Positive Health Online
Your Country

Craniosacral Therapy, Cranial Moulding and Baby Helmets
by Graham Kennedy RCST(more info)
listed in craniosacral therapy, originally published in issue 203 - February 2013
Craniosacral therapy is well known for its effective treatment of babies and children. Whilst babies are brought for treatment with a wide range of conditions, one of the more distressing for parents is severe unresolved cranial moulding. Although there are many different types of moulding patterns, one of the more common is known as plagiocephaly.
Also known as deformational plagiocephaly, positional plagiocephaly or flat-head syndrome, plagiocephaly is the medical term used to describe a flattening on one side of the back of a baby’s head.
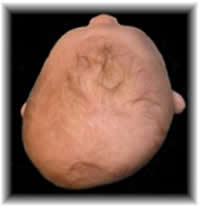
Plagiocephalic Head Shape
This flattening is usually accompanied by a bulging on the same side of the baby’s forehead, a bald area at the flat spot as well as ear and eye misalignments. Some estimates state that plagiocephaly occurs in up to 50% of all babies under a year old to some degree.
Another form of severe cranial moulding, known as brachycephaly is associated with both sides of the back of the head being completely flat. This particular moulding pattern is also associated with a head shape that is wider than it is long, and also has a high or “peaked” appearance.
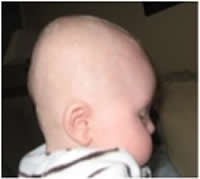
This extreme moulding can occur due to the fact that at birth the bones of a baby’s skull are not fully formed and have not fused together to make the familiar sutures seen in an adult skull. As a result, they remain susceptible to the effects of external forces acting upon them.
Usually, the first port of call for worried parents is their GP or health visitor. Conventional wisdom considers plagiocephaly to be essentially a cosmetic issue, with little or no physiological consequences. Its primary cause is considered to be due to babies spending more time (especially when sleeping) on their backs as a result of the back to sleep campaign, which highlighted babies sleeping on their fronts as a significant risk factor in Sudden Infant Death Syndrome (or SIDS).
As a result, the most commonly given advice is to have more ‘tummy time’ during the day in order to reduce the pressure on the back of the head, that it will flatten out in its own time, or if not the eventual growth of the hair over the area will serve to conceal it.
Many parents feel dissatisfied with these options and so seek out alternative forms of treatment. Two of the most common treatment options that parents look into are craniosacral therapy (along with other practitioners offering treatment in the ‘cranial’ field e.g. cranial osteopaths) and cranial remoulding orthoses, also known as baby helmets.
Before we look at the effectiveness and impact of these different treatment processes, let’s explore the different causes of these severe forms of cranial moulding.
Causes of Severe Cranial Moulding
As a result of the structure of a baby’s skull, cranial moulding is almost always associated with external forces acting upon the different cranial bones and distorting their natural positions. One important exception to this is a condition known as craniosynostosis, which is a premature fusing of one or more of the cranial sutures. This rare congenital condition (affecting 1 in every 2500 to 3000 births) needs to be medically diagnosed and treated, most commonly through surgery.
Aside from craniosynostosis, the causes of cranial moulding can be placed into three main categories:
- Prenatal factors
- Birth factors
- Postnatal factors
Prenatal factors - the main prenatal causes of cranial moulding, are due to compression of the cranium as a result of reduced inter-uterine space. This can occur as a result of uterine fibroids, an asymmetrical uterus, a reduction of amniotic fluid, multiple pregnancy or from the baby’s head getting stuck in an unfavourable position (e.g. breech with head wedged under mother’s ribs) towards the end of pregnancy.
Birth factors - it is during birth that the baby’s cranium experiences the most intense compressive forces as a result of being squeezed through his mother’s pelvis. Whilst moulding of the cranium at birth is a normal physiological process, if the baby experiences any aspect of the birth as stressful, distressing or even traumatic, these cranial compressions can become more firmly locked into the system along with high levels of shock, neurological charge and emotional intensity.
The moulding pattern produced by babies with both plagiocephaly and brachycephaly are typically associated with posterior (back to back) presentations. This occurs as a result of the baby’s occiput (the cranial bone at the back of the head) being compressed against the mother’s lumbo-sacral promontory. If a baby has been in this position for an extended amount of time, or if the contractions have been quite intense (as occurs with induced births), then the moulding produced may be more severe.
