Positive Health Online
Your Country

Add as bookmark
Nutritional Care Of Peptic Ulcer
by Dr Mohan Krishnarao Kale(more info)
listed in nutrition, originally published in issue 165 - December 2009
Abstract
Peptic Ulcer is one of the most common diseases today. It refers to an eroded lesion in the gastric intestinal mucosa. An ulcer may form in any part of the digestive tract, which is exposed to acid gastric juice, but is usually found in the stomach (gastric ulcer) and the duodenum (duodenal ulcer). Nutritional Care/Diet is of utmost importance in the treatment of ulcer. The diet should be arranged as to provide adequate nutrition to afford rest to the disturbed organs, to maintain continuous neutralization of the gastric acid, to inhibit the production of acid and to reduce mechanical and chemical irritation. Before as well as after treatment, nutritional care is vital to prevent, heal and cure Peptic Ulcer.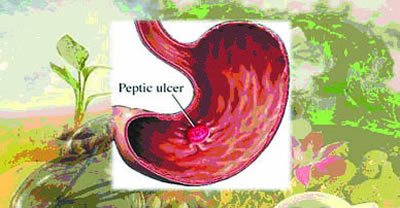
Introduction
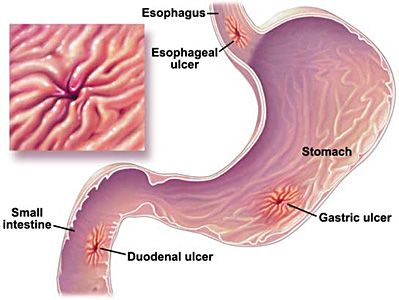
Peptic Ulcer is one of the most common diseases today. It refers to an eroded lesion in the gastric intestinal mucosa. An ulcer may form in any part of the digestive tract, which is exposed to acid gastric juice, but is usually found in the stomach (gastric ulcer) and the duodenum (duodenal ulcer). Duodenal ulcers are about ten times more frequent than gastric ulcers. They are more common in sedentary workers. The incidence of peptic ulcers is four times higher in men than women. Men are more affected by duodenal ulcers whereas women usually get ulcers in the stomach. Both kinds affect young to middle-aged persons, and are most common in the 35-40 age groups. Symptoms
The most common symptoms of peptic ulcer: - Sharp and severe pain and discomfort in the upper central abdomen;
- The pain is commonly described as burning or gnawing in character;
- Gastric ulcer pain usually occurs an hour after meals and rarely at night;
- Duodenal ulcer pain usually occurs between meals when the stomach is empty and is relieved by food, especially milk. It is often described as hunger pain;
- There is distension of the stomach due to excessive flatulence, besides mental tension, insomnia and gradual weakening of the body. It may also cause constipation with occasional blood in the stools. If an ulcer bleeds slowly, there is anaemia, while massive bleeding lead to shock, or even death if untreated.
Causes
- Peptic ulcers result from hyperacidity in the stomach. This strong acid secreted by the cells lining the stomach can be potentially dangerous and it may eat the lining of the stomach or duodenum producing, first, irritation of the stomach wall and eventually an ulcer;
- Dietetic indiscretion, like overeating, taking of heavy meals or highly spiced foods, coffee, alcohol and smoking are the main factors contributing to this condition. Alcohol is a very powerful acid producer and has a burning effect on the stomach lining. Coffee also increases the production of acid especially when it is taken black;
- The ingestion of certain drugs particularly aspirin, food poisoning, infections like influenza, septicaemia and gout may also cause ulcers;
- Emotional stress, excessive worry, anger, tensions, jealousy, and hurry also plays a major role in the formation of ulcers. Presumably stress and strain, hurried and irregular meals, and inadequate mastication are important contributory factor in ulcers.
