Positive Health Online
Your Country

Lichen Planus: A Disease Profile
listed in skincare, originally published in issue 184 - July 2011
Introduction
Lichen Planus (LP) is a relatively uncommon, inflammatory papulosquamous disorder of unknown aetiology; The response may be provoked by a viral infection, and some studies, have associated the condition with chronic hepatitis C.[1] LP may also be provoked by a drug or after a stressful event; further studies have linked LP also to dyslipidaemia.[2] LP may affect the skin, nails, hair and mucous membranes.
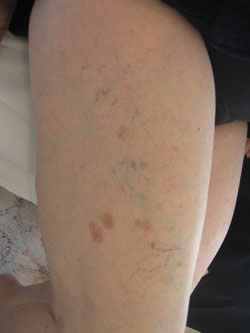
Lichen Planus - C Louch 2011
Pathogenesis
The relationship between hepatitis C virus (HCV) infection and oral lichen planus (OLP) remains a matter of controversy. HCV is a single-stranded, positive-sense RNA virus. It is a blood borne pathogen. After acute HCV infection, the proportion of patients who may remain chronically infected is estimated to be as high as 85% to 90. However, and as the aetiology itself of LP is currently unknown, at present, there is not enough information to determine if HCV genotype plays a role in development of OLP.[3] As further case control studies have associated LP with dyslipidaemia, viral infections, stress and possible drug reactions, practitioners taking care of patients with LP should be aware of the possible associations.[4]
LP is rare in children under the age of 5 years and more common in middle aged women. Ten per cent of patients do have a positive family history. The disease progression is variable and unpredictable in all subtypes; LP lesions are intermittent pruritic, and may occur abruptly as a generalised disease; LP can occur also secondary to drug intake. Severe oral LP may degenerate to squamous cell carcinoma in 3% of cases.[5]
The primary lesion is a 2 to 10mm flat-topped papule with an irregular, angulated border, named a polygonal papule. New lesions are pink to white, and over time become purple and sharply defined. The skin surface shows lacy reticulated patterns of whitish lines, called Wickham's striae. New lesions may develop in areas of an injury, called Koebner phenomenon.[6] The histological features of the disease are marked liquefaction of the basal layer, expansion of the granular cell layer and dense sub-epidermal infiltrate, predominantly of T-lymphocytes. Patients may present with disease limited to one or two areas of the skin, and it is quite uncommon that the presentation may be extensive affecting both skin and mucous membranes. It is common for mucous membranes to be affected without any symptoms on the skin. In around 10% of patients there are nail changes.
Symptoms
Symptoms related to the skin lesions vary from nothing to severe pruritus. Scaling of the skin may also be associated with LP and it tends to be the thicker and scalier areas, which are most pruritic. Hyperpigmentation may occur where the lesions have been and this seems to be more common in darker skin colours. On the mucous membranes lesions can be accompanied with a stinging sensation; they may become painful if the lesions deteriorate and become erosive.
Nail changes in LP occur because of nail plate thinning, which results in longitudinal grooving and ridges. Further nail changes may include subungual hyperkeratosis, onycholysis and longitudinal melanonychia. Very rarely the nails may appear altogether.
