Positive Health Online
Your Country

Shin Splints/Compartment Syndrome
listed in osteopathy, originally published in issue 194 - May 2012
Shin splints (Runners leg) is not a specific diagnosis; it is merely a descriptive term, no more specific than headache or chest pain.[Pecina and Bojanic 2005, Pg 255]
The evidence seems clear that shin splint pain has many different causes and reflects the variation in anatomy.[Pecina and Bojanic 2003 Pg 255]
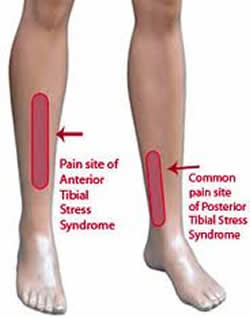
The most common causes of shin splints are:
- Tibialis Posterior Syndrome;
- Periostitis of the Tibia (Medial Tibial Stress Syndrome);
- Chronic (exertional) compartment syndrome;
- Stress Fracture of the Tibia.
Garrick and Webb [1990], state even the most sophisticated current diagnostic tools have not been able to positively identify the causes of ‘shin splints’.
The principle symptom of runner's leg is pain, whatever the aetiology. In the early stages pain appears exclusively after running; in the latter stages tenderness and pain are present at the beginning, during and after running (activity) and during normal everyday activity.

Tibialis Posterior Syndrome
Most anterior (deepest) muscle of deep posterior (plantar flexor) compartment of leg; origin, soleal line and posterior surface of tibia, the head and shaft of the fibula between the medial crest and interosseous border, and the posterior surface of interosseous membrane; insertion, navicular, three cuneiform, cuboid, and second, third, and fourth metatarsal bones; action, plantar flexion and inversion of foot; nerve supply, tibial.
Look up the full anatomy of this muscle. Important for maintaining stability of the foot.
With a pronated foot and lowered arch, overuse of the muscle, e.g., during running appears. This excessive pressure leads to a ‘separation’ of the muscle fibres at the origin of the muscle in the posterior aspect of the tibia (Partial ruptures). This process is gradual and, therefore, the symptoms appear gradually.[Pecina and Bojanic 2003 pg 257]
Tenderness felt along the medial border of the leg, behind the medial edge of the tibia in the middle and distal thirds of the leg is characteristic for this syndrome.[Pecina and Bojanic 2003 pg 257]
Diagnosis confirmed by palpation. Slip a finger behind the medial edge of the tibia and move from proximal to distal. Pain will be reproduced in the middle and distal thirds of the tibia 8-12cm in length, (Pecina and Bojanic 2003 pg 257).
Periostitis of the Tibia
The term should be used to describe periosteal changes of the anteromedial plane of the tibia, in an area approximately 10cm above the ankle, and 5-10cm in length.[(Pecina and Bojanic 2003 pg 258]
The correct aetiopathological explanation is not yet known[(Pecina and Bojanic 2003 pg 259]
Chronic (Exertional) Compartment Syndrome
The aetiology for chronic compartment syndrome relates to a limiting non-compliant fascia surrounding an affected muscle compartment. Sports activity leads to increased muscle volume, and if there is non-compliant fascia this will result in an excessive intracompartmental pressure, which restricts blood flow, leading to an exercise ischaemia.
This leads to the characteristic signs of compartment syndrome; muscle weakness, cramp type pain over the affected compartment(s) and importantly altered neural sensation. These can appear on initiating exercise and disappears on cessation of the painful activity. [Pecina and Bojanic 2003 pg 260]
Stress Fracture of the Tibia
The most common localization of stress fractures of the tibia is in the area between the proximal and middle thirds of the bone [Pecina and Bojanic 2003 pg 262)]
The symptoms include dull pain, localized to a small area approximately 2-3cm in diameter, which is usually associated with swelling over the area. [Pecina and Bojanic 2003 pg 262]
Palpation over the area confirms the diagnosis. Swelling can be palpated, and exquisite tenderness can be elicited over the area. Pain is always localized and never diffuse.
Factors Predisposing to Shin Splints
I have reviewed many books on the subject (see bibliography) and there is no consensus as to why this happens.
Training errors, i.e. increasing training volume by greater than 10% each weak, ill fitting shoes, leg length discrepancies, pronated and supinated feet have all been mentioned (Pecina and Bojanic 2003, Kreider et al 1998). With treatment regimes concerned with non-steroidal anti-inflammatories, rest stretching, orthotics and proper fitting running shoes being the order of treatment, I could not find any mention of an osteopathic approach to this syndrome.
However, although not in the literature that I have read, practically it is of paramount importance to obtain optimal biomechanical alignment of the spine and lower limbs when treating over use syndromes such as ‘shin splints’.
Anything that prevents full dorsiflexion of the ankle joint will inevitably lead to compensation of the entire leg as it attempts to regain full range of motion; this compensation will also attempt to heal any injured tissues.
Need to look at assessment/ evaluation and treatment techniques for the following
- Ankle mortise;
- Individual joints of the foot;
- Sup/inf tib/fib joint;
- Subtalar joint;
- Tibial torsion;
- Tib post, flexor hal longus and dig longus;
- Hip position;
- Rotated innominate;
- Spinal mechanics;
- Piriformis syndrome;
- Leg length real and functional;
- Proprioception.
(Credit: D. Lintonbon and J.Webb 2005
David & Jim have compiled the above list as the literature is devoid of specific techniques for the treatment of shin splints.

