropeptide Y levels have been found in insomniacs, proving yet another link between poor sleeping pattern and obesity. It has been confirmed by many studies that nightshift workers are more prone to weight gain than people working normal office hours.
Research has also found that regular binge eating, high stress levels and a diet comprised mainly of sugary or processed fatty foods seems to have an effect on the production of neuropeptides. The hypothalamus secretes neuropeptide Y during emotional stress, raising anxiety levels and stimulating the stressed individual to eat, consume alcohol or other addictive substances, and therefore further reducing resilience to emotional trauma and survival.[16,17,18]
Another influential chemical responsible for hunger, appetite and especially carbohydrate cravings is serotonin. Although around 80% of the body’s serotonin is produced by the gut, it still plays an important task in the brain’s serotonin pathways. It is known that a release of serotonin lifts the mood, improves memory and sleep. It is thought that while closely interacting with dopamine pathways, serotonin creates and magnifies a satisfaction-dependence mechanism relating to consumption of carbohydrates and high-sugary foods and substances related to well-known addictions in humans.
Serotonin’s close ally dopamine is secreted by neurons that originate in substantia nigra, an area related to the basal ganglia in the brain’s limbic system. A surge of dopamine to the brain leads to emotionally high expectations of ‘what is going to happen’ – consequently influencing motivation and making us seek pleasure and reward. While working hand in hand with the brain’s own opiate system, the result is similar to a heroin high. It is a well-known fact that satisfaction from certain foods, especially sugar, can be very similar to pleasure from alcohol and drugs. This has led some scientists to speculate the idea that being too heavy results in over-consumption of more delicious high-calorie foods in order to satisfy the key factor – dopamine related rewards. Several studies have shown the correlation between obesity and low levels of dopamine.[19,20]
Endocannabinoid System & Satisfaction
Reward seeking and satiety is closely related to the brain’s endocannabinoid system, with its complex actions in immune-, nervous-, endocrine system and many body organs. It is literally a bridge between the body and the mind. Although there is still a lot to learn about it, it is already known that endocannabinoids are very powerful appetite stimulators with similar properties to cannabis. It has been found that activation of the cannabinoid receptors in the brain increases the activity of appetite-related neurons, called endorphins, which then travel to the brain’s appetite-control centre, the hypothalamus, stimulating the desire to eat calorie-dense foods such as chocolate.[21,22,23]
Stress - our Everyday Companion
Stress, with its complex chemical reactions, activates the brain’s limbic system including the endocannabinoid pathway, which is an important central stress mediator, controlling the surge of stress-induced neurotransmitters, especially cortisol. Constant stress leads to cortisol activation, which in turn increases insulin and leptin resistance. Both insulin resistance and elevated cortisol levels stimulates the hypothalamic hunger centres in the limbic system, causing uncontrollable eating habits and, in many cases, severe addictions to certain food substances.
Hunger hormones - leptin, ghrelin, neuropeptide Y and several other chemicals magnify the stress response even further by increasing appetite and slowing down the overall metabolic rate. The whole situation becomes even more complicated with lack of sleep and poor lifestyle choices.[15,24]
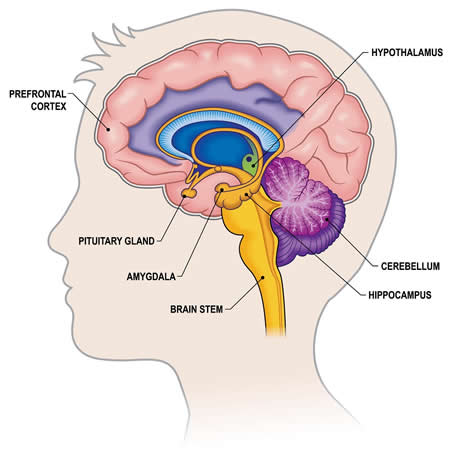
Components of the Limbic System
Photo credit: ©iStock.com/JamesKopp
What is the Limbic System?
