Positive Health Online
Your Country

Podiatry - Importance of the Foot
listed in bodywork, originally published in issue 122 - April 2006
Abstract
Podiatry is a profession registered with the health professions council specializing in the treatment and diagnosis of conditions affecting the foot, and its related structures. Specialist areas of podiatric medicine have developed, ranging from wound care to surgery. However, the area that may be seen and most relevant to general wellbeing is that of the relation of the foot to gait dysfunction and related symptomology such as back, hip, knee and foot pain. This paper introduces the 'foot function' approach used by podiatrists in the treatment of such lower limb musculoskeletal dysfunction. An insight into podiatric theory should enable therapists working within this field a more holistic and multidisciplinary approach. It is the view of the authors that a closer working relationship between health therapists and podiatrists with an interest in movement dysfunction provides a better quality service for appropriate patients.
Introduction
'People do not limp because they hurt, rather they hurt because they limp'
Dr H Dananberg
During a normal day we can take up to about 2000 steps. What if the way we take these steps is different both sides? Or, places stress upon body tissues that cannot cope without becoming damaged? Podiatry has been treating such gait related symptoms using varied theories and therapies since the profession began to develop in the eighteenth century. The publication of Biomechanical examination of the foot: Volume 1 and Normal and Abnormal function of the foot, volume II by Dr Root et al marked a major landmark in the development of foot orthopaedics. These volumes presented an innovative, systematic approach to the assessment and mechanical treatment of the foot and gait ailments.
Recently, further podiatric theories have emerged relating the foot to gait dysfunction and symptom presentations ranging from heel to lower back pain. Aberrant foot function can be a causative factor in people leaning forward while walking, failing to fully extend their knees in gait or lowering their arches too far (pronation). Such abnormal locomotive methods may then have symptomatic results. From the above examples it can be seen that foot function has a direct influence on our ability to remain pain free for normal daily activities, and so has a direct impact on our body and general health.
Role of the Foot in Gait Dysfunction and Symptoms
Before understanding abnormal, it is essential to first introduce the theory behind normal foot function.
Normal Foot Function
The basics – pronation and supination at the subtalar joint
The subtalar joint (STJ) is one of the largest joints in the foot and makes up part of the rearfoot complex. While the ankle joint may be seen as a hinge joint, supplying motion up (dorsiflexion) and down (plantarflexion), the subtalar joint supplies motion in all three directions (triplanar). These motions are joined together into pronation (lowering of the arch) and supination (raising of the arch):
Pronation at the STJ: Eversion, Abduction and Dorsiflexion
Supination at the STJ: Inversion, Adduction and Plantarflexion
In closed kinetic chain (with the foot at least partially weight bearing) pronation and supination cause the leg to move with the STJ. Pronation causes the leg to internally rotate and supination causes the leg to externally rotate. The reverse is therefore also true; internal leg rotation causes the STJ to pronate, and external leg rotation causes the STJ to supinate. Linking this to normal gait is relatively straightforward. At heel strike the leg is internally rotating and therefore the STJ is pronating, and following midfoot contact (midstance) the leg is externally rotating and the STJ is therefore supinating.