Pathogenesis – Imbalance between mucosal defensive factors and aggressive factors
Defensive Factors
Prevent the stomach and duodenum from being harmed (self-digestion); Mucus – continually secreted, protective effect; Bicarb – secreted from endothelial cells, neutralized hydrogen ions; Blood flow – good blood flow helps to maintain mucosal integrity; Prostaglandins – stimulate secretion of bicarb and mucus and help promote blood flow, suppress secretion of gastric acid. Aggressive factors
em>Helicobacter pylori – gram negative bacteria, can live in stomach and duodenum; May break down mucus layer, inflammatory response to presence of the bacteria may break down defences, also produces urease – forms CO2 and ammonia which are toxic to mucosa; NSAIDS – inhibit the production of prostaglandins; Decrease blood flow, decrease mucus production and bicarbonate synthesis, promote gastric acid secretion; Gastric Acid – also needs to be present for ulcer to form – activates pepsin and injures mucosa; Pepsin; Smoking.
Treatment
Classes of drugs: Antibiotics, Antisecretory agents, Mucosal protectants, Antisecretory agents that enhance mucosal defenses, Antacids etc;
Nondrug therapy: Diet – change in eating pattern, 5-6 small meals a day, Smoking cessation, NSAID(analgesics) should be avoided whenever possible and avoid alcohol;
Raise the head of the bed, or lie on left side;
Decrease fat intake;
Nutritional / Dietic Control.
Nutritional Care
Diet is utmost importance in the treatment of ulcer. The diet should be so arranged as to provide adequate nutrition to afford rest to the disturbed organs, to maintain continuous neutralization of the gastric acid, to inhibit the production of acid and to reduce mechanical and chemical irritation. To achieve the above objectives, the following nutrient modifications are recommendedEnergy
Most patients suffering from active peptic ulcers are undernourished and therefore need an increased energy intake. However, since they are confined to bed the energy needs for activity are not utilized and make up the extra needs.
Proteins
A high protein intake is recommended to provide essential amino acids for tissue protein synthesis and thus promote healing. Proteins are also included because of their good buffering action. They may be increased by about 50 %. However meat proteins are to be avoided because meat extractives have a stimulating effect. Though milk protein has a good buffering action, the high calcium content of milk stimulates excess acid production hence, should be used in moderation. Eggs and other protein foods need to be included to provide essential amino acids.
Fats
Since fat delays the emptying of stomach, an increased intake is beneficial. However, fat is only moderately increased since patients suffering from peptic ulcers are generally middle aged executives who are also prone to atherosclerosis. Emulsified fats like butter, cream etc are better tolerated.
Carbohydrates
Carbohydrates are included to meet the energy needs. Foods containing harsh, irritating fibre should be avoided.
Vitamins
Requirements of nearly all vitamins remain normal. Adequate amount of vitamin C should be provided for the healing of ulcers and better iron absorption.
Minerals
Care should be taken to include sources of iron and calcium in the diet. Generally, bland diets are found to be low in iron and vitamin C due to the restriction in fruits and vegetables, and medicinal supplements may have to be given.


References
1. Malhotra S.L. New approaches to the pathogenesis of peptic ulcer based on the protective action of saliva with special reference to roughage, vegetable fibre and fermented milk products. Medical Hypotheses, 4 (1): 1-14. 1978. 2. FrankI. T., Jayaraj A. P., Clark C. G. Diet and Ulcer. The Lancet, 330( 8555) : 398. 1987.
3. Kuipers EJ, Thijs JC, Festen HP. The prevalence of Helicobacter pylori in peptic ulcer disease. Aliment Pharmacol Ther; 9(2): 59-69. 1995.
4. Vaira D, Menegatti M, Miglioli M. What is the role of Helicobacter pylori in complicated ulcer disease? Gastroenterology.113(S): 78-84. 1997.
5. Russell MK, Mueller C., Nutrition screening and assessment. In The A.S.P.E.N. Nutrition Support Core Curriculum: A Case-Based Approach: American Society for Parenteral and Enteral Nutrition,163 –186, 2007.
6. Walid H A. et al, Prospective Study of Diet and the Risk of Duodenal Ulcer in Men, American J Epidemiology 145(1):42-50. 1997.
7. Grace H E et al. Comparison of Coffee Intake and Coffee-Induced Symptoms in Patients with Duodenal Ulcer, Nonulcer Dyspepsia, and Normal Controls. American J Gastroenterology 85(10):1339-1342 .1990.
Comments:
-
Priya said..
is there any specified amount of energy to be consumed?
« Prev
Next »