Positive Health Online
Your Country

Malocclusions Linked to Abnormal Foot Motion
by Brian A Rothbart PhD(more info)
listed in bodywork, originally published in issue 151 - October 2008
This paper discusses the impact abnormal foot motion can have on the cranial bones and occlusion. Section I describes this foot-cranial-dental coupling. Section II describes the Ascending Foot Cranial Model. Section III describes an embryonic foot type that is frequently responsible for cranial imbalances and malocclusions. And Section IV describes a Proprioceptive Therapy using Proprioceptive Insoles that can reverse (in children) or stabilize (in adults) cranial imbalances and malocclusions.
Intuitively, we know that the body’s framework functions as a unit: instability in one area of the body can reverberate throughout the entire body. This understanding underpins the concept that cranial imbalances and malocclusions can be the result of abnormal motion within the feet. While many scientists accept the plausibility of this correlation, little or no clinical research has been published that supports this foot-cranial-dental linkage until recently.
Over the past several years, I have collected clinical data that statistically suggests cranial imbalances and malocclusions are linked to abnormal foot motion. These findings are presented below, and hopefully will prove useful in treating malocclusions and cranial imbalances.
Section I: Foot-Cranial-Dental Coupling
One of my recent published statistical studies suggests that abnormal foot motion can result in facial distortions. Specifically, asymmetrical abnormal pronation, where the feet are rotated inward, forward and downward (See Fig. 1), can result in an asymmetrical loss of Vertical Facial dimension (VFd), the distance between the outer orbit of the eye (exocanthion) and outer margin of the ipsilateral lip. Two facial distortion patterns have been identified relative to the asymmetrical pronation patterns in the feet.[1]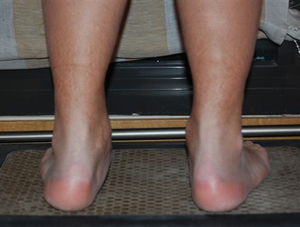
Figure 1. Abnormal Pronation Left Greater than Right
- Left Foot More Pronated than Right Foot: vertical distance between the left eye and ipsilateral lip is shorter, relative to the distance between the right eye and lip (referred to as the Vertical Facial dimension [VFd]) (See Fig. 2). This is frequently associated with a Class II malocclusion (overbite) and narrowing of the dental arch.

Figure 2
In both cases, a torsional (twisting) strain develops in the facial bones (side to side and front to back). This can lead to a plethora of symptoms, including TMJ dysfunction and/or headaches.
- Right Foot More Pronated than Left Foot: vertical distance between the right eye and ipsilateral lip is shorter, relative to the distance between the left eye and lip. This is frequently associated with a Class II malocclusion (overbite) and narrowing of the dental arch.
Section II: Ascending Foot Cranial Model
The science studying how the foot moves when walking is termed foot biomechanics.
