Positive Health Online
Your Country

Effective Antimicrobial Essential Oils for Protection against Dangerous Infection
by Maggie Tisserand(more info)
listed in infections and inflammation, originally published in issue 196 - July 2012
The Rise of MRSA
MRSA is an acronym for methicillin-resistant Staphylococcus aureus, and refers to strains of this bacterium that are resistant to the antibiotic methicillin, and to other classes of antibiotics. MRSA is often referred to in the press as a ‘superbug’, meaning a bacterium resistant to several antibiotics. MRSA infections are classified as either healthcare-associated MRSA (HA-MRSA) or community-associated MRSA (CA-MRSA), although this distinction is more complicated than simply where the infection was caught. MRSA was first reported in the United Kingdom in 1961, and in the United States in 1968. A combination of its virulence, ease of transmission and antibiotic resistance has resulted in MRSA becoming a major problem in the health care setting and in the community.

The world we live in is full of bacteria, the vast majority of which are harmless, although some are more dangerous than others. MRSA is perhaps the most dangerous of infectious diseases, not because it is a ‘rare beast’ but precisely the opposite - because it is commonplace. Staphylococcus aureus is known as a commensal of humans i.e. it comprises part of the body’s normal bacterial flora, but without causing disease. Staphylococci frequently live on the skin, especially in folds such as the armpit and groin, in the nose and less commonly in the throat. MRSA strains give rise to the same diseases and conditions as those caused by antibiotic-sensitive strains, and are usually no more aggressive or infectious; they are only more serious than other Staph. aureus infections because they do not respond to antibiotic treatment. The World Health Organization published a report in 1982, warning that the spread of antibiotic resistant bacteria in hospitals would make the choice of antibiotic “a gamble of worsening odds”. Following this report, WHO initiated a survey of hospitals in fourteen countries which concluded that “hospital infection is a common and serious problem throughout the world”.
MRSA is an international problem that affects the health of young and old alike. It can be picked up in the community as well as in hospitals and nursing homes. It is affecting the health of both domestic and agricultural animals. It has become adept at surviving long journeys. It can lie dormant on clothing and commercial items. It can be carried in the nostrils and on the bodies of healthy individuals. Researchers tracking the spread of MRSA say that the disease is distributed by the movement of people and goods around the world. In North America the number of MRSA deaths outnumber those from AIDS by a factor of five, yet current funding for MRSA research is a tiny fraction of the funding available for HIV/AIDS.
Antimicrobial Essential Oils to use for Prevention / Treatment
Tea tree
Thyme linalool or Benchmark thyme
Manuka
Lavender
Geranium
Antimicrobial Essential Oils for Airborne Use
Cinnamon
Orange
Lemon
Lemongrass
Grapefruit
It is important to have an understanding of essential oils and how to use them and I recommend the reader purchase one of the many excellent books on the subject of aromatherapy. Many of the above oils are detailed in Aromatherapy vs MRSA.
Essential Oils Clinical History against Infections
Essential oils have a long history of use in combating infection and many are marketed for their antiseptic properties. Science is now backing up these claims and an internet search for “antimicrobial research with essential oils” will bring up hundreds of research papers. Scientific research is ongoing; as recently as November 2010, an international conference on antimicrobial research took place in Spain. One session, entitled: “Antimicrobial natural products”, covered a wide range of natural substances that included essential oils and aromatic plants. Essential oils are nature’s antiseptics and their ability to kill microorganisms has been well documented over the centuries. Hippocrates, the founder of medicine, used aromatic plants as early as 500BC. Essential oils are most commonly extracted from plants of a single botanical source by steam distillation and are known to be a complex mixture of organic hydrocarbons. Chemical analysis of essential oils allows them to be classified depending upon the nature and ratio of components in the oil and this significant difference in chemical composition is what gives each of them their unique properties.
The scientific testing of essential oils against micro-organisms has been taking place for decades, with the majority of the work seeking out effective preservatives for the food industry. As food poisoning can cause fatalities whenever there is an outbreak, a vast amount of research has been undertaken with food grade essential oils such as thyme, peppermint, lemon, cinnamon, clove and oregano. Some essential oils with significant antimicrobial credentials, such as eucalyptus oil, are too highly scented to be used as a food preservative and have instead been utilized in toothpastes, mouth washes, cough drops, pastilles and decongestants. Thyme oil has been used as a fumigant in sick rooms and places of worship by many ancient civilizations. As far back as 1887, thyme was recognized as having antibacterial properties, although it wasn’t until the 1980s that it became the subject of scientific interest. The majority of microbiology research into thyme’s ability to kill bacteria has been published in food journals. Thyme oil is also much respected for its antibacterial triumph against gum disease.