The word limbic means border in Latin. Initially this term was used to describe the border structures around the basal regions of the cerebrum. However, with recent neuroscience developments, we now know that the limbic system represents the entire neuronal circuitry that controls and regulates our emotional behaviour, influencing our desires and motivations, and regulating the ‘fight or flight’ response to stress. The limbic system, as it is understood now, consists of many structures. One of the most influential parts of it is the hypothalamus, representing less than 1% of the entire brain mass. The hypothalamus has communicating pathways with all levels of the limbic structures - sending output signals towards the brain stem and into the reticular area of the mesencephalon, upwards to the higher areas of the diencephalon and cerebrum, to the anterior thalamus and the limbic cortex onto the secretory parts of the anterior and posterior pituitary glands. In summary, several vegetative and endocrine functions, including aspects of certain emotions and behaviour, hunger, thirst, temperature and water regulation are all associated with different parts of hypothalamus.[19, 24]
The Love Hormone & Loss of Appetite
There is a hormone synthesized in the para-ventricular nuclei of the hypothalamus called oxytocin. Oxytocin has some possible clinical significance in relation to appetite. Some researchers have called it the ‘love hormone’ as it plays an important role in socializing, flirting, bonding and reproduction of mammals, improving perception of social cues and increasing trust between the individuals. A recent study suggests that oxytocin is also anorexigenic, meaning appetite suppressive in its action. An increase in oxytocin can reduce the amount of food intake with the additional benefit of improved blood sugar regulation. Anyone who has ever been in love can easily relate to the feelings of excitement, excess energy, immense happiness and lack of appetite - all thanks to this ‘love hormone’. Although oxytocin’s appetite regulative effect may sound very promising, it is too early to make any conclusion yet and larger studies are needed to understand its full mechanism related to calorie intake.[25,26]
The Amygdala
As part of the limbic system, this complex tissue is about the size of almond. Gerard Tortora, Professor of Biology, suggests that the amygdala seems to be a behavioural awareness area that operates at a semiconscious level. It projects into the limbic system one’s present status in relation both to surroundings and thoughts.[19] On this basis, the amygdala is believed to help form the individual’s most appropriate responses to all life events, including constant stress, threats, a consequent fear and related food choices in these specific circumstances.[24]
The Hippocampus
The hippocampus collects all our sensory information, translates and stores it in the brain’s long-term memory bank. Adults often dwell on happy childhood memories, such as mother’s cooking. Just a brief whiff of a pleasantly smelling food may retrieve old memories, stimulate appetite and in many cases, especially under stress, encourage unnecessary eating. A combination of occasional episodes of comfort eating and distant sweet memories may become powerful enough to activate the brain’s reward circuitry, leading to a well-developed and often difficult to control food-related addictions.[21]
The list of structures and functions of the limbic system will certainly expand in the future as neuroscientists learn more about it, but so far it is understood that our actions, reactions and emotions are products of the limbic function. It is the area where all information from the specific sense organs meet, where the neuropeptide receptors are most concentrated and where most important decisions are made. Detrimentally however, some of them are not necessarily health preserving.[19,24]
Can we Become Addicted to Food?
The idea to link food addiction with other widely known addictions is relatively new and has therefore not yet been researched well enough to make any fundamental conclusions. The topic though is hotly debated amongst scientists and clinicians. Growing evidence supports the idea that some ingredients in foods, especially sugar, can elicit similar brain responses as highly addictive substances, such as cocaine and heroine. For a better understanding of human addictive behaviour we need to look at the three main components of addiction.[20]
Firstly, a person can have obsessive thoughts and feelings about certain foods/substances which can lead in some cases to cravings. These cravings may well be linked to the pleasant memories from the past relating to consumption of certain highly addictive substances, such as sugary foods. The personal memory bank - the hippocampus - stores all conscious memories from near or distant past, whereas the amygdala stores our subconscious, highly charged emotions with previously learned conditioned responses. These make us act on them, almost impulsively, whenever necessary. The next stage leads to a loss of control over cravings, particularly when things go wrong or stress levels are high. This is where the amygdala steps in again, rising irrational emotions and expectations of a pleasant on-coming satisfaction from the substance. Once these difficult-to-control emotions take over, the overall behavioural pattern becomes hard to manage. The final stage leads to a repeated consumption of addictive substances, even regardless of constant health warnings or already developed health issues, with high emotional expectations of satisfaction. We, as human beings, can exhibit all three of these traits in our relationships with high calorie, highly processed sugary foods and drinks. It is a well-known fact that true addiction provides less satisfaction from the substance the more it is consumed. The thrill is not as high any more and we need to increase the amount to satisfy the needs. The increased dopamine levels lead to high expectations of ‘what is going to happen’, motivating and pushing us to do what we want to do. In normal circumstances, as we succeed, we would feel rewarded and happy. However, real addiction never fully satisfies. Increased dopamine levels combined with the effect from the over-stimulated endocannabinoid system tricks the mind to seek out something which promises to be physically and emotionally highly rewarding.[21,22,23]