There are various subtypes of lesion planus:
Types of LP
Papular LP
This is the most common form of LP; the papules are located on the flexor surfaces of the wrists and forearms, the ankles and the lumbar region.[7]
Hypertrophic LP
Lesions which persist become thicker and the colour changes to dark red. These are commonly found on the shins and tend to aggregate into different patterns. Vesicles and bullae may appear. A persistent brown staining develops after the lesions resolve.[8]
Follicular LP
The lesions are follicle-based papules found on the scalp and permanent hair loss with marked scarring may occur (scarring alopecia).[6]
Mucosal LP
The most common form is the non-erosive form with a white lacy pattern. The erosive form is painful with beefy desquamation. Oral lesions affect primarily the buccal mucosa and lateral edge of the tongue. This may affect the mucosal lip, but rarely extends beyond the vermilion border. Genitals may be involved, with intense pruritus and commonly a burning sensation, marked mucosal fragility and erythema. Secondary candidiasis occurs frequently, as a likely side-effect of allopathic topical medication.[5]
Nail Involvement:
Nails may present changes in the absence of skin findings, which are usually proximal to the distal linear depressions in the nail plate. Inflammation of the matrix may result in adhesion of the proximal nail fold to the scarred matrix to form a ptergium (scar).[9]
Laboratory Findings
Laboratory findings, involving a skin biopsy, show an accumulation of mononuclear cells obscuring the dermoepidermal interface, and a T cell-mediated cytotoxic reaction against the basal layer keratinocytes. Routine immunofluorescence biopsy of scalp skin helps ruling out lupus. Antibodies to hepatitis C virus are detected in about 16% of patients with cutaneous lichen planus and about 30% of patients with mucosal involvement.[4]
Differential Diagnosis
The papular form of LP may be confused with psoriasis and popular eczema although the epidermal changes are quite different. Hypertrophic LP can be distinguished from psoriasis, stasis dermatitis and lichen simplex chronicus, through verrucous changes. Scarring alopecia is differentiated from discoid lupus through biopsy and immunofluorescence. Mucosal non-erosive lesions can resemble leukoplakia or candidiasis and genital lesions may also be difficult to distinguish from psoriasis papules. Erosive lesions may in some cases confused with pemphigus vulgaris, paraneoplastic pemphigus and fixed drug eruption.[5]
Allopathic Treatment of LP
Sedating antihistamines are usually prescribed for pruritus, together with Group I or II topical steroids twice daily as initial topical treatment for localised disease. Hypertrophic lesions are treated with intralesional triamcinolone acetonide. Prednisolone is usually prescribed for generalized skin or erosive mucosal involvement and corticosteroids for initial treatment for oral lesions, to be applied topically. Inhaled corticosteroids are also prescribed as alternatives to cream Orabase preparations and sprayed directly on lesions. Retinoids are reserved for severe forms of recalcitrant LP and Tacrolimus for erosive oral lesions.[5]
Phytomedical Treatment of LP
Phytomedical treatment of LP focuses on the possible underlying cause of the condition. The first step to ensure a successful outcome of the treatment is to refer the patient for a full biochemistry and haematology profile, and if necessary, hepatitis screen. In case of dyslipidaemia, systemic treatment may focus on reducing the patient's low density lipoprotein (LDL) and triglycerides for example. A typical systemic phytomedical approach would involve the following extracts dispensed as 1:2 or 1:1 tincture formulation: Trigonella foenum-graecum, Cynara scolymus, Gymnema sylvestre, Chionanthus virginica.[10]

Chionanthus virginica - C Louch 2011
In case the patient suffers from liver dysfunction, the following systemic phytomedical extracts would be dispensed: Glycorrhiza glabra, Bupleurum falcatum, Scutellaria baicalensis, Silybum marianum, Schizandra chinensis, Taraxacum radix, Astragalus membranaceus. In case of a viral liver condition such as hepatitis C, phytomedical antivirals such as Hypericum perforatum for example would be added to the prescription.[10]

Scutellaria baicalensis - C Louch 2011
Phytomedical treatment of LP lesions would typically involve a soap free wash cream based on Aloe vera extract. Hot water is to be avoided as it tends to dehydrate the epidermis, thus exacerbating pruritic skin conditions such as LP. An external phytomedical ointment to be used on damp skin twice a day would consist of infused oils of Calendula officinalis, Stellaria media, Borago officinalis, Symphytum officinale. A topical lesion cream to be applied on the LP lesions two to 3 times a day would typically be composed of phytomedical extracts of Calendula officinalis, Stellaria media, Matricaria recutita.[10]

Borago officinalis - C Louch 2011
Treatment Outcome
In general, phytomedical treatment is very effective in clearing LP lesions within 12 to 18 months. However, LP may persist longer in a small number of people who are severely affected. This is mostly in people who develop LP mouth ulcers, and LP of the vulva or penis. Once the rash has cleared, about one in five affected patients may have a recurrence sometime in the future. A small number of people have several recurrences, depending on their underlying condition. In case of nails or hair involvement, bald patches or damaged nails may be permanent.
