Positive Health Online
Your Country

Add as bookmark
Cognition and Fibromyalgia: Symptoms, Causes and Treatment
by Dr Smita Pandey Bhat PhD(more info)
listed in fibromyalgia, originally published in issue 176 - November 2010
Cognition is the ability to think, perceive, know and understand the world. The term cognition is taken from the Latin word 'cognoscere' that means to know. In psychology the cognition refers to mental functions, mental processes and states of intelligent entities. The particular focus is on comprehension, inferencing, decision- making, planning and learning. The term cognition is broadly the act of knowing that ends up in thought and action.[1]
Introduction of Fibromyalgia
Fibromyalgia is a chronic syndrome characterized by tiredness , pain in muscles, bones, joints and tender points. (Tender points are places in the neck, shoulders, back, hips , arms and legs that hurt when touched).[2,3] Fibromyalgia is taken from the Latin words (fibra+ myo+ algos). Fibra means fibre or fibrous tissues, myo means muscles and algos means pain. The term was coined in 1976.[4] It more affects females than males with a ration of 9:1. by ACR (American College of Rheumatology) criteria.[5] Fibromyalgia can occur in 3 to 6% of the population. The age of onset is between 20 and 50, though it may occur in childhood as well.[6]Symptoms
The major symptoms of fibromyalgia are widespread pain, tenderness to light touch, moderate to severe fatigue, heightened sensitivity to skin, tingling sensation achiness in the muscle tissues, prolonged muscle spasms, weakness in the limbs, and nerve pain and also chronic sleep disturbances.[4] Other symptoms include headaches and facial pains, depression, anxiety, mood changes, dizziness and difficulty concentrating etc.[7] In addition to above symptoms, the patients may experience cognitive dysfunctions as well.Causes
The causes of this disease are unknown. There are several theories which state the causes of pain. One such theory is 'central sensitization' which states that the people with fibromyalgia have lower threshold of pain because of the increased sensitivity that causes pain. Other theories state that the sleep disturbances, injuries, infections abnormalities of autonomic nervous systems( sympathetic nervous system dysfunction) and changes in muscle metabolism (reduced blood flow to muscles) etc can cause fibromyalgia. Also , psychological stress. and hormonal changes may cause fibromyalgia.[7] The increased psychosocial stress, excessive physical exertion, and lack of slow- wave sleep and changes in humidity and barometric pressure may exacerbate the symptoms.[4]Risk Factors
The risk factors include the female sex, early and middle adulthood, disturbed sleep patterns, family history and rheumatic disease.Diagnosis
Strictly speaking there are no diagnostic criteria for this disease. But there is a widely accepted criteria for research purposes elaborated in 1990 by the American Centre of Rheumatology , popularly known as AMR criteria.[4] This is as follows:- A history of widespread pain lasting more than three months, affecting four quadrants of the body i.e. both sides and above and below the waist;
- There are 18 tender points out of which the patient may feel pain in 11 or more tender points.[8]
Treatments
Drug treatments include analgesics, antidepressants, anti-seizure drug and muscle relaxants. Non drug treatments includes physical exercises, massage treatment , stress management, cognitive behaviour therapy and neurofeedback, or biofeedback. Holistic treatments include management of sleep, diet, stress, pain, managing blood sugar levels and avoiding known triggers etc.[4,7]Fibromyalgia and Cognition
The patient may experience cognitive dysfunction ( known as 'brain fog' or 'fibro fog') which may be characterized by impaired concentration, unclear thinking and short-term memory consolidation, impaired speed of performance, inability to multi-task, and cognitive overload.[9,10] Fibro fog is the term described by Stuart Donaldson as "decreased ability to concentrate, decreased immediate recall, and an inability to multi-task".[26]Other symptoms include confusion and forgetfulness, inability to recall simple words and transposing words and numbers. Sometimes cognitive functions are so impaired that they get lost in familiar places and they have difficulty in communication. Sometimes they lose their jobs or paediatric patients drop out of school.[13] Also, there is difficulty in finding the right word for the conversation and they have trouble retaining new information.[25]
Causes of Cognitive Dysfunction In Fibromyalgia
- The patients were studied on CT(SPECT) to visualize their brain. It was found that there was decreased blood flow in the right and left caudate nuclei and thalami.[13]
- Abnormal levels of neurotransmitters such as substance P, serotonin, dopamine, norepinephrine, and epinephrine may be cause cognitive dysfunction. Neuroendocrine imbalance of the HPA axis may play a role in fibro-fog.[13]
- The distracting quality of pain may be another possible cause of the cognitive dysfunction. Cognitive performance of patients with fibromyalgia is correlated with their reported level of pain.[13]
- Researchers are looking at tissue volumes in areas of the brain (hippocampus) that may be damaged by the effects of stress hormones.[13]
- The results of a study by Elvin et al (2006) support the suggestion that muscle ischemia can contribute to pain in FM, possibly by maintaining the central nervous changes such as central sensitization / disinhibition.[19]
- Others studies have implicated yeast overload, water retention, and glial-cell abnormalities as causes of cognitive dysfunction in fibromyalgia.
Fibromyalgia, Sleep And Cognition
Cote and Moldofsky (1997) studied 10 female patients with fibromyalgia and a matched non comparison group. They spent two nights in the sleep laboratory. The subjects completed self assessment of a computerized battery and performance tests at hourly intervals from 7.0h to 20h. The results indicated that fibromyalgia patients spent more time on stage 1 sleep. They reported greater sleepiness, more fatigue, more pain, more negative mood, and lower accuracy on performance tasks across a 14 h day. The Fibromyalgia group was slower in speed, but not impaired in accuracy, on performance of complex tasks, i.e., grammatical reasoning, serial addition/subtraction, and a simulated multi-task office procedure.[11]Fibromyalgia ,Cognitive Ageing and Cognition
Park et al (2001) studied three groups of patients- fibromyalgia patients with concomitant depression, and in the absence of medications and age and education matched controls and education, matched older controls (individually matched to be 20 years older than the fibromyalgia patients). They found that older controls performed more poorly than the younger controls on speed of processing, working memory, free recall, and verbal fluency. Fibromyalgia patients performed more poorly on all the measures than the age matched controls, except for information processing measures. Fibromyalgia patients performed like the older ones, though they had better speed of processing and poorer vocabulary. Fibromyalgia patient's cognitive performance has been correlated with the pain, but not with anxiety and depression.[13]Fibromyalgia and Attention
Dick et al (2002) compared the fibromyalgia patients with the rheumatoid arthritis and musculoskeletal pain patients and normal controls. They found that all three groups of chronic pain patients, regardless of diagnosis, had impaired cognitive functioning on an ecologically sensitive neuropsychological test of everyday attention.[30]Fibