Positive Health Online
Your Country

Natural Treatment Options for Acne Vulgaris
listed in herbal medicine, originally published in issue 200 - November 2012
Mild acne affects many teenagers at some point but also adults. Acne is a condition which can be effectively treated. In order to make most of the treatments available it is necessary to understand the underlying pathology of the condition.
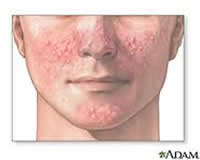
Acne is a hormonally driven condition which affects your pilosebaceous glands. Sebaceous glands are found on most parts of the body, except for the palms of your hands, soles and dorsum of the feet. Sebaceous glands are mostly found on the face and scalp, but also on chest and back. This explains the tendency for acne on these areas. The size of the glands differs hugely between individual and anatomical sites. These glands respond to circulating androgens (male hormones, which both men and women have) by producing sebum (fat).[6] Acne arises if the level of these circulating androgens is very high or the gland becomes overly sensitive to circulating androgens. Testosterone is the primary androgen associated with acne. It is produced in the adrenal glands, the ovaries in women and testes in men. Testosterone is both present in men and women.[1]
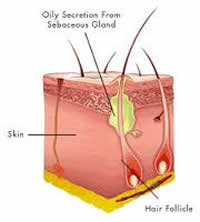
sebaceous gland
There are 4 key processes which occur to produce acne lesions:
- Increased production of sebum (oil);
- Excess keratin production within the hair follicle leading to follicular plugging;
- Increased bacterial activity within the follicle as there is enhanced colonisation with a bacteria called: Propionibacterium acnes (P. acnes);
- Release of inflammatory mediators into the follicle and surrounding dermis causing increased inflammation.[2]
The response of the body to increased circulation of androgens, begins to occur often at 7-8 years of age. Initially, the androgens cause changes in both sebocytes and follicular keratinocytes. This leads to microcomedone formation. Microcomedones are non-inflammatory lesions, which are the first signs of acne. Secondly, the androgens lead to an increase in sebum production.[5]
Sebum consists of lipids such as, triglycerides, waxes, free fatty acids and squalene, as well as debris of dead fat producing cells. Sebum supports the growth of the bacteria P.acnes, and as such acne cannot occur without the presence of sebum.[1]
In a normal follicle, keratinocytes are shed as single cells into the follicular channel and then excreted. However, some keratinocytes can remain adherent in the follicular channel leading to blockage, which can either be partial or complete.[6] Initially these blockages can lead to small changes known as microcomedones. It can take as long as 2 to 3 years before they become significant acne lesions. As the microcomedone becomes bigger and the swelling increases behind the blockage, comedones develop. These are always the precursor lesions to acne.[2]
Comedones can be open or closed. Open comedones are also known as ‘blackheads’ and arise where the blockage of the follicle is high up and contents of the follicle are pushed through the follicle opening and exposed to the air. Closed comedones are known as ‘whiteheads’ and their contents are not exposed to the air, as the blockage is deep down the hair follicle.[7] Both black and whiteheads occur during the non-inflammatory stage of acne. The blockage within the hair follicle allows for build up of sebum, which is an ideal environment for P. Acnes to proliferate.[4]
P. acnes exists on every skin surface and it tends to proliferate and colonise the hair follicle leading to inflammation, which in itself causes the release of pro-inflammatory cytokines, such as CD4+ T-Lymphocytes, which causes the initial formation of papules and pustules. White blood cells are attracted to the area of inflammation due to the increased amount of bacteria. Thus pus is formed largely from dead white blood cells.
Inflammatory mediations move out into the surrounding dermis and cause often more nodular and/or cystic lesions, which can in some cases lead to permanent scarring.[6] Nodules are larger than pustules and extend deeper into the layers of the skin, and caused by large comedones rupture, releasing their inflammatory contents into the surrounding skin. As those extend deeper into the surrounding skin, affecting dermis and epidermis, they may lead to scarring. Cysts are not as solid as nodules and will often occur where there are two or three nodules together.[3]
There are a number of useful medicinal plant extracts for the topical treatment of acne, which include:
Myrrh (Commiphora myrrha), is stated to possess antimicrobial, astringent, carminative, antiseptic and vulnerary properties, and has been traditionally used for furunculosis, wounds and abrasions. The German Commission E approved topical use for mild inflammation. Its volatile oil, gum and resin components are well documented. Phenol components of the volatile oil may account for the antimicrobial properties of myrrh.[9]
Another useful medicinal plant is Yarrow (Achillea millefolium). Yarrow is stated to possess astringent and antiseptic properties. Traditionally it has been used for bruises, fevers and swellings. Some activities documented for yarrow are associated with the azulene constituents. Antimicrobial properties have been documented by the sesquiterpene lactone fraction.[8]
The phytochemical properties of Liquorice (Glycorrhiza glabra) are also well documented and is particularly characterised by triterpenoid components. For example Carbenoxolone, an ester derivative of a triterpenoid constituent of liquorice, is well known for its use in ulcer therapy. Liquorice is stated to possess anti-inflammatory properties and can therefore be of use an in topical preparation for acne. Glycyrrhetinic acid has shown significant anti-inflammatory activity. Antimicrobial activity versus a number of bacteria has been documented for liquorice and attributed to isoflavonoid constituents such as glabridin, glabrol and their derivatives.[8]