Patient with LP have a slightly higher than average chance of developing other inflammatory diseases. For example: ulcerative colitis, alopecia areata, vitiligo, dermatomyositis, morphea, lichen sclerosis, and myasthenia gravis. In case of ulcer development in the mouth due to LP, there may be a higher chance of developing mouth cancer. Regular mouth checks from a dentist are advisable.[11] If the vulva is severely affected, there is a slight increased risk of developing cancer of the vulva.[12]
References
1. S Birkenfeld, J Dreiher, D Weitzman and AD Cohen. A study on the association with hepatitis B and hepatitis C in 1557 patients with lichen planus. Journal of the European Academy of Dermatology and Venereology 25 (4): 436-440. April 2011.
2. Nita Chainani-Wu, Francina Lozada-Nur, Norah Terrault. Hepatitis C virus and lichen planus: A review. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology, Volume 98, Issue 2, Pages 171-183. August 2004.
3. Jean-Michel Pawlotsky, Mustapha Ben Yahia, Chantal Andre, Marie-Catherine Voisin, Liliane Intrator, Françoise Roudot-Thoraval, Lionel Deforges, Christophe Duvoux, Elie-Serge Zafrani, Jean Duval and Daniel Dhumeaux. Immunological disorders in C virus chronic active hepatitis: A prospective case-control study. Hepatology 19 (4): 841-848. April 1994.
4. SM Breathnach and MM Black. Lichen Planus and Lichenoid Disorders. Rook's Textbook of Dermatology, Seventh Edition Pages: 2089-2120. 2008
5. Bethanee J. Schlosser. Lichen planus and lichenoid reactions of the oral mucosa. Dermatologic Therapy 23 (3), Pages: 251-267. May/June 2010.
6. Gillian Marshman. Lichen planus. Australasian Journal of Dermatology 39(1): 1-13. February 1998.
7. Christian Kunte, Istrid Erlenkeuser-Uebelhoer, Silke Michelsen, Karla Scheerer-Dhungel and Gerd Plewig. Behandlung des therapieresistenten erosiven, oralen Lichen ruber mit extrakorporaler Photopherese (ECP) JDDG: Journal der Deutschen Dermatologischen Gesellschaft 3 (11): 889-894. November 2005.
8. Hashem B. El-Serag, Howard Hampel, Christine Yeh and Linda Rabeneck. Extrahepatic manifestations of hepatitis C among United States male veterans. Hepatology 36 (6): 1439-1445. December 2002.
9. DAR de Berker, R Baran and RPR Dawber. The Nail in Dermatological Diseases.
Baran and Dawber's Diseases of the Nails and their Management, Third Edition: 172-222. 2008.
10. Louch C. Lichen Planus: A Disease Profile. Positive Health PH Online Issue 184 July 2011. www.positivehealth.com/article/skincare/lichen-planus-a-disease-profile
11. C Scully and M El-Kom. Lichen planus: review and update on pathogenesis. Journal of Oral Pathology & Medicine. 14 (6): 431-458. July 1985.
12. CB Bunker and SM Neill. The Genital, Perianal and Umbilical Regions. Rook's Textbook of Dermatology, Seventh Edition: 3535-3638. 2008.
Comments:
-
herbssolutionsbynature said..
The treatment is option in such cases but the intense itching needs to be treated. Several Lichen Planus Treatment are available. This includes steroid creams, pasts and tablets, immune suppressant medications, PUVA, antihistamenics and emollients but all these have several side effects. Lichreton an herbal product by Herbs Solutions By Nature is made of totally natural herbs and so is completely free of any kind of side effects.