Positive Health Online
Your Country

Every Child Can Grow an Attractive Face - Mouth Breathing Causes Crooked Teeth
listed in breathing, originally published in issue 183 - June 2011
Sleep that knits up the ravelled sleeve of care
The death of each day's life, sore labour's bath
Balm of hurt minds, great nature's second course,
Chief nourisher in life's feast.
~William Shakespeare, Macbeth
Allergic rhinitis is an extremely common health problem affecting up to 40 million in the United States and between 10-25% of the World's population[1] with the actual prevalence varying within and among countries.[2,3,4,5] The British Society for Allergy and Clinical Immunology estimate that rhinitis affects one in four in the UK.[6]
Typical symptoms of rhinitis include nasal congestion, runny and itchy nose, and sneezing. The eyes, ears, sinuses, and throat can also be involved.
There is no doubt that a seemingly innocuous 'stuffy nose' wreaks havoc on the health of children and adults. Here, we examine the literature to determine whether rhinitis and sleeping with the mouth open is a causal factor for snoring, sleep apnoea and ADHD.
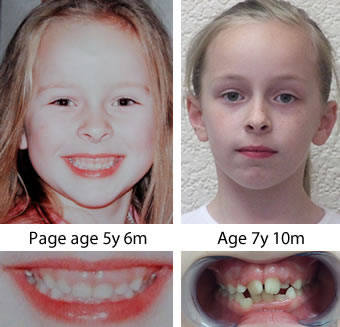
A growing child can develop crooked teeth within a very short time if they change
from habitual nasal breathing to mouth breathing.
The impact of rhinitis and how it negatively affects the quality and quantity of sleep is under recognised and undertreated. "Nasal congestion, which is one of the most bothersome and prevalent symptoms of AR (allergic rhinitis), is thought to be the leading symptom responsible for rhinitis-related sleep problems," including snoring, sleep apnoea and insomnia.[1]
During your school days, you may remember reading about Joe the 'fat boy' from the Pickwick Papers written by Charles Dickens in 1837.
Joe ate in great quantities and was liable to fall asleep during any situation. His breathing was heavy, he snored and he was continuously sleepy. Originally described as the Pickwickian syndrome, his breathing was later labelled as obstructive sleep apnoea syndrome.
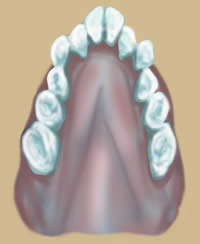
Narrow V shaped top jaw from incorrect tongue posture due to mouth breathing.
There are three types of sleep apnoea: central, obstructive and mixed. Obstructive sleep apnoea is the most common type of apnoea and is characterized by holding the breath from collapse of the upper airways during sleep. This holding of the breath, which prevents airflow to the lungs, may occur between five and fifty times per hour. Each breath hold can range from a few seconds to over one minute, causing one's blood oxygen saturation to decline to as low as 50%. Sleep apnoea is a serious and often undiagnosed condition leading to a wide array of health conditions.
After reviewing texts and articles on Medline, the centre for research disorders in Cincinnati, Ohio concluded that obstructive sleep apnoea, sleep fragmentation, and disturbed sleep often result from nasal obstruction.[10] The authors of the paper observed that "since breathing through the nose appears to be the preferred route during sleep, nasal obstruction frequently leads to nocturnal mouth breathing, snoring, and ultimately to obstructive sleep apnoea."[10] The paper advised that allergic rhinitis and other upper respiratory disorders should be treated more aggressively.[10]
A study by Kim et al which involved 52 patients found that "the more elongated and narrow upper airway during open-mouth breathing may aggravate the collapsibility of the upper airway and, thus, negatively affect OSA severity."[7]
In another study, 385 patients with obstructive sleep apnoea were examined through a questionnaire. Results showed that upper airway symptoms were common, with 61% of patients reporting mouth dryness, 52% with nasal stuffiness, 51% with dryness of the nose, 30% with sneezing, 24% with mucus in the throat, and 17% with a runny nose.[8] Each of these symptoms are characteristic of rhinitis and mouth breathing.