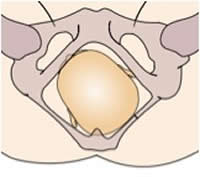
Posterior Birth
Intense compression of the occiput can also occur during the last stage of labour, when the baby is negotiating his mother’s pelvis outlet. During this time, the baby’s face is pressing directly against his mother’s sacrum and the occiput is being dragged and compressed by the pubic bone.
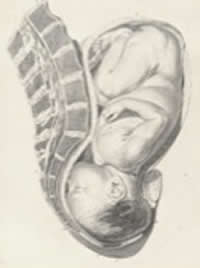
Compression of Occiput
Rotational forces introduced into the baby’s cranium, neck and body during the rotational stage of birth are also instrumental in the development of plagiocephaly and other severe moulding patterns. These forces can create a preference for the head to turn towards one direction as opposed to the other. In extreme cases, this can manifest as torticollis.
Torticollis is a contraction in one of the sternocleidomastoid muscles in the neck, causing the head to preferentially turn or tilt more towards one direction. Where babies are unable to turn their heads equally to both sides, they will favour the side of the easiest rotation. This leads to increased pressure being put on that side of the occiput, especially if the baby has weak neck muscles, or for some reason has reduced control of head movements. This positional preference can then get locked into the system and becomes reinforced every time the baby lies down on his back.
It may be worth mentioning here that these factors do not in any way justify the increased use of caesarean sections over vaginal births. Whilst elective C-sections are performed in some countries in order to optimise cranial symmetry, it is by no means a certainty. In fact, both of these moulding patterns can be found in babies born by C-section, where the head has been compressed by the pelvis (or the ribs) for some considerable time. In addition to that, C-sections are not free from their own consequences to the baby. They can introduce significant amounts of shock into the baby’s system, even where there has been little or no cranial compression.
However, there is certainly no guarantee that babies born by C-sections will be free from severe moulding patterns. I have seen many babies born in this way who have significant moulding. These patterns can arise as a result of many different factors depending on whether the section was an emergency or elective.
Other significant risk factors include prematurity (the cranial bones of premature babies are softer and therefore more vulnerable to compression than those of full-term babies), low birth weight, prolonged labour, use of forceps, ventouse (vacuum extraction) and induction drugs.
Post-natal factors - it is these factors that are considered to be the dominant causes of severe cranial moulding. As previously mentioned, chief amongst these is the increased prevalence of babies spending more and more time on their backs, especially when sleeping. Other associated factors include increased amounts of time spent in car seats and baby carriers as well as torticollis and other problems affecting rotation of the neck.
The importance of these post-natal factors in the development of cranial moulding patterns is lent credence due to the fact that many parents report that their baby’s heads seem symmetrical at birth but start to develop strong asymmetries several weeks later. In my experience, these post-natal positional factors are secondary rather than primary causes, in that they have, over time served to exacerbate and exaggerate the pre-existing compressional and rotational patterns present from the baby’s prenatal or birth experience.
Potential Side-Effects of Severe Cranial Moulding
The Institute of Child Health at the University College of London states that “There are no symptoms associated with plagiocephaly other than the flattened appearance of the back of the head - either evenly across the back or more on one side. It does not cause any pressure on your baby’s brain and development will not be affected by it in later life. Its importance is entirely cosmetic.”[1]
Whilst this is the most commonly heard view, it is not necessarily the most accurate. We need to understand that there are both mechanical and non-mechanical forces at work with these patterns. The mechanical forces arise as a direct result of the deformation and compression of the cranial bones and sutures. These compressions can adversely affect both blood vessel and cranial nerve function with a number of significant effects. These include problems with amongst other things hearing, balance and co-ordination, eye movement, sucking and swallowing and even visceral dysfunction.
The non-mechanical forces include the effects of the shock that introduced the severe compressive forces in the first place. One of the most significant effects of shock is to disrupt the integrated functioning of the brain and nervous system. This combined with the mechanical factors could leave these babies at greater risk for developmental delays, motor and sensory problems and even behavioural and learning difficulties later in life.[2,3,4]
Treatment
In order to treat the different conditions associated with severe cranial moulding effectively, we need to differentiate between treating the cause and treating the effect. The effects are the actual symptoms themselves. Chief amongst these is the distorted head shape, although as we have seen there may also be other associated symptoms as well.
The cause of these patterns, however, is the intense compressive forces experienced by the baby during some of his earliest experiences. These compressive forces are almost always accompanied by significant levels of shock, combined together with intense emotional content. As a result, the degree of unresolved moulding is often considered representative of the amount of unresolved shock present within the baby’s head and body.