What the Patients Say
All the knowledge of possible pathophysiological dysfunctions, all these statistics and measurements make no sense without knowing what really happens in the lives and heads of our patients. Complementary medicine practitioners or CAM Providers who deal with weight issues have all seen frustrated patients who, in their own words, have done everything to reduce their weight. They have endured yo-yo dieting, tried different exercises and personal trainers, gastric band hypnosis and promising diet pills. A fraction of them admit to eating too much in general and some of them recognize the fact that food has become an overwhelming addiction, similar to alcohol or cigarettes. Many gastric band patients have regretted their decision trying to resolve the weight problems with bariatric surgery only. When asked why, the answer more often is that nothing has actually changed. They still have the same stressful job, a challenging domestic life and complicated relationships. Wine and chocolate are still tempting. Even though the initial weight loss gave a certain amount of excitement and a boost of confidence, they are still unhappy. Many patients say that they have not been fully understood by the medical profession; feelings, thoughts and the way the patients cope with everyday life difficulties are not the priorities in medicine. What is the solution? Sleep more, less stress. less chocolate, join a gym, Weight Watchers? As already explained, the human brain, behaviour and health are multi-level complexities. They are always in constant inter-action with each other, highly influenced by external environmental toxins, life styles, personal temptations, emotions, social needs and events.
Too Heavy & Too Light
Dr Rosina Sonnenschmidt, one of the Western world’s leading experts in diet-related issues, introduces in her book The Way to your Ideal Weight a unique concept of the weight-health problems with a hope and possible solutions to many patients. Over the years, having seen numerous patients with various weight-related illnesses, she has come to the conclusion that “feeling too light makes people overweight” and “feeling too heavy makes people underweight”. A thorough questionnaire, or in medical terms - anamnesis, from the patient provides Dr Sonnenschmidt with a “psychogram of the personality”. The psycho-analysis of this information directs the patient in his or her search for the possibilities of new ways of grounding themselves. By strongly projecting their thoughts and hopes on a better and healthier future, they can stop referring back to an unhappy past. The idea of the need to be grounded comes from the overweight person’s perceptions that they feel too light and therefore must eat more to get sufficient body awareness and come down back to the earth. Interestingly, Dr Sonnenschmidt explains how we, as human beings, survive extreme situations and daily stress. Under constant pressure we wind ourselves up so much that we reach a very specific, unique and uplifting energetic state, which helps us perform the task exceptionally well, feel excited and enjoy our own sweet success. However, it is impossible to remain high for too long. We need to wind down, refuel, have a rest and recharge the batteries. As a ‘rule’ or habit, we, as human beings with high stress levels, tend to wind down by indulging in grounding foods, which are usually high in carbohydrates and hidden sugars, or worse, using other well-known addictive substances. Due to the Western lifestyle and life’s high demands in general, this pattern of behaviour becomes easily a norm in highly-stressed situations with a resultant weight gain.[27,28]
The Altered Structure of our Food
As we naturally tend to indulge in high calorific foods after stressful events, it is important to pay attention to what we eat and how we cook it. We have already looked at the importance of the healthy structure of our main building blocks - cells and mitochondria. Food and how it is cooked has its own structure, which can dangerously alter the body’s structure and function. Precisely, a structural alteration of food proteins can modify the functions of these specific proteins. This process is called glycation. Cooking food at high temperatures leads to glycation which in turn produces glycotoxins. A high consumption of highly processed foods leads to an increased intake of glycotoxins. According to research, there are links between glycotoxins and the rise of type 2 diabetes, kidney problems and dementia.[14] Lesser cooking temperatures result in reduced production of glycotoxins. The closer to nature and the less processed, less structurally-altered our food is, the better it is for the bodily functions and overall structure.[13,28,29]
Stress affects everyone in some way. It guides reactions and determines the appropriate or sometimes inappropriate actions for survival, too often leading to easily available and socially acceptable self-medication with hidden sugars and high calorie foods. Expanding waistlines are a continuous and growing concern and a huge burden on the already over-stretched healthcare system. However, obesity is caused by more than just too many calories and lack of exercise. It is also a result of persistent organic pollutants, environmental obesogens and structurally altered proteins in our everyday foods. Before we make surgical weight reduction as widely available as a cardiac bypass operation, we should acknowledge the fact that life in general does not always provide us with easy shortcuts - what may be suitable for some may not be for the others. Any weight issue is a highly individual matter. It requires a holistic approach incorporating a thorough understanding of each individual’s circumstances, available mental and emotional resources, coping mechanisms and habitual choices. Instead of reducing the sizes of stomachs en masse we need to empower our patients with better knowledge and coping strategies. We must raise awareness of the hidden risks in certain foods and food preparations, emphasizing the importance of health and wellbeing for the next generation. We must work to reduce the intake of dangerous toxins and addictive substances in our food such as sugar and educate patients on the better management of weight-related concerns.