- Normal Pronation: Foot is pronating when the ipsilateral (same side) hip is internally rotating. This hip to foot coupling is referred to as Hip Drive (See Fig. 3);
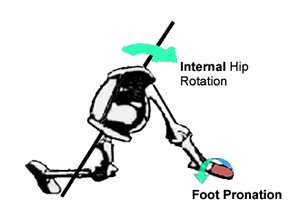
Figure 3. Hip Drive
- Abnormal Pronation: foot is pronating when the ipsilateral hip is externally rotating, I have theorized an Ascending Foot Cranial Model to explain the observed coupling affect between the feet, cranium and occlusion (See Fig. 4);
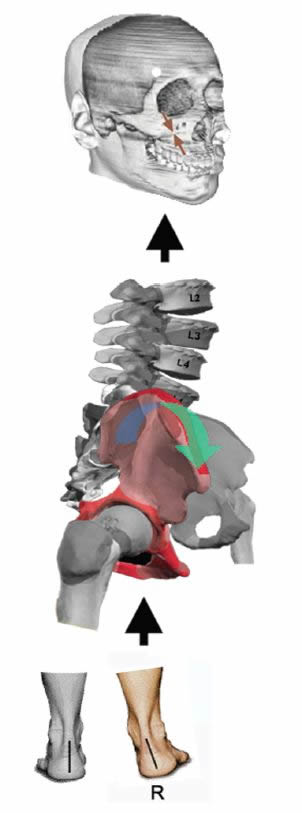
Figure 4. Ascending Foot – Cranial Model
- Abnormal Foot Pronation (inward, forward and downward) forces the innominates (hip bones) to rotate anteriorly (forward) and the downward (ASIS), the more anteriorly rotated hip being ipsilateral to the more pronated foot;[2]
- Anterior Rotation of the Hip Bones draw the temporal bones into an anterior (internal) rotation, the more anteriorly rotated temporal bone being ipsilateral to the more anteriorly rotated hip bone;
- Anterior Rotation of the Temporal Bones extends the sphenoid and cants both the sphenoid and maxilla:
– If the right temporal bone is more anterior rotated (tip of right mastoid more cephalad, less prominent), the sphenoid bone is forced into a left torsional pattern (canted downward to the right) and the right maxilla is canted superiorly;
– If the left temporal bone is more anterior rotated, the sphenoid bone is forced into a right torsional pattern (canted downward to the left) and the left maxilla is canted superiorly;- The resulting cants in the sphenoid and maxilla bones result in asymmetrical Vertical Facial dimensions, the shorter VFd being on the same side as the more pronated foot;[3]
- Extension of the sphenoid bone narrows the dental arch and crowds the teeth. The curve of Spee deepens. (See Fig. 5).
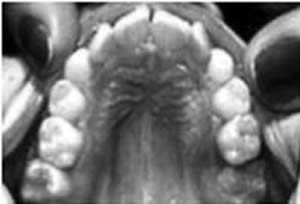
Figure 5. Curve of Spee
Dental Orthogonal Radiographic Analysis (DORA) supports the above proposed Ascending Foot Cranial Model and the observed facial distortions resulting from this model. This radiographic technique was first introduced by Gerald Smith, DDS, to visualize cranial lesions resulting from occlusal lesions. Later, I adapted DORA, correlating (linking) the distortional patterns in the cranial bones to the loss of Vertical Facial dimensions.
Figure 6 is a DORA of a patient with an abnormal pronation pattern left > right.
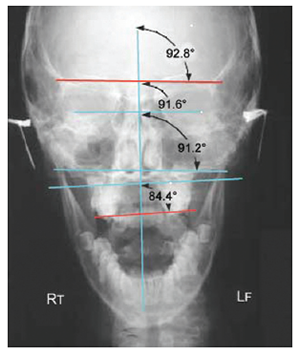
Figure 6. DORA Dental orthogonal radiographic analysis visualizing a cranial imbalance. An inferior cant of the sphenoid (cephalad red sphenoid line) concurrent with a superior cant of the maxilla (caudal red malar line) can result in a relative loss of vertical facial dimension. This author suggests that the cant in the sphenoid and maxilla bones results from an anterior (internal) rotation of the temporal bone. The petrous acts as the axis of rotation of the temporal bone. As a point of reference, internal rotation of the temporal bone is defined as a relative medial, anterior displacement of its squama. The sphenoid line is the horizontal line through which the two lowest points on the inferior border of the malar bone. (Reprinted with permission from Smith[8])
The following lines are drawn:
The following changes are observed on the DORA:
- VRL (Vertical Reference Line): a vertical line drawn through the centre of the nasion and the anterior nasal line;
- LWSL (Lesser Wing of Sphenoid): a line connecting the height of the convexity of the right and left portions of the lesser wings of the sphenoids;
- ATL (Apex of the Temporal Bones): a line connecting the tips of the right and left malar (zygomatic) bones;
- Malar Line is the horizontal line through the two lowest points on the interior border of the malar bone;
- LWS Line is canted downward left, suggesting a right torsional pattern;
- AT Line is canted cephalad right, suggesting a more anteriorly rotated left temporal bone);
- ML line is canted cephalad left, suggesting a left cephalad cant of the maxilla (a maxilla that is shifted upwards on the left side of the face).