As I mentioned earlier, the most common treatment approaches are as follows:
- Do nothing – assume that the remoulding process will occur on its own;
- Increased tummy time during the day - to take pressure off the back of the head;
- Cranial orthoses – baby helmets;
- Craniosacral therapy / cranial osteopathy.
Do nothing - in this situation, the assumption is made that the natural corrective forces of the body will be sufficient to resolve whatever moulding patterns may be present. The principal reason why moulding patterns stay unresolved is that these natural forces have been overwhelmed by more intense external compressive forces. Whilst a certain degree of moulding does resolve on its own, these deeper patterns are associated with forces that are greater than, and have therefore overwhelmed the natural corrective forces of the body.
This option could be considered at worst to treating neither the cause nor the effect, and at best to only treating the effect.
Increased ‘tummy time’ - this option is recommended in order to reduce the amount of time that babies spend on their backs during the day, in order to take some of the pressure of the already compressed cranium. It is still recommended, however, that babies should sleep on their backs. This recommendation comes from research into cot death, which found a relationship between a baby’s sleeping position and incidences of SIDS.
Plagiocephalic babies have often been described as less active when lying on their backs, and do not use their upper body and arms as much as non-plagiocephalic babies. This can lead to significant delays in such important milestones as sitting unaided and crawling.
Encouraging the baby to spend more time on his front (prone) is important in terms of helping to reduce the moulding pattern, but it is also a major factor in helping a baby meet its developmental milestones.
Unfortunately, this recommendation is not always easy to implement. Some babies have developed positional preferences that are often based upon their earlier prenatal and/or birth experience. For example, many babies with prenatal and/or birth related umbilical shock may have difficulty, or get distressed lying on their tummy where pressure is being placed directly onto the abdomen. Other babies, with different experiences (e.g. posterior presentation babies) may have difficulty lying on their backs. Babies with severe plagiocephaly will often feel very unstable when placed on their fronts and may readily roll back to their more ‘normal’ supine position.
In order to fully address these issues, it is important for practitioners to be able to assess and treat not only the mechanical compressive and rotational forces within the babies cranium and body, but also to help resolve the deeper factors that are often holding these in place.
Cranial Orthoses - the use of cranial orthoses, or baby helmets, to treat severe cranial moulding patterns has been on the increase over the last few years. The helmets, which consist of a plastic shell lined with a foam padding can be very effective at reducing the severity of any severe moulding.
The helmets are all custom-made for each baby once an accurate ‘map’ of the baby’s cranium has been made with a portable scanning device.

Baby Helmet
The aim is for the helmet, which needs to be worn constantly for several months, to apply a gentle corrective pressure to the bones of the skull, thereby helping to ‘guide’ them back into place. Regular follow-up appointments are made in order for the helmet to be adjusted to the baby’s growing and changing head shape.
The best results are achieved in babies between 4 and 7 months of age. Older babies can be treated (up to around 14 months of age), but the improvements may not be as significant and the treatment process will often take much longer.
As these images[5] show, helmets can be very effective in re-moulding the shape of the baby’s cranium back towards a more ‘normal’ head shape.
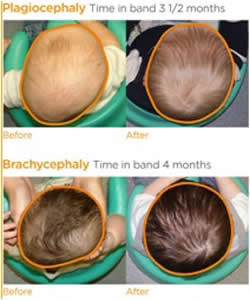
Remoulding Using Baby Helmet
Many cranial osteopaths are also now recommending them as either a supplement or an alternative to their treatment. Stuart Korth, the director of the Osteopathic Centre for Children in London has said “I used to be against helmets but have since changed my mind. They offer the best cosmetic solution for a good many cases of plagiocephaly, and so far, I have seen no adverse effects.”
Korth then goes on to add “Paediatric osteopathy is of value in most cases of plagiocephaly. Cosmetic improvement [my emphasis] is most likely with a helmet, though.”[6]
So, whilst the use of baby helmets can be effective in treating the ‘cosmetic’ aspects of severe cranial moulding, what happens to the underlying compressive and rotational forces, shock and emotional issues that go together to hold the moulding pattern in place? In order to answer this, we need to recognize that there are a number of factors that helmets fail to address.
