Positive Health Online
Your Country

Nutritional Approaches to Liver Detoxification
listed in detoxification, originally published in issue 33 - October 1998
Introduction
The liver is the most hard-working organ in the human body. It performs many functions that are vital to life. It plays an important role in digestion (breaking nutrients down) and assimilation (building up body tissues). It is the storage site for many essential vitamins and minerals, such as iron, copper, B12, vitamins A, D, E and K. Red blood cells, which are responsible for carrying oxygen around the body, are also produced in the liver and Kupffer cells help to devour harmful micro-organisms in the blood so helping to fight infection.
Among its many functions, the most important role of the liver is that of Detoxification. The liver detoxifies harmful substances by a complex series of chemical reactions. The role of these various enzyme activities in the liver is to convert fat soluble toxins into water soluble substances that can be excreted in the urine or the bile depending on the particular characteristics of the end product.
Every day our bodies are bombarded with toxins from both outside (exotoxins) – the polluted environment, medications, alcohol, cigarette smoke, car exhaust emissions and toxins from within the body (endotoxins) – the by-products of nutrient breakdown, hormones and bacterial waste products from the intestines. All produce harmful substances. It is the role of the liver to render these potentially harmful products into less harmful compounds.
The effects of exposure to toxins varies from individual to individual. Some people are highly sensitive to different endo and exo toxins. Others, because their bodies are more resilient and their livers can detoxify more efficiently, are not so sensitive.
When optimum nutrition is provided the liver operates efficiently. A great many people however, do not eat the right kinds of foods to provide the liver with everything it needs for the elimination of the extra toxins our bodies are exposed to on a daily basis. If nutrition is compromised through poor dietary and lifestyle habits, this will have implications on detoxification processes, and other organ functions will suffer as the body retains the toxins it cannot eliminate.
The rate at which the liver can eliminate toxins can determine an individual's susceptibility to toxic overload, which in turn can lead to symptoms of ill-health. When the liver becomes so overloaded with harmful toxins that the enzymes that break them down can no longer cope, the toxins build up and this then manifests itself in a specific disease state which, without the intervention of correct nutrition, can become a vicious circle of chronic toxic overload. This can be explained by the diagram above which vividly shows how toxic overload can manifest in chronic health problems. Many inflammatory conditions, such as arthritis, cardiovascular problems, headaches, chronic fatigue and premature ageing can all be related to a build up of toxins that the liver is unable to cope with, as shown in Figure 1 (below).
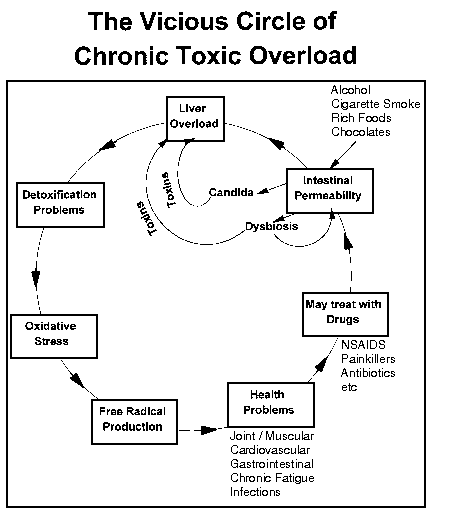
There are two stages of liver detoxification:Phase I and Phase II
Phase I is carried out by the cytochrome P 450 enzyme system and consists of oxidation and reduction reactions. Various nutrients are required in order for the Phase I detoxification system to be carried out efficiently. Cytochrome P450 reactions generate free radicals and this can cause secondary damage to cells. An adequate supply of key antioxidants and free radical quenches is therefore essential to prevent tissue damage. Reduced glutathione, superoxide dismutase and additional nutrients such as beta carotene, vitamin E, selenium and N-acetylcysteine will act as antioxidants.
Other nutrient cofactors required for cytochrome P450 reactions include riboflavin, niacin, magnesium, iron and certain phytonutrients such as indoles from cruciferous vegetables and quercetin have been shown to support Phase I detoxification.
The metabolites from this detoxification process are often potentially more harmful than their original toxic compounds and it is important for health that they are not allowed to build up. This is where Phase II detoxification comes in.
In Phase II glutathione conjugation is the primary pathway for these intermediate metabolites. Increased exposure to toxins as well as a poor dietary supply of glutathione can soon lead to glutathione depletion and increased damage from these highly reactive intermediates. Oral supplementation with reduced glutathione or N-acetylcysteine may help to increase glutathione levels in vivo.
Glucuronidation pathways in Phase II can be reversed by Beta glucuronidase enzymes produced by pathological bacteria and cause toxins to be reabsorbed increasing toxicity. Studies have shown that calcium d-glucurate, a natural ingredient found in certain vegetables and fruits can inhibit beta glucuronidase activity resulting in increased elimination of toxins. Supplements of calcium d-glucurate may also be taken to enhance the glucuronidation pathway.