The Basics – the Foot as a Pivot
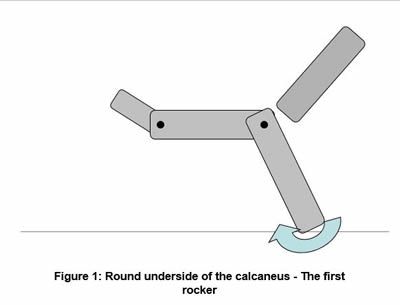
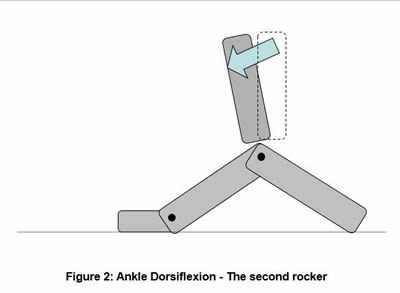
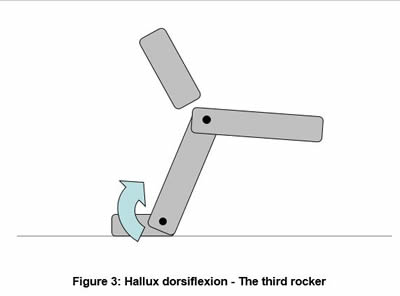
Motion in the lower limb should be thought of as an upside-down pendulum of the body passing over the planted foot. In effect, humans walk by pulling themselves forward over the weight-bearing foot and this pull is mainly provided by the opposite limb as it swings forward. However for this to occur, the foot on the ground must allow the smooth passage of the body over it – essentially acting as a pivot. This pivoting is done through three 'rockers'; the rounded heel, ankle dorsiflexion and the forefoot extending around the digits (Figures 1-3). These foot pivoting motions allow us to place a foot in front of the body and transfer our centre of mass forward and over the stance limb. Vitally, it allows adequate extension of the hip and knee and therefore a stride with the torso remaining upright.
Abnormal Foot Function
The Basics – Pronation and Supination
The foot can be thought of as a see-saw. If you push up on one side of the see-saw, the other side will go down. If you push up on one side of the foot, the other side will go up or down depending on what side of the fulcrum (or 'axis') you are pushing. The harder the push, the harder the resulting force. Some feet have more force than normal, pronating the foot. These people tend to have resultant symptoms in structures that resist pronation (see Table 1). In addition, when the leg begins to externally rotate the foot has to resupinate. If the foot cannot resupinate because it is pronating with so much force, then the leg will not be able to externally rotate and abnormal compensation will result.
Table One - examples of structures that reduce pronatory moments (rotary forces)
that may be injured with excessive pronation and injury examples.
| STRUCTURE | INJURY EXAMPLES |
| Plantar Fascia | Plantar Fasciitis / Fasciosis |
| Posterior Tibial Tendon | Posterior Tibial Tendonopathy / Dysfunction |
| Anterior Tibial Tendon | Chronic Anterior Compartment Syndrome |
| The Plantar Ligaments | Plantar Ligament Sprains |
Some feet supinate excessively. These are relatively rare and are often seen with more generalized medical conditions. Due to the excessive supinatory forces, symptoms range from recurrent ankle sprains to injuries of structures that reduce the supinatory moments, such as the peroneal muscle group
The Basics – The Foot as a Pivot
If the foot cannot work as a pivot then the leg cannot pass over it. This means that a failure of any of the three foot rockers (Figures 1-3) will reduce the ability of the knee and hip to extend in gait. In these cases it is common to not only see the hip and knee limited in their extension, but also for the trunk to flex forward. As the hip is not extending, there is no stored energy for release and there is greater muscular exertion from the hip flexors to 'pick the leg up' and progress forward. Such a style of walking can have marked implications
on the body, examples of which are below:
• Increased Lumbar Sheer
Lumbar flexion creates disc compression as well as muscular overuse. This may be one of the causative, or aggravating factors, in chronic lower back pain.
• Hamstring Tightness
If the hip fails to extend, there is never a full reduction of the angle between leg and ischial tuberocity. This means the hamstring muscle group is never actually relaxed as it is always stretched. In these situations, via the golgi tendon organ response, the hamstring will actually shorten and remain tight.
These tight hamstrings are not only prone to increased risk of injury in sport, but also due to fascia insertion into the sacroiliac joint region, may be part of the myriad of causes of sacroiliac joint dysfunction.
• Anterior Knee Pain
A flexed knee style gait increases retro-patella forces, thought to be a causative factor in anterior knee pain syndrome. If the foot is also over-pronated, malalignment may become a factor due to excessive internal leg rotation.
