Positive Health Online
Your Country

The First Chinese Medicine Degree Programme Outside China
listed in chinese oriental medicine, originally published in issue 32 - September 1998
The watershed for complementary medicine/therapies (CMT) was in 1993 when the British Medical Association acknowledged that CMT's rise in popularity was not due to a "passing fashion". For Chinese medicine 1997 must be viewed as the final breach in the cultural frontier when Middlesex University (MU) and Beijing University of Traditional Chinese Medicine (BUTCM) designed and validated a joint five year full-time BSc (Hons) Traditional Chinese Medicine (TCM) programme. This unique programme is based on the curricular contents recommended by the State Administration of Traditional Chinese Medicine (SATCM) in China for its universities of TCM including BUTCM. In China, the curricular content and the practice of TCM or Chinese medicine (CM) are regulated and controlled by the SATCM which then delegates the process of delivery to the Universities and colleges. On completion, SATCM issues the degree through these educational institutes.

Students studying Chinese Medicine at Middlesex University
The programme sets down the standards and quality for future CM curriculum outside China. One of the external validating panel called the programme "the gold standard" for CM education. In future, patients will have a reference point to assess the knowledge and skills behind a CM qualification and the quality of treatment they should receive. They will be able to check the bona fide status of the practitioners graduated from the Middlesex University by accessing MU's live register of its graduate practitioners. MU, in the absence of a Statutory Regulatory Body for CM, is required to set up its own CM Ethics Committee and together with the live register to "police" the professional conducts of its graduate practitioners until a regulatory body is set up.
This validated programme is approved and accredited by the SATCM in China. It is also approved for Higher Education Funding Council For England (HEFCE) funding and by the Department of Further Education and Employment (DFEE) for mandatory grants. The programme marks the beginning of a new era in the history of CM. It is a major achievement in academic collaboration between BUTCM, the foremost university in CM, and MU, a modern and visionary university. This programme, the first of its kind outside China, has proved very popular and is embraced by existing CM practitioners.
Context
The practice of CM in China and among overseas Chinese communities dates back many thousand years. Only recently has it gained popularity outside China. Much of this popularity is due to the few pioneers who had the vision and the conviction to introduce TCM into the UK. CM education and training have remained inside China, possibly due to linguistic, cultural and political factors. Nevertheless, these pioneers successfully gained CM knowledge and skills in China by learning the Chinese language first and then studied CM in Chinese. This could last as long as eight to ten years instead of five years! They had nevertheless successfully achieved their goal to become qualified and skilled practitioners. Some of them went on to successfully train others in the art of Chinese medicine and to ensure continuity.
There is evidence to support that Chinese Medicine is especially effective in the treatment of chronic diseases such as skin conditions, arthritis, malaria, cancer, and chronic pain affecting the spine, joints, and muscles (Lewith et al 1996). Similarly, evidence suggests that more and more people are willing to pay for their complementary medicine and therapies including CM, and in some cases their insurance company will refund the cost. Prince Charles (1997) called it "a very real social phenomenon".
a) The National Association of Health Authorities and Trusts (NAHAT) report (1993) found that "The vast majority of purchasers have a positive attitude to funding complementary therapies".
b) The Department of Health permitted General Practitioners to employ complementary therapists. Accordingly, "It is open to any family doctor to employ a complementary therapist to offer NHS treatment with their practice" (Dorrell 1991).
c) The current government wrote in 1994 that "In principle, complementary therapies that have value in health care should be available to NHS patients. It is a necessary part of good practice that general practitioners should have access to a wide choice of therapeutic approaches." (Primarolo 1994).
The British Medical Association (BMA), which in its 1986 report dismissed Complementary Therapies as "passing fashion", has since had a change of policy. In 1993, amidst increasing interest in complementary therapies (CTs) among medical and health care professionals, the BMA called for improved training and education within complementary medicine and recommended that:
• "Priority should be given to research in acupuncture, chiropractic, herbalism, homeopathy, and osteopathy as the therapies most commonly used in this country";
• "The Council of Europe Cooperation in Science and Technology project on non-conventional therapies be approved by the UK Government";
• "Accredited postgraduate sessions be set up to inform clinicians on the techniques used by different therapists and the possible benefits for patients… consideration should be given to the inclusion of a familiarisation course on non-conventional therapies within the medical undergraduate curriculum."