Ohki et al. performed a study to determine the relationship between mouth breathing and nasal obstruction in patients with obstructive sleep apnoea. The study involved 30 normal subjects and 20 patients with snoring or sleep apnoea. Researchers found that chronic nasal obstruction and resultant mouth breathing may induce obstructive sleep apnoea.[9]
Finally, in a paper entitled, "The nose and sleep disordered breathing: what we know and what we don't know," performed an analysis of medical literature on the subject.[11] The analysis confirmed that "SDB (sleep disordered breathing) can both result from and be worsened by nasal obstruction." It was stated that "nasal congestion typically results in a switch to oronasal breathing that compromises the airway." Furthermore, "oral (mouth) breathing in children may lead to the development of facial structural abnormalities associated with SDB." The paper concluded that the change to mouth breathing that occurs with chronic nasal obstruction is a common pathway for sleep-disordered breathing.[11]
Snoring and Sleep Apnoea in Children
It is clear that nasal obstruction with resultant mouth breathing leads to chronic health conditions in adults but does the same apply to children?
Based on an analysis of the medical charts of 248 mouth-breathing children, it was found that 144 (58%) were primary snorers and 104 (42%) had obstructive sleep apnoea syndrome, concluding that "primary snoring and OSAS are frequent findings in mouth breathing children."[12]
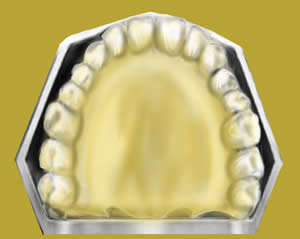
Normal U shaped top jaw which optimally houses all teeth, without overcrowding.
Shaped by the correct resting position of the tongue.
Mouth breathing was also recognized to be a factor in a study to determine the prevalence and association of sleep disorders and school performance. Based on a total of 1,164 completed questionnaires on children aged between 7 and 13 years, it was found that the overall prevalence of snoring was 38.9% with 3.5% habitually snoring. "Allergic symptoms, daytime mouth breathing, shaking the child for apnoea, restless sleep and hyperactivity were significant and independent risk factors and sleep-related symptoms for HS."[13]
The treatment of children with ADHD is commonly with medication or stimulants. An opportune question to ask is whether this is the correct approach given the potential benefits from addressing allergic rhinitis and improving sleep quality?
A Polish study noted that children with sleep respiratory disorders wake up tired, with blocked noses, were breathing through their mouth, tire easily, have concentration problems, are irritated, and demonstrate hyperactivity that may resemble ADHD symptoms. The paper further states that "long-term disease leads to exacerbation of all-systemic symptoms, results in cardiovascular complications, induces developmental inhibition and cognitive dysfunction, and is responsible for school/social failures and reduced life quality."[14]
In a paper entitled A practical approach to allergic rhinitis and sleep disturbance management,[15] Davies et al comments that "sleep quality can be significantly impacted by nasal congestion. This may lead to decreased learning ability, productivity at work or school, and a reduced quality of life."[15]
This is further summed up by Ferguson who states that allergic rhinitis "can lead to impaired nocturnal sleep, and this impairment results in daytime fatigue and somnolence, reducing both learning and work efficiency and decreasing quality of life."[16]
Blaiss in a paper entitled Pediatric allergic rhinitis: physical and mental complications[18] note that allergic rhinitis has a far negative impact on the health of the child than just a simple sneeze. "There are numerous complications that can lead to significant problems both physically and mentally in the child who suffers with allergic rhinitis. Sleep disturbances, poor school performance, and hyperactivity are all mental complications seen in many children related to their nasal allergies."[17]
In a study by Gottlieb et al, parent questionnaires from 3019 children were analyzed to assess the prevalence of sleep disordered breathing symptoms in 5-year-old children and their relation to sleepiness and problem behaviours. Sleep disordered breathing was defined as frequent or loud snoring; trouble breathing or loud, noisy breathing during sleep; or witnessed sleep apnoea.[18] The study found "parent-reported hyperactivity (19%) and inattention (18%) were common, with aggressiveness (12%) and daytime sleepiness (10%) reported somewhat less often. SDB symptoms were present in 744 (25%) children."[18] Authors concluded that "children with sleep disordered breathing symptoms were significantly more likely to have parent-reported daytime sleepiness and problem behaviours, including hyperactivity, inattention, and aggressiveness."[18]
.jpg)
Light forces move teeth, that is why nasal breathing and correct tongue posture is paramount.