Jogger's/Foot Pain
Foot, ankle and lower leg pain can be sustained by sportspersons of all ages and experience levels, including;
- Shin splints-myositis of Tibialis posterior/ant (see above);
- Calf pain;
- Talotibial/Fibulotalar ligamentous strain;
- Achilles tendon strain/bursitis;
- Inflamed calcaneal fat pad;
- Plantar fascitis, causing calcaneal spur pain;
- Hallux valgus/bunion/gout;
- Metatarsalgia;
- Osteoarthritis of Great Hallux metatarsophalangeal joint.
The pronated foot is a common cause of foot pain because of its deviation from the norm. Thus the foot, supported by its musculature fatigues from excessive or chronic normal use. The heel everts in the pronated foot hence the talus slides medially. The forefoot tarsal heads in turn abducts and widens, flattening the metatarsal arch with the metatarsal heads becoming more weight bearing with resultant Metatarsalgia.
The muscle most involved is the invertor Tibialis posterior that becomes elongated, tender and is rendered functionally ineffective on weight bearing.
In chronic pronation the lateral evertors shorten (peronei) to take up the slack. Toe extensors change their alignment and become ankle-foot evertors. The talocalcaneal ligament thus becomes taunt in supination and eventually becomes inflamed and painful under stress. The longitudinal arch becomes flattened and stresses the plantar fascia causing a spur.
Treatment
- Assess and treat plantar fascia, hypertonicity of the peroneal group through soft tissue, MET techniques;
- Assess sub/tib talar joints. Intrinsic joints of the foot;
- Assess superior/inferior tib/fib joints;
- NSAIDs / Gel during acute phase;
- Orthotics assessment;
- Shock absorbing insole/heel pad;
- Correct footwear;
- Analyse gait pattern.
Bibliography
Chaitow, L and Delaney, J.W. Clinical application of neuromuscular techniques. Volume 2: The lower body. Churchill Livingston, England. 2002.
Greenman, P.E. Principles of manual medicine. 2nd Edition. Lippincott Williams and Wilkins. Baltimore, USA. 1996.
Kreider, R.B., Fry, A.C, and O'Toole, M.L. Overtraining in sport. Human Kinetics, Leeds, UK. 1998.
Magee, D. J. Orthopaedic physical assessment. 2nd edition. W. B. Saunders, Philadelphia, USA. 1992.
Pecina, M.M and Bojanic, I. Overuse injuries of the musculoskeletal system. 2nd edition. CRC Press, London, UK. 2004.
Subotnick, S. I.,.Sports medicine of the lower extremity. 2nd edition. Churchill Livingston, England. 1999.
Ward, R. C., et al. Foundations for osteopathic medicine. 2nd edition. Lippincott Williams and Wilkins, Baltimore, USA. 2002.
Comments:
-
LG said..
I am 47 yo and run 12-15 mi pr wk. I have been running for the last 4 years and recently began to experience excrutiating shin splints that forced me to stop. I rested and resumed, only to experience the pain. In shear frustration I threw off my running shoes and ran barefeet...my pain imediatley bgan to subside. I went home and ordered my first pair of Vibrams......that was a year ago and I am on my second pair! Vibrams have completley eliminated my shin splints! I will never go back to a regular running shoe. I have discovered a whole new way to run and do so painlessly...I never knew that I was a heavy heel striker...the Vibrams have forced me to become a mid-forefoot runner...it has changed my running life! Vibrams were my answer!
-
John Deas said..
I am not into running but i would strongly suggest going barefoot or wearing minimalist footwear. As a 46 year old tree surgeon who has worn about the thickest and heaviest footwear there is over the years i have recently switched to wearing very light weight thin soled boots whenever possible for work and going around barefoot indoors and out when i can - no shin or tendon pains any more and also back ache is much reduced. This is really a no-brainer, if your feet can feel the ground properly your whole posture changes to accomodate changes in the terrain and you move more gently with your feet flexing and working as they evolved to do, sparing your joints from sudden jolting and stress.