The recommendations also challenged the CMT practitioners to be evidence based and to open up to public scrutiny, in particular from the scientific community.
Goldbeck-Wood (1996) reported that "Complementary medicine is gaining in popularity worldwide, with increases in the number of practitioners and the number of patients consulting them … one in ten people in Britain consults a practitioner of complementary medicine each year".
HRH Prince Charles (1997) who is a believer in alternative medicine, acknowledged that tremendous advances have been made in scientific and biological research, to the extent that conditions once thought untreatable could be cured. However, he argued that "clearly this alone is not fulfilling all our health care needs as large number of people are paying to seek help from complementary medical practitioners. We simply cannot ignore what is a very real social phenomenon." He asked that orthodox and complementary medicines collaborate with each other to create what he calls a "more patient centred health care."
This phenomenon can only be partly attributed to an expansion in information and knowledge about health promotion available in the public domain. This may have broadened the responsibility for health. Similarly, there were substantial changes in the health care services as the result of:
• changing patterns of health and disease
• enormous demographic shifts
• growing complexity of health and welfare services
• increase specialisation in different professional health care provision.
The Patient's Charter may also have contributed to the rise in the interest in Chinese Medicine. The Charter offers patients, in many cases for the first time, full access to information about their health, their treatment and outcomes enabling them to make informed decisions and choices.
The implications for Chinese medicine
There is now a rush to open Chinese Medicine clinics. This is reminiscent of the American gold rush or the massive growth in Chinese Takeaways in the 70s & 80s. Such a practice has serious implications especially in the aspects of safety and competence. I alluded earlier to how some of the pioneers had worked very hard to introduce Chinese Medicine into the UK. These successes are already overshadowed by reports of abuse which so concerned Professor Zhang Wenkang, the then Deputy Minister of Public Health and Director of the SATCM, that he had to advise that "Non-doctors who acquire some knowledge from short courses should not practise (Chinese) Medicine". Tomlinson (1996) as if to emphasise Professor Zhang's point, also reported that "China is tightening supervision of Chinese Medicine and Pharmacology courses for foreigners and will stop institutions from granting advanced training certificates to non-medically trained students."
Due care and responsibility towards the public safety must be exercised in the absence of a regulatory body. It would be such a pity to undo the pioneering work of those who struggled against all odds to study successfully Chinese medicine and introduced it into the UK to benefit the public, in particular those with chronic conditions. The above report was not suggesting that only people qualified in orthodox medicine can learn and practise Chinese medicine, this would have serious implications for China itself because most of its Chinese medicine doctors are not qualified in orthodox medicine (OM) but have learned some orthodox medicine. Rather, the short courses are available for the bona fide OM practitioners.
Thus, the actions taken by China so far to monitor the roles of the Universities of Chinese Medicine in the promotion of Chinese Medicine are very valuable in confidence building among orthodox medical practitioners. It could go a step further by standardising the postgraduate programmes for qualified OM practitioners. The programme could include adequate understanding of Chinese medical philosophy to ensure the art of Chinese medicine does not become a technique to be rigidly applied and followed.
Chinese medicine and the curriculum approach
Chinese medicine is both a holistic system and a single discipline which offers many methods to treat a condition. Previously, practitioners had studied all methods and may have practised most of them. With increasing knowledge in the field of Chinese medicine and the expansion of practice, practitioners have begun to specialise in fewer methods (we now refer to them as "branches"). These branches are shown in Diagram 1.
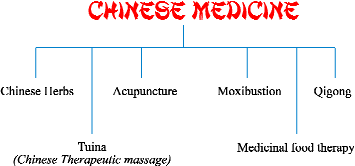
Diagram 1: The Branches of Chinese Medicine
These methods are effective singularly, or in partnership with one another, or all together in achieving the primary Chinese medical principle that health and illness are aspects of one thing; the balance of yin and yang. Chinese medicine is based on eight basic diagnostic principles: of yin and yang; interior and exterior; cold and heat; and deficiency and excess. The aim of every treatment is to achieve one of the following outcomes:
• to tonify / strengthen / nourish / raise yang
• to tonify/strengthen/nourish/raise yin
• to eliminate/dampen excess yang
• to eliminate/dampen excess yin
Orthodox medicine includes general medicine and surgery. In both medicines, there are sub-specialities.