"Both allergic rhinitis and attention-deficit/hyperactivity disorder (ADHD) are common paediatric conditions associated with learning difficulties and sleep disturbances."[19] Brawley et al analyzed data from 30 children to determine the prevalence of allergic rhinitis in patients with physician diagnosed ADHD.[19] The paper concluded that "most children with ADHD displayed symptoms and skin prick test results consistent with allergic rhinitis. Nasal obstruction and other symptoms of allergic rhinitis could explain some of the cognitive patterns observed in ADHD, which might result from sleep disturbance known to occur with allergic rhinitis."[19]
Authors of the paper entitled Attention deficit hyperactivity disorder and sleep disorder note that "there is a clear correlation between ADHD and sleep disorders" [20] and "by improving these children's sleep, the symptoms of ADHD are diminished and thus avoid the need to administer psychostimulants, which have undesirable side effects that produce a great deal of anxiety in the parents of these children."[20]
In a paper published in the journal Pediatrics, researchers concluded that "inattention and hyperactivity among general paediatric patients are associated with increased daytime sleepiness and - especially in young boys - snoring and other symptoms of SDB. If sleepiness and SDB do influence daytime behaviour, the current results suggest a major public health impact."[21] "Children undergoing evaluation for ADHD should be systematically assessed for sleep disturbances because treatment of sleep disorders is often associated with improved symptomatology and decreased need for stimulants."[22]
Bearing the documented evidence, having a good night's sleep is imperative to the health of every child and adult. Treating rhinitis is an absolute must in this regard. "Health professionals and school personnel need to increase their awareness of the ramifications of this disease and actively work to prevent deterioration in both academic achievement and workplace productivity."[23]

Self help Buteyko book for children, teenagers and parents
How to Unblock the Nose
The most common reason why the nose is blocked is because breathing volume is too much. The more one breathes through the mouth, the more that the nose will be blocked. When overbreathing takes place, the partial pressure of carbon dioxide in your lungs and blood reduces. This causes a pooling of blood in the nose, increases swelling and creates more mucus.
So, to unblock your nose, do the opposite of big breathing. Hold your breath on the out breath instead. Here is how to do this.
- Take a small breath in through your nose;
- Allow a small breath out through your nose;
- Hold your nose with your fingers to prevent air from entering or escaping;
- Nod your head up and down or sway your body until you feel a very strong need for air;
- Hold your breath for as long as you can but not until you turn blue;
- Let go and breathe in through your nose;
- Calm your breath immediately.
Wait for one minute and repeat. Repeat five or six times until your nose is completely free. And at any time that your nose gets blocked, repeat this again to temporarily decongest your nose. Your nose will be permanently free when your chronic overbreathing is addressed. A free video segment of how to unblock the nose is available at www.youtube.com/watch?v=_UaA_Xz9Ba4
Breathe Better During Sleep
To address snoring and sleep apnoea, and to ensure a deep restful sleep with quieter breathing and better energy upon waking, apply the following solutions;
- No food 2 hours before bed as food increases breathing;
- A cool bedroom is best (but not cold). It is better to have no central heating in a bedroom and to ensure that your duvet or bedclothes are not excessively warm. High temperatures increase breathing. In addition, an airy bedroom is best;
- Don't sleep on your back. Instead sleep on your left hand side or tummy. Sleeping on the back is by far the worst position as there is no restriction to breathing. The left hand side is most preferred position as you breathe less;
- Ensure that your mouth is closed at night.
Ensuring your Mouth is Closed at Night
(free video segment available at www.youtube.com/watch?v=96xUIUA79Ho)
We recommend that adults and older children wear paper tape to gently keep their lips together. Paper tape can be bought at most chemists. A good brand is 3M and a suitable size is one inch. Apply it horizontally to cover your mouth. If you are unable to place it in a horizontal position, then place it vertically. Before applying, fold over a tab at either end of the tape to make removal easier in the morning. Wearing the tape at night is imperative to a good night's sleep and will significantly improve your energy levels upon waking. In fact, all the symptoms listed above will be helped by keeping your mouth closed at night. Taping the mouth is not suitable for children under 5.
If you have drunk copious amounts of alcohol or are feeling nauseas, it is not recommended to wear the tape.
It is possible that some people may, very reasonably, experience a feeling of panic at the very thought of having their mouth taped. To help overcome this, it may be helpful to put the tape on half an hour before going to bed. This should be enough time to become used to the tape and to overcome any nervousness. For the first few nights wearing the tape will feel a little strange. It may come off during the night, but at least you will have spent some hours breathing through your nose.
Continue to wear the tape until you have managed to change to breathing through your nose at night. How long this takes will vary with the individual.
Good Night
References:
1. Storms W. Allergic rhinitis-induced nasal congestion: its impact on sleep quality.
Prim Care Respir J. 17(1):7-18. Mar 2008.
2. Sly RM. Changing prevalence of allergic rhinitis and asthma. Ann Allergy Asthma Immunol. 82(3):233-48; quiz 248-52. Mar 1999.
3. Von Mutius E, Weiland SK, Fritzsch C, et al. Increasing prevalence of hay fever and atopy among children in Leipzig, East Germany. Lancet. 351:862. 1998.