Canadian researchers evaluated twenty-eight essential oils for their antibacterial properties against four bacteria prevalent in the food industry. Staphylococcus aureus was one of the four. Of the essential oils tested, the most effective were the thyme oils, having significant levels of the aroma-chemicals thymol and carvacrol. These two plant constituents were found to be the most potent against the four main bacterial pathogens responsible for outbreaks of food poisoning. In Canada alone, the cost of treating food borne disease due to contamination with bacteria is estimated to be $500 million a year.
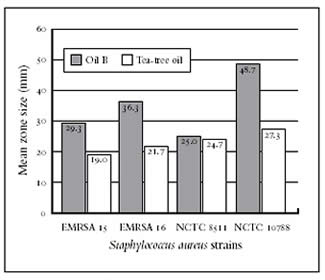
Fig 1 Bar Chart Comparing Tea Tree to Oil B
Microbiology Testing of Essential Oils as an Alternative to Antibiotics
For decades, research institutions from around the world have been taking a serious look at essential oils as potential alternatives to antibiotics, with tea tree oil being the most researched essential oil by far. The antimicrobial activity of an essential oil is determined in the laboratory (in vitro) by a number of standard methods. One of the commonest methods employed in the laboratory is the Zone of Inhibition test. This is a very quick and easy method where a standard number of microorganisms (about 1 million bacterial cells per millilitre) are applied to the surface of an agar plate, which allows bacteria to grow. A measured amount of essential oil is added either to a paper disk or to a ‘well’ bored into the agar. The components in the oil will diffuse into the culture medium and a circular zone will be visible if there is any antimicrobial activity. Tea tree oil, as an example, disrupts the cell membrane of the bacterium, causing a loss of potassium ions from the cell. The lipophilic (lipid loving) monoterpenes integrate with the phospholipids in the membrane and leakage occurs. Antimicrobial essential oils have also been known to cause inhibition of glucose dependant respiration in S. aureus, E. coli and C. albicans. As well as effective trials with the essential oils when putting them in direct contact with bacteria, the vapours released from essential oils have also been proven to be highly antimicrobial. A recent study has shown that MRSA and Clostridium difficile have been killed in the laboratory by a blend of vapours released from a variety of dispersion devices. The most efficient system is the use of ‘venturi technology’ where air is forced over the surface of essential oil blends causing the antimicrobial vapours to be released into the atmosphere, killing bacteria in the air as well as on surfaces. This method of using essential oils opens up an exciting possibility for reducing the spread of airborne healthcare associated infections.
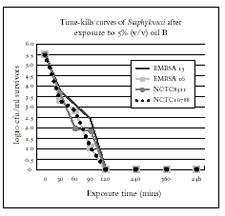
Fig 2 Time-kill Curves for Oil B thyme blend
Microbiology research in 2001 looked at the antibacterial effect of a blend of Australian tea tree and New Zealand manuka essential oils. When the blend had more manuka than tea tree, the mixture was more effective against Gram-positive organisms such as Staph aureus. Conversely, when the mixture had a higher proportion of tea tree to manuka, the mixture was more effective against Gram-negative organisms such as E. coli.
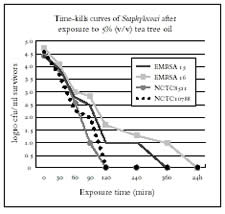
Fig 3 Time-kill Curves for Tea Tree
Blending essential oils together has been found to create powerful and effective mixtures of aroma-chemistry. In 1998, a patent was filed for a natural broad-spectrum antibiotic. It consisted of a combination of tea tree and thyme oils. The specific thymes used in this research were white thyme (rectified Thymus vulgaris) and wild thyme, (Thymus serpyllum). Staphylococcus aureus was the organism tested, not MRSA. The patent was later withdrawn.