The approach taken by MU and BUTCM is very radical. The programme's intentions are to:
a) produce practitioners of comparable academic levels, professional skills and competence as their contemporary peers studying in China, addressing the concerns expressed in NAHAT document (Worth, 1997) to safeguard the public interest;
b) meet the needs of the West in
accepting that orthodox medicine is the latter's predominant health care modality, so that CM practitioners can work collaboratively with OM colleagues to enhance the quality of life for patients;
c) modernise the CM programme but still underpin it with the traditional principles by dedicating one third of the medical content hours to Western biomedical sciences to enable the practitioners to cope with medical emergencies; and introducing research knowledge and skills as an integral part of their practice in order to facilitate evidence-based and reflective practice;
d) deliver the programme outside China in the English medium jointly by BUTCM and MU staff with input from University College London Medical School in orthodox clinical medicine;
e) broaden and enrich the students' clinical experiences by undertaking a six-month hospital-based internship in China;
f) include business studies reflecting the need to prepare students to work independently.
g) develop the students' knowledge and skills beyond technician level to that of reflective practitioners who will be able to diagnose and prescribe from evidence-based knowledge and skills; and be responsible and accountable for their actions.
The programme's uniqueness
The programme claims to be both the first of its kind and unique. It sets out a clear benchmark for quality and standards in accordance with the Higher Education's Quality Assurance Agency in the UK and SATCM in China for future TCM programme development with partners; it has received approval and accreditation from SATCM, the highest authority in TCM in China; the students are registered with both BUTCM and MU; the programme will be jointly delivered by MU and BUTCM; Both MU and BUTCM accept the enormous responsibility to be undertaken in setting up the programme's own "policing" arm – the Chinese Medicine Ethics Committee which will monitor the practices of its graduates. A live register of its graduates will be held at MU's Academic Registry. It is freely accessible to the public to confirm the bona fide status of the practitioners from whom they are seeking medical assistance.
The detailed breakdown of the programme offered below supports the programme's claim to uniqueness:
• 1440 hour's foundation including the core elements like; the basic theory of CM: theories of; yin-yang and the five elements, zang-fu organs, qi, blood and body fluids, the meridian, etiology and pathogenesis; and the principles of prevention and treatment;
• 1128 hours for Chinese herbal medicine/or acupuncture & moxibustion of which 50% is practice;
• 1100 hour's western biomedical science with input from orthodox medical staff;
• 540 hours in personal skills, ethics and law;
• 360 hour's Mandarin language;
• 360 hours in research principles, methods and processes;
• 270 hours in managing small business and other complementary therapies.
Challenges to this programme and the Scope of Practice
The recommendations of the two recent influential reports contributed much to the final outcome of this programme: NAHAT's guidelines (Worth 1997); the Scottish Office Department of Health (1996). The graduates will:
• have a biomedical understanding of patients' conditions;
• recognise complex and unusual conditions and know when to seek assistance;
• acknowledge their own limitations to practise within the guiding principles of the Scope of Practice;
• understand the effects of Chinese Medicine and Western drug interactions;
• understand Western clinical diagnostic techniques and laboratory test results;
• communicate effectively with orthodox medical colleagues.
The impact of Chinese medicine outside China
This programme will have a significant impact in the practice of Chinese medicine beyond the shores of the UK, benefiting the public who are seeking both quality and safe CM treatment. It is extending the good work of the first generations of CM practitioners. It will give further impetus to placing CM practice and treatment on a research based footing as the practitioners will begin to introduce researched evidence to enhance the credibility and effectiveness of their practices. CM is not a threat to other methods of regaining health. In China, the birthplace of CM, orthodox medicine is very much alive and in demand for its own merits. CM has much to offer to complement orthodox medicine. David Morgan (1997) gave a very interesting account from available published literature, database and Internet material on HIV/AIDS, of the benefits of Chinese medicine in enhancing the OM treatment of this disease process.