It is important therefore to understand the possible causes of failure of the foot to act as a pivot. Common examples of this include the following
• Lack of the First Rocker – The Underside of the Heel
Failure here is rare, but may be seen in patients with partial amputation following trauma or chronic wounds such as diabetic ulceration.
• Lack of the Second Rocker – Ankle Dorsiflexion Failure here is common, and may be due to factors including calf muscle tightness, bony exostosis of the ankle joint or a lack of translation and distension of the ankle mortice complex.
• Lack of the Third Rocker – Hallux Dorsiflexion Failure here is again common. This can be due to structural problems such as arthritis or bunions, when it is impossible for the hallux to dorsiflex the required 55-65 degrees to permit normal hip and knee extension. However, functional problems can also occur. In these cases the hallux has a perfectly normal range of motion when not weight bearing, but when walking cannot use this essential range of motion.
This functional failure of the hallux to work (functional hallux limitus) can be caused by a myriad of conditions. The two most common are excessive pronation placing excessive stress through the medial band of the plantar fascia or / and increased dorsiflexory movements under the first ray (1st metatarsal and cuneiform) preventing this medial column to plantarflex. This first ray plantarflexion allows the hallux to rotate up and obtain the required dorsiflexion to allow hip and knee extension.
Podiatric Treatment of Foot Based Gait Dysfunction
When treating symptoms related to gait dysfunction it is essential to address the cause of the problem and normalize the patient's gait style, not just move the compensatory process elsewhere. Unfortunately, many in-shoe appliances have large arch fillers that push the first ray up and cause a functional hallux limitus. In these cases some symptoms may improve, but compensation may just be moved elsewhere. Podiatric foot orthotics, from all available podiatric theory, work by increasing or decreasing abnormal foot movements while allowing the first ray to plantarflex. This is why podiatric theory uses custom foot impressions to capture foot shape exactly and so normalize foot function, improve gait dysfunction and reduce symptoms.
Case Examples
1. Patient A: Symptom presentation
Chronic lower back pain (LBP) with acute episodes for about 10 years. An improvement had been experienced with recent chiropractic care. The chiropractor noticed an abnormal gait style and referred to podiatry.
Diagnosis Chronic non-radiating LBP with acute episodes.
Clinical Findings Both feet are maximally pronated in stance resulting in a bilateral functional hallux limitus. In gait there is a limited hip and knee extension and the trunk is flexed. In-shoe F-Scan plantar pressure assessment demonstrated a complete absence of normal loading of the medial aspect of the foot. This is seen as a compensation process for functional hallux limitus.
Clinical Reasoning Due to the inability of the foot to pivot over the third rocker, the hip and knee cannot fully extend. To maintain an element of propulsion the centre of mass is taken forward via flexion of the trunk. As stated previously, this may result in increased lumbar shear, increased muscular overuse and abnormal sacroiliac joint function.
Treatment Custom orthoses were prescribed to reduce pronatory movements and increase the ability of the hallux to rotate, and so re-establish the third rocker. These appliances were checked for efficacy via the in-shoe pressure analysis system. The orthoses were made and the system used to modify the appliances until normal plantar pressure distribution and foot timings were established.
Outcome Symptoms began to improve after two weeks. Within four weeks the patient was experiencing the first pain-free days for over three years. Unfortunately there has been one acute episode following a weekend away when the patient took her new shoes and forgot the orthoses. Pain has now resolved again. Video gait analysis demonstrates a marked improvement in hip and knee extension and a decrease in abnormal lumber flexion.
2. Patient B
Symptom Presentation Right sided heel pain for three months. This originally occurred following an increase in social walking. Worse after activity and upon rising after rest or sleep.
Diagnosis Plantar fasciitis.
Clinical Findings The right foot is maximally pronated in stance (no reserve of pronation available). This is due to an intrinsic foot problem, called a forefoot varus, in this case larger on the right than the left
Clinical Reasoning The greater pronation on the right causes lowering of the arch of the foot, increasing tension within the medial band of the plantar fascia. This increased tension results in injury of the plantar fascia at its origin from the calcaneus.