Other nutrients which play vital roles in the Phase II pathway include amino acids glycine, cysteine, glutamine, methionine, taurine, glutamic acid and aspartic acid.
Glutamine plays a chief role in ammonia detoxification as well as helping to maintain mucosal integrity of the gastrointestinal tract.
In some people the detoxification pathways (Phases I and II) are out of balance. For example, if Phase I is more active than Phase II, a build up of reactive intermediate metabolites can occur which in turn can lead to tissue damage and disease. These people are referred to as Pathological Detoxifiers.
Pathological detoxifiers can be identified as those individuals who are highly sensitive to fumes e.g. paints and perfumes, react adversely to various pharmaceutical drugs and may have a reaction to drinking caffeine. Alternatively a liver detoxification test can pinpoint exactly how efficiently your liver is carrying out the detoxification process and if you are a pathological detoxifier.
There is now an extensive body of evidence indicating that diet plays a crucial role in modifying the body's detoxification pathways. Even in allopathic medicine grapefruit juice is utilised for transplant patients as grapefruit contains naringenin which slows down Phase I enzyme activity. This enables such drugs as cyclosporin – which is given to prevent organ rejection – to stay in the system for longer prior to the drug being detoxified. Pathological detoxifiers may also find it useful to include grapefruit juice in their diet.
Vitamins and minerals – particularly the B vitamins – play a major role, acting as cofactors for many enzyme systems including those of liver detoxification, therefore ensuring a plentiful supply of the B complex group of vitamins is of prime importance for optimum detoxification. Therefore, including plenty of whole grains which contain B vitamins in the diet as well as taking a good B complex supplement will aid the liver in this crucial role.
Depletion of vitamin C may also impair the detoxification process; vitamin C also prevents free radical formation. Vitamin C is found in citrus fruits and green leafy vegetables. However, in order to obtain optimum amounts supplementation is required. At least 1000mg a day is recommended.
Vitamin E and selenium are cofactors for glutathione peroxidase activity as well as being powerful antioxidants. (Vitamin E also works synergistically with vitamin C.) Today, our diets are very low in selenium due to the depletion of the soil of this vital mineral. Supplementation is therefore imperative.
Cruciferous vegetables such as broccoli, cauliflower, brussel sprouts and cabbage in the diet have been shown to enhance Phase I activities. It is thought that the indoles which are the active ingredients in these foods are the major contributors to this activity.
Zinc is another essential nutrient and acts as a cofactor for many enzyme systems. Zinc deficiency can cause a whole range of consequences. One important role that zinc plays is in the functioning of an enzyme alcohol dehydrogenase involved in the conversion of alcohols to aldehydes in Phase I detoxification. Therefore anyone who drinks alcohol should ensure they have optimum amounts of zinc in their diet.
Dietary Guidelines for Optimum Detoxification
The diet should include plenty of organic, unrefined, unprocessed foods, as fresh as possible and in their natural state. Fresh vegetables, fruits, whole grains and unrefined carbohydrates should make up the majority of the diet. Red meats, animal fats, sugars and refined foods should be avoided as should caffeine, other stimulants and alcohol.
Drink plenty of bottled water or diluted juice, at least two litres per day. A minimum of one daily serving of cruciferous vegetables and at least five servings of fresh fruit should be included in the daily diet. Protein sources can be obtained from lentils, soya, beans, nuts, seeds and fish and organic chicken.
In summary, therefore, it can be said that an efficient liver detoxification system is vital to health and in order to support this process it is essential that many key nutrients are included in the diet.
Many people choose to follow a detoxification programme, which may take many forms. However, it should be noted that any such programme should be supervised by a qualified nutritionist because when toxins are released too quickly this can be extremely uncomfortable and may cause headaches, fatigue, diarrhoea, irritability and lightheadedness. However, removal of toxins gives many positive health benefits, giving increased energy, clear skin, vitality and a general feeling of well-being.
References
Percival, M (Dr) (1997) 'Phytonutrients and Detoxification' Clinical Nutrition Insights Vol 5 No 2
Amber Ackerson N.D. Dietary Regulation of Detoxification Tyler Encapsulations
Bland, J (Dr) (1997) The 20 Day Rejuvenation Diet Keats Publishing
'Standard Detoxification Profile.' Application Guide Great Smokies Diagnostic Laboratory (1997)
'How to Detox' Here's Health (May 1998)
'Innovative Clinical Approaches to the Cascade of Chronic Illness' Nutri Ltd (1997)
'The Detoxification Process Simplified' Heathcomm International (1997)
Kaminski, M M.D Functional Medicine Symposium Course Notes (1998) The Gut Liver Connection
Comments:
-
No Article Comments available