The birthplace of CM will be challenged to;
• use high tech to communicate its knowledge and skills;
• lead the transformation and explosion of interest in CM to ensure quality, safety and change in health care responsibility;
• provide leadership in safe practice and treatment with CM;
• to make its large clinical research data available to practitioners outside China;
• regulate the quality and safety of herbs and instruments used;
• be more research oriented and use research based practice.
The practitioners will be challenged to;
• deliver safe and effective treatment;
• collaborate and work interprofessionally to contribute to the World Health Organisation's target to achieve "Health for All by the Year 2000";
• provide concise and essential information to the public to enable them to make informed choices;
• practise research based medicine as well as conduct their own research to build up their knowledge.
Quality Assurance
In the absence of a Statutory Regulatory Body or a unified professional body, the University has established its own TCM Ethical Committee to regulate the professional conduct of its graduates. A unified professional body is a large family of practitioners who may practise one or more of the CM branches. These branch members (sub-specialists) work to the professional body's vision and objectives. This will provide a strong unified voice for Chinese medicine and its practitioners. The students are offered by BUTCM the opportunity to link with their own students for peer support, the exchange of ideas and publication of research projects. As an academic subject, both MU and BUTCM must demonstrate their capacity to nurture the programme and deliver the quality standards set by HEFCE in the UK and SATCM in China.
Conclusion
Middlesex University in developing this joint programme with BUTCM and acknowledging the pioneering work already available, is to facilitate and take the practice of CM to an evidence-based level. It is also hoped that future programme designers will find this collaborative programme helpful. This explains why a detailed curricular content is offered above. It also attempts to clarify the misunderstanding over the term "CM".
This development also expects China to provide "leadership" for colleagues outside China to emulate including research and evidence-based practices to support the practitioners. Making available the vast number of research papers will be most welcome and will be a boon for the CM practitioners outside China.
A period of reflection is also very important to ensure the continuing quality growth of the popularity of CM outside China. Popularity must be matched with credibility and acceptance by other health care professionals. There is now an urgent need to look at ways to create a body similar to the General Medical Council, to provide unified and strong leadership for all CM practitioners who are doing so much to contribute to the overall public health through supporting their orthodox colleagues.
Acknowledgement
To develop an academic programme is never an easy task and to develop this joint programme has been even harder with complex and complicated human interactions and cultural values. The success of this programme is very much the collaborative effort of many colleagues both in the UK and China. There are too many to name and to them I would like to acknowledge with gratitude their effort and support. I would like to say a special "thank you" to Drs PC Chang, JH Chen and Lily Cheung who have given much of their busy time to advise on the development of the programme.
References:
BMA (1986), Alternative Therapy: Report of the Board of Science and Education, London: British Medical Association
BMA (1993), Complementary Medicine, new approaches to good practice, Oxford; Oxford University Press BMJ, July 1996
Coward R (1986), The whole truth: the myth of alternative medicine, London Faber & Faber
de Wit (1981), Quoted in BMA (1986), Alternative Therapy: Report of the Board of Science and Education, London: British Medical Association
Goldbeck-Wood S: Complementary medicine is booming worldwide; BMJ Vol 313 20 July 1996, p131
HRH Prince Charles (1997) quoted in The Times, 22.10.97
Lewith G et al (1996), Complementary Medicine: an integrated approach. Oxford University Press, Oxford
Morgan D (1997), HIV/AIDS and complementary medicine: seeking information on alternative treatments. The AIDS Letter, No 63 Oct/Nov 1997, The Royal Society of Medicine Press.
NAHAT (1993), Complementary therapies in the NHS (research paper No. 10) London: National Association of Health Authorities and Trusts.
Scottish Office Department of Health (1996), Complementary Medicine and the NHS – an examination of Acupuncture, Homeopathy, Chiropractic and Osteopathy, The Stationery Office
Tomlinson R(1996): China tightens up TCM courses; BMJ vol 312, 20 April 1996.
West R (1992), Alternative medicine: prospects and speculations. In Saks M (ed): Alternative Medicine in Britain, Oxford: Clarendon Press
Worth C (1997), Guidelines for selecting practitioners of complementary and alternative medicine within the health service 1997/1998
World Health Organisation (1978): Alma Ata 1978 Primary Health Care, Geneva, (Health for All Series, No.1)
Comments:
-
No Article Comments available