4. Romano-Zelekha O, Graif Y, Garty BZ, Livne I, Green MS, Shohat T. Trends in the prevalence of asthma symptoms and allergic diseases in Israeli adolescents: results from a national survey 2003 and comparison with 1997. J Asthma. 44(5):365-9. Jun 2007.
5. Lima RG, Pastorino AC, Casagrande RR, et al. Prevalence of asthma, rhinitis and eczema in 6 - 7 years old students from the western districts of Sao Paulo City, using the standardized questionnaire of the "International Study of Asthma and Allergies in Childhood" (ISAAC)-phase IIIB. Clinics. 62:225. 2007.
6. www.bsaci.org/index.php?option=com_content&task=view&id=125&Itemid=149
7. Kim EJ, Choi JH, Kim KW, Kim TH, Lee SH, Lee HM, Shin C, Lee KY, Lee SH.
The impacts of open-mouth breathing on upper airway space in obstructive sleep apnea: 3-D MDCT analysis. Eur Arch Otorhinolaryngol. Oct 19 2010.
8. Kreivi HR, Virkkula P, Lehto J, Brander P. Frequency of upper airway symptoms before and during continuous positive airway pressure treatment in patients with obstructive sleep apnea syndrome. Respiration..80(6):488-94. 2010.
9. Ohki M, Usui N, Kanazawa H, Hara I, Kawano K.Relationship between oral breathing and nasal obstruction in patients with obstructive sleep apnea. Acta Otolaryngol Suppl.523:228-30. 1996.
10. Scharf MB, Cohen AP Diagnostic and treatment implications of nasal obstruction in snoring and obstructive sleep apnea. Ann Allergy Asthma Immunol. 81(4):279-87; quiz 287-90. Oct 1998.
11. Rappai M, Collop N, Kemp S, deShazo R. The nose and sleep-disordered breathing: what we know and what we do not know. Chest. 124(6):2309-23. Dec 2003.
12. Izu SC, Itamoto CH, Pradella-Hallinan M, Pizarro GU, Tufik S, Pignatari S, Fujita RR. Obstructive sleep apnea syndrome (OSAS) in mouth breathing children. [Article in English, Portuguese] Braz J Otorhinolaryngol. 76(5):552-6. Oct 2010.
13. Sahin U, Ozturk O, Ozturk M, Songur N, Bircan A, Akkaya A. Habitual snoring in primary school children: prevalence and association with sleep-related disorders and school performance. Med Princ Pract. 2009. 18(6): 458-65. Epub Sep 30 2009.
14. Wasilewska J, Kaczmarski M Obstructive sleep apnea-hypopnea syndrome in children [Article in Polish] Wiad Lek. 63(3):201-12. 2010.
15. Davies MJ, Fisher LH, Chegini S, Craig TJ. A practical approach to allergic rhinitis and sleep disturbance management. Allergy Asthma Proc. 27(3):224-30. May-Jun 2006.
16. Ferguson BJ. Influences of allergic rhinitis on sleep. Otolaryngol Head Neck Surg. 130(5): 617-29. May 2004.
17. Blaiss MS. Pediatric allergic rhinitis: physical and mental complications. Rev Prat. 15; 46(8): 975-9. Apr 1996.
18. Gottlieb DJ, Vezina RM, Chase C, Lesko SM, Heeren TC, Weese-Mayer DE, Auerbach SH, Corwin MJ.Symptoms of sleep-disordered breathing in 5-year-old children are associated with sleepiness and problem behaviors. Pediatrics. 112(4):870-7. Oct 2003.
19. Brawley A, Silverman B, Kearney S, Guanzon D, Owens M, Bennett H, Schneider A. Allergic rhinitis in children with attention-deficit/hyperactivity disorder.
Ann Allergy Asthma Immunol Jun;92(6):663-7. 2004.
20. Betancourt-Fursow de Jiménez YM, Jiménez-León JC, Jiménez-Betancourt CS. [Attention deficit hyperactivity disorder and sleep disorders].[Article in Spanish]
Rev Neurol. Feb 13;42 Suppl 2:S37-51. 2006.
21. Chervin RD, Archbold KH, Dillon JE, Panahi P, Pituch KJ, Dahl RE, Guilleminault C. Inattention, hyperactivity, and symptoms of sleep-disordered breathing. Pediatrics. Mar;109(3):449-56. 2002 .
22. Domínguez-Ortega L, de Vicente-Colomina A [Attention deficit-hyperactivity disorder and sleep disorders].[Article in Spanish] Med Clin (Barc). Apr 8;126(13):500-6. 2006.
Comments:
-
No Article Comments available