Section III: Etiology of Abnormal Foot Pronation
The author discovered an embryological foot type in which the first metatarsal is elevated and inverted relative to the second metatarsal, referred to as a Primus Metatarsus Supinatus (PMS) foot structure.[4,5] This foot structure is the result of an incomplete unwinding of the talus (a tarsal bone sitting on top of the heel bone). Clinically, this places the first metatarsal and hallux (big toe) off the ground, when the foot is placed in its anatomical neutral position. (See Fig. 7) In order for the 1st metatarsal and hallux to reach the ground, when walking or standing, the foot must roll inward and downward, e.g. abnormally pronate.[6] It is this abnormal pronation that can result in loss of VFd.
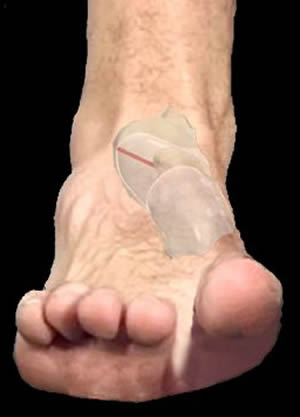
Figure 7. PMs Foot Structure Resulting From Talar Supinatus
Section IV: Proprioceptive Therapy Using Proprioceptive Insoles
Proprioceptive Therapy is the process of using Proprioceptive Insoles to reverse the postural distortions, and eliminate the associated pain resulting from the Primus Metatarsus Supinatus foot structure. Computerized postural and video analysis is run to determine the correct strength of signal (prescription) to use in the Proprioceptive Insoles. If the wrong prescription is used, it can exacerbate the pain.The Rothbart Proprioceptive insoles are non-supportive type foot insoles which apply a tactile stimulation to the bottom of the foot (See Fig. 8). In theory, this tactile stimulation transmits a signal to the brain (cerebellum). Acting on this signal, the cerebellum initiates a positional correction affecting the entire body posture, including the cranial bones. The torsional rotations within the temporal bones and sphenoid are reversed. Frequently this improvement in position reduces or eliminates many of the symptoms associated with cranial imbalances (headaches) and malocclusions (TMJ).

Figure 8 (Inset). Rothbart Proprioceptive Insole
Proprioceptive insoles can prevent malocclusions from developing in young children. However, if a malocclusion has developed, orthodontic therapy should be considered (e.g. the Advanced Lightwire Functional appliance) to improve the functional alignment of the cranial bones and teeth.
Proprioceptive insoles are used to realign the head over the cervical spine. This must be done before orthodontic intervention is initiated. Otherwise, orthodontic intervention can lock the head in a forward position that will prove intractable to correction. A forward head position can result in headaches, neck and shoulder tension and pelvic instability.
References
1. Rothbart BA. Vertical Dimensions Linked to Abnormal Foot Motion. Jour Amer Podiatr Med Assoc. 98(3): 189-195. 2008.2. Rothbart BA. Relationship of Functional Leg-Length Discrepancy to Abnormal Pronation. Journal American Podiatric Medical Association. 96(6): 499-504. 2006.
3. Rothbart BA. Vertical Facial Dimensions Linked to Abnormal Foot Motion. Journal American Podiatric Medical Association. 98(3): 189-195. 2008.
4. Rothbart BA. Medial Column Foot Systems: An Innovative Tool for Improving Posture. Journal Bodywork and Movement Therapies. 6(1): 37-46. 2002.
5. Proprioceptive Stimulation – The Primus Metatarsus Supinatus Foot Structure. Available Online at http://www.rothbartsfoot.info/RFS.html
6. Proprioceptive Stimulation - Abnormal Pronation, Gait Animation. Available Online at
http://www.rothbartsfoot.info/TreadmillAnalysis.html
Further Information
For more information regarding the Primus Metatarsus Supinatus foot structure and Proprioceptive Therapy, visit: www.rothbartsite.com
Comments:
-
No Article Comments available