Treatment Custom functional foot orthoses to reduce pronatory moments were supplied. This reduction in pronation force reduces the tension in the plantar fascia and allowed the structure to heal. The appliances were posted, or 'wedged' at the level of the abnormality (the forefoot) while intrinsically utilizing a dell beneath the first ray so as not to impinge on normal foot function. The medial aspect of the arch of the appliance was not in contact with the foot, as this can prevent normal first ray mechanics and although heel pain can improve, move problems elsewhere.
Outcome The patient became pain free in approximately three weeks. Although initially pain returned if orthotics were not worn, within six months the appliances were only used in shoes utilized for activity.
Conclusion Podiatry is the profession specializing in the treatment, diagnosis and prevention of foot-based health problems. As with many professions, specialist areas within podiatry have developed, one of which is the area of gait dysfunction. Gait abnormalities may have a multi-aetiological background, and therefore the understanding of the foot based implications upon general health may be empirical to patients' wellbeing.
Bibliography
1. Dananberg HJ. Gait style as an aetiology to chronic postural pain – Part 1 – Functional hallux limitus. Journal of the American Podiatric Medical Association. 83(8): 433-441. 1993.
2. Dananberg HJ. Lower Back Pain: A Repetitive Motion Injury. In: Vleeming et al (Eds). Movement, stability and low back pain. The role of the sacroiliac joint. Churchill Livingstone, Edinburgh. 1997.
3. Harradine PD, Bevan LJ, Carter N. Podiatric Biomechanics Part 1: Foot based Models. British Journal of Podiatry. 11(1): 5 – 12. 2003.
4. Kirby KA. Foot and Lower extremity biomechanics: A ten year collection of Precision Intricast News Letters. Precision Intricast incorporated, Arizona. 1997.
5. Kirby KA. Biomechanics of the normal and abnormal foot. Journal of the American Podiatric Medical Association. 90(1): 30-34. 2000.
6. Lee WE. Podiatric biomechanics. An historical appraisal and discussion of the Root model as a clinical system of approach in the present context of theoretical uncertainty. Clinics in Podiatric Medicine and Surgery. 18(4): 555-684. 2001.
7. Root ML, Orien WP, Weed JH, Hughes RJ. Biomechanical examination of the Foot. Volume 1. Clinical Biomechanics Corporation. 1971.
8. Root ML, Orien WP, Weed JH. Clinical Biomechanics Volume II. Normal and Abnormal Function of the Foot. Clinical Biomechanics Corporation. 1977.
Comments:
-
robert jones said..
mine is a complex one.head injury 1978(fracture base of skull)made about 90% recovery.
always had slight ataxia but walking was back to normal until a few years ago when gait disturbance worsened.
was admitted for tests two years ago, nothing found on mri scans x rays etc.
was admitted again last year following lower back pain.mri scan revealed l5/s1 foraminal narrowing/stenosis,also slight bulging disc at l5.
have developed pes planus valgus inboth feet/worst on right,arch has completely dropped and metartarsals are starting to curl in.
have been seeing podiatrist on nhs who keeps giving me insoles which are not helping,it is got to the stage where they were causing me to fall,and a physio said i would be better of removing them.i have seen other podiatrists who charge a fortune for insoles(of the shelf)some of them dont even exanine my foot for movement,or whatch me try them out.
i am now seeing a podiatrist who seems to know how to treat me and he has made impressions of my feet along with computer imprints.i will be seeing him in a weeks time to try them out.
the main question is will decompression surgery help the gait disturbance?as the back pain has now stopped,or is it best to address the foot problem first.
i am 56 years old slim build and no other health problems.
ps i do smoke and find that if i sop smoking for longer than3 hrs my walking improves!
its a pity you are not nearer swansea as i would pay you a visit asap.