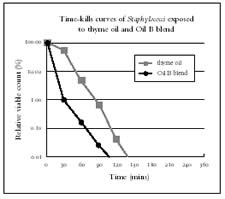
Fig 4 Time-kill curves for all staphylocci exposed to thyme oil and Oil B blend
Essential Oils in Clinical Trials
Some clinical research in 2003 set out to compare tea tree oil with the standard topical antibiotic mupirocin. The purpose of the trial was to compare two methods of eliminating MRSA - from the nose, where it can be carried by hospital patients who could then infect themselves, and from body sites where MRSA bacteria can be harboured. The standard treatment was a 2% mupirocin nasal cream used in conjunction with a triclosan body wash. The tea tree regimen used a 4% tea tree oil ointment for use in the nose plus a body wash with 5% tea tree oil. At the end of the trial period the researchers concluded: “the tea tree oil products appeared to work as well as the standard hospital treatments”.
In 2004 another clinical trial was carried out in the UK. The randomized control trial compared the efficacy of tea tree preparations to a standard hospital regimen for the eradication of MRSA colonisation. The standard regimen comprised the topical antibiotic mupirocin in a 2% dilution for nasal treatment, along with chlorhexidine and a silver infiltrated cream for cleansing colonised body sites. The tea tree regimen consisted of a 10% tea tree cream and 5% tea tree body wash. One hundred people were involved in the five-day trial with the standard regimen, and by the end 49% were cleared. A similar number of people were treated with the tea tree products and 47% were cleared. The trial conclusion was that whilst the topical antibiotic was more effective at clearing nasal carriage of MRSA, the tea tree products worked better at clearing the colonised body sites.
In 2005, I began working with scientists at the University of Brighton to try to find effective essential oils or a blend of essential oils that would offer an alternative to the much-tested tea tree oil. It had to be safe to use on the skin whilst being powerful enough to kill epidemic strains EMRSA-15 and EMRSA-16. Common thyme oil was not included in tests, as its skin irritant factor is well known, but I did include a sub species of thyme which produced good results against both epidemic strains as well as two strains of MSSA (methicillin sensitive Staphylococcus aureus). Over a period of months several different species of thyme were investigated, culminating in an optimum blend of four individual thyme species. Tea tree oil was also investigated and a comparison of the results was made. Both the tea tree and the thyme blend (named Benchmark thyme) were effective in killing the MRSA and the MSSA.
There is no shortage of academic evidence to show that essential oils and their individual components are antimicrobial, but having access to the research is just the first step on a long flight of stairs. Unfortunately, each ascending step has onerous costs and difficulties, mainly with the setting up of clinical trials and the gaining of regulatory approval that only large, financially strong companies can consider undertaking. Another hurdle is that because of the vast financial investment needed to bring a medicinal product to market, even large pharmaceutical companies need to be able to secure a patent in order for them to retain exclusive marketing of the product and recoup their investment before the patent expires. So, for the time being, there are no licensed products, based on essential oils, to combat MRSA.
Bibliography and Acknowledgements
The article is a compilation of passages taken from Aromatherapy vs MRSA by Maggie Tisserand. Published by The Clarity Press, 2012. www.theclaritypress.co.uk
Special acknowledgements must go to contributors to the book - Dr Jonathan Caplin of the University of Brighton for contributing Chapter 4 and to Professor Val Edwards-Jones, Manchester Metropolitan University for contributing Chapter 5.
Further Information
Aromatherapy vs MRSA is available from www.singingdragon.com , Amazon and other online retailers, and all good bookshops.
www.amazon.co.uk/Aromatherapy-MRSA-Antimicrobial-Essential-Bacterial/dp/1848192371
www.amazon.com/Aromatherapy-MRSA-Antimicrobial-Essential-Bacterial/dp/1848192371
www.jkp.com/catalogue/book/9781848192379
Comments:
-
Andrew Cutler D.B.Th; MCMA said..
As a Registered Medical herbalist for over twenty years I am delighted to read this article. However I wrote many years ago to the then head of infection control for the Dorset hospitals group outlining research into trials that had taken place using dilutions of tea tree oil down to as low as 1%. Over 29 different pathogens were killed including MRSA. My letter at the time suggested trialling a 'mist' system to be used in hospitals as a means of infection control. Needless to say I was never acknowledged and heard nothing from the Doctor to whom I had written. Glad at last there is some more progress!