- The first factor is that helmets can be seen as doing for the cranium of the baby what braces do for the teeth of the older child / adult. Whilst both of these are considered corrective from a cosmetic viewpoint, the principle that they are based upon is that of a static internal system that can be easily moulded without any adverse reactions.
All practitioners in the ‘cranial’ field recognize that all of the physiological structures of the body, including the bones of the head and the face, express a subtle innate movement. This movement is considered to be in direct relationship to the deepest expression of Health within us. This means that where these movements are truly free, then health will be a natural response. However, if these movements become inhibited in any way, then health (whether physical, emotional or psychological) will be compromised in some way.
Moulding the cranium, and indeed the teeth based solely on external criteria (i.e. what looks right) can actually inhibit the subtle movements of the associated bones, often creating a knock-on effect of inertia elsewhere within the body.
- A second factor comes into play when we consider the deeper forces at work within the moulding pattern. As we have seen, these can be divided into both mechanical and non-mechanical forces. The effects of the mechanical forces are clearly seen as distorted compressive and rotational patterns affecting the shape and positional integrity of the different cranial bones.
However, these patterns are not restricted to the cranium. As a result of the continuity and inter-relationships of the different tissues, these patterns extend throughout the body affecting a variety of structures including the face, neck, spine, diaphragm and pelvis.
Whilst helmets may be effective at re-moulding the shape of the cranium, they are unable to address these more extensive tissue patterns. As a result of the changes instigated in the cranium, the patterns in the rest of the body will have to adapt in specific ways in order to establish a new state of balance. Some of these adaptations may actually cause some of these tissue patterns to become more firmly held within the body.
- The final factor is the fact that helmets also fail to address the non-mechanical forces at work within the moulding pattern. These forces are related to levels of shock and emotional overwhelm that commonly get integrated within the whole-body tissue patterns that are associated with plagiocephaly and other severe moulding patterns. In my experience, it is possible, and even quite common to correct the more mechanical aspects of the moulding pattern but to leave the non-mechanical aspects unresolved. In situations such as this, these forces will continue to affect the psyche and physiology of the baby as he grows and develops throughout his life.
So, what are we to make of all this? Does it mean that helmets are bad for babies? In my opinion, the answer to that is no. Most parents whose babies have some form of severe cranial moulding will be most concerned with the cosmetic appearance. If this can be easily and readily corrected, either through the use of helmets or using them in combination with some form of cranial treatment so that their effects can be continually monitored, then their initial concerns have been met.
However, in understanding the deeper dynamics at work with cranial moulding issues, it falls to us as practitioners to inform parents that there are also other issues to consider beyond simple cosmetic ones. As a result, helmets only address the effects of the condition and not the causal factors.
Craniosacral Therapy - in the previous section, I have outlined some of the underlying principles upon which craniosacral therapy is based. Cranial therapies can be highly effective in treating not only the mechanical patterns, but also the non-mechanical forces that work together to create severe moulding patterns. However, this does not mean that all practitioners will work in the same way, and even that one practitioner is as effective as the next.
What is less well-known is that different practitioners will emphasise different aspects of the work in their practices, based upon their interests, experience and skill levels. Many practitioners are highly skilled at working with more mechanical issues, but may have little understanding or awareness of the non-mechanical forces. There tend to be fewer practitioners around who include working with the shock and emotional content of these patterns.
For effective treatment, most babies with severe cranial moulding will need to resolve the deeper emotional and shock-related issues before the mechanical aspects of the moulding pattern can be fully addressed. It is highly recommended that parents take the time to find a practitioner who they not only feel comfortable with, but also has experience in working in both of these ways with babies.
References
1. Taken from www.ich.ucl.ac.uk/gosh_families/information_sheets/plagiocephaly/plagiocephaly_families.html
2. Speltz M, et al "Case-control study of neurodevelopment in deformational plagiocephaly" Pediatrics DOI: 10.1542/peds.2009-0052. 2010.
3. Balan, P. et al, Auditory ERP’s reveal brain dysfunction in infants with plagiocephaly, J. Craniofac. Surgery, 13(4), p. 520-525. 2002.
4. Miller, R, and Clarren, S, Lon-term developmental outcomes in patients with deformational plagiocephaly. Pediatrics, 105(2). 2000.
5. Photo taken from www.londonorthotics.co.uk//plagiocephaly/locband.html which is the website for the London Orthotics Consultancy which specialises in the production and fitting of these helmets.
6. Quote taken from www.babyworld.co.uk/information/baby/health/flathead.asp
Comments:
-
No Article Comments available