Aloe vera is another useful topical agent for acne. Aloe vera gel is contained in the mucilaginous tissue that is found in the inner leaf of the plant, and should not be confused with aloes, which are the latex stored in tubules along the leaf margin. Aloe vera gel may be produced by a hand-filleted technique to remove the inner leaf, or by a whole-leaf extraction process where the aloes constituents (anthraquinones) are now usually subsequently removed (e.g. by charcoal filtration).[9]
The principal constituents of the gel are polysaccharides consisting mainly of polymannans, of which acemannan is the major one. Other constituents include glycoproteins such as aloctins, and various carboxypeptidases, sterols, saponins, tannins, organic acids, vitamins and minerals. Traces of anthraquinone glycosides may also be present in preparations.[9]
Aloe vera is used topically to aid wound healing from cuts and burns, including sunburn, and is used in many cosmetic preparations such as moisturisers. Its anti-inflammatory, immunomodulatory and antibacterial properties make it an ideal ingredient of topical acne treatments.[8]

salixalba
The bark of willow (Salix alba) can also be an effective ingredient for topical acne treatment. The bark of willow is reported to have analgesic, anti-inflammatory astringent properties. The bark of willow contains the phenolic glycosides salicin (up to 10%), acetylsalicin, salicortin, salireposide, picein, triandrin. Esters of salicylic acid, salicyl alcohol, and flavonoids and tannins are also present. The bark of willow is reported to have analgesic, anti-inflammatory, antipyretic and astringent properties.[9]
Another common plant known as German Chamomile (Matricaria recutita L.) is frequently used in topical applications for acne. The flowerheads of German chamomile contain essential oil composed mainly of (−)-α-bisabolol. Sesquiterpenes and proazulenes (e.g. matricarin and matricin) are also present. Chamazulene (1 to 15%), another volatile oil found in chamomile, is formed from matricin during steam distillation of the oil. Other constituents present in chamomile include flavonoids (apigenin, luteolin, quercetin, rutin), and the natural coumarins umbelliferone and its methyl ether, heniarin.[8]
German chamomile is used topically for haemorrhoids, mastitis and leg ulcers and general skin lesions. Many beneficial properties have been identified for flavonoids; one of the most popularly cited being their antioxidant activity. Other actions that are proposed to contribute to their biological effects include reducing inflammation, decreasing vascular cell adhesion molecule expression, increasing endothelial nitric oxide synthase (eNOS) activity, and inhibiting platelet aggregation.[9]
Historically, the relationship between adequate nutrition and acne has been highly controversial. Before the 1960s, certain foods were thought to exacerbate acne. However, subsequent studies dispelled these alleged associations as myth for almost half a century. Several studies during the last decade have prompted medics to revisit the possible links between nutrition and acne.
The association between diet and acne can no longer be dismissed. Compelling evidence exists that high glycaemic (sugar) diets may exacerbate and worsen acne, due to the effect of the insulin metabolism in the human body. In particular, evidence that the ingestion of certain fats, dairy products and starchy carbohydrates may exacerbate acne is currently under investigation. Other dietary factors implicated in acne include omega-3 fatty acids, antioxidants, zinc, vitamin A, and iodine.
Moreover, sebum production is controlled by androgens, which means that hormones play a big role in the condition. Stress, which is linked to the body’s stress hormone production, may also be implicated in exacerbating the condition.[10]
In sum, acne prone skin can be treated effectively with a number of phytomedical topical applications. However, the following advice may be useful to improve positive outcome:
- Harsh washing should be avoided;
- Spots should not be squeezed to avoid permanent damage of the skin such as scarring, especially if the lesions are red and pustular;
- Oily products should not be used on the skin;
- Moisturisers are needed on the skin between the lesions to avoid dryness. However, all products used should be labelled oil free and non-comodogenic;
- Foundation and cover-up make-up can make acne worse and should be used as little as possible;
- The patient needs to be aware that there are really no quick treatment options for acne;
- Low in the glycaemic index and food low in saturated fats may be beneficial in acne prone skin;
- Results can only be seen after weeks to months depending on each case
References
1. Zaenglein AL, Graber EM, Thiboutot DM, Strauss JS. Chapter 78. Acne
vulgaris and acneiform eruptions. In: Wolff K, Goldsmith LA, Katz SI, Gilchrest B, Paller AS, Leffell DJ, Editors. Fitzpatrick’s Dermatology in General Medicine 7e: www.accessmedicine.com/content.aspx?aID=2963025 . Accessed August 8, 2010.
2. Dreno B, Poli F. Epidemiology of Acne. Dermatology. 206(1): 7–10. 2003.
3. Zouboulis C, Piquero-Martin J. Update Future of Systemic Acne
Treatment. Dermatology 206(1):37–53. 2003.
4. Goulden V, Stables GI, and Cunliffe WJ. Prevalence of facial acne in adults. J Am Acad Dermatol. 41(4):577–580. 1999.
5. Gollnick H, Cunliffe W, Berson D, et al. Management of acne: a report from a global alliance to improve outcomes in acne. J Am Acad Dermatol. 49(1 Suppl):S1–S37. 2003.
6. US. Department of Health and Human Services, Agency for Health- care Research and Quality, Management of acne. Summary-Evidence Report/Technology Assessment: Number 17. AHRQ Publication No.01-E018. Rockville, MD: Agency for Healthcare Research and Quality; March 2001.
7. Purdy S, DeBerker D. Acne vulgaris. Clin Evid. 5:1714. 2008.
8. Plant Bioactives and Drug Discovery: Principles, Practice, and Perspectives (Wiley Series in Drug Discovery and Development) Valdir Cechinel-Filho.
9. Phytochemicals, Plant Growth, and the Environment (Recent Advances in Phytochemistry) by David R. Gang (31 Aug 2012).
10. Advancing Dietetics and Clinical Nutrition [Paperback] Anne Payne (Editor), Helen M. Barker (Editor)
Comments:
-
No Article Comments available