References
1. Obesity Epidemic Is Global, New Study Confirms. Medscape Medical News, 29-05- 2014.
2. The Government Office; Foresight project “Tackling Obesities: Future Choices” www.gov.uk
3. Steven McGee. Evidence Based Physical Diagnosis. 3rd edition, Elsevier Saunders, 2012.
4. Bariatric Surgery. Alan A Saber, MD Diseases/Conditions, Procedures, Feb 10 2015.
5. Tucker ME. New guidelines address bariatric surgery in children. Medscape Medical News. January 19, 2015.
6. Public Health England Obesity Knowledge and Intelligence. www.noo.org.uk
7. Call to Make Bariatric Surgery as Common Coronary Bypass. News, Jul 02 2015.
8. Regulation of Appetite to Treat Obesity. Gilbert W Kim; Jieru e Lin; Michael Valentino; F. Colon-Gonzalez; Scott A Waldman. Expert Review of Clin. Pharmacology. 4(2): 243-259. 2011.
9. Bariatric Surgery May Up Risk, Change Pattern of Fractures, Society of Bone and Mineral Research Annual Meeting 2015. Medscape Medical News, 2015.
10. Bariatric Surgery Linked to Suicide Attempts. Medscape Medical News. Pam Harrison review. October 14 2015.
11. Obesity in Children. Steven M Schwarz, MD Diseases/Conditions, Jun 24 2015.
12. Scott Isaacs MD. Hormonal Balance. Bull Publishing Company, 2012.
13. Jeffrey S. Bland. The Disease Delusion. Harper Wave. 2014. Kindle edition
14. Jim Hunter. Weight Loss Hormones. Jagger Publishing, 2015. Kindle edition
15. Appetite-Regulating hormones From the Upper Gut: Disrupted Control of Xenin and Ghrelin in night Workers. Clinical Endocrinology, 12-01 2013.
16. The Gut Hormones in Appetite Regulation. Suzuki K, Jayasena CN, Bloom SR. J Obes. 2011. 2011:528401 Epub Sep 22 2011.
17. Endocrine System Anatomy. Jasvinder Chawla, MD Diseases/Conditions, Jun 04 2014.
18. Neuropeptide Y: History and Overview. K. Tatemoto www.springer.com
19. Gerard J Tortora. Principles of Anatomy and Physiology. 14th edition, Wiley, 2014.
20. Food Addiction, Substance Dependence Share Common Ground. Medscape Medical News, 04-07 2011.
21. Joe Griffin, Ivan Tyrrell. Freedom from Addiction. HG Publishing, 2008.
22. Marijuana Munchies are All in the Brain. U.S.Study, Nature 2015. Reuters Health Information, 18-02 2015.
23. Endocannabinoids. G. Griffing, MD. Diseases/Conditions, Procedures. Feb 05 2015.
24. Guyton. Textbook of Medical Physiology. Eighth edition chapter 58 p.651-658. 1991.
25. Intranasal Oxytocin Cuts Calorie Consumption in Healthy Men. Elizabeth Lawson MD study. Medscape Medical News. 03-09-2015.
26. Oxytocin a Promising New Treatment for Anorexia. Medscape Medical News, March 18, 2014.
27. Rosina Sonnenschmidt. The Way to Your Ideal Weight. Narayana Publications, 2011
28. Slash Sugar Intake to Fight Obesity, Tooth Decay – WHO. Reuters Health Information, 03-04 2015.
29. Fructose intake may contribute to overeating. Heartwire from Medscape. 01-03-2013.
Comments:
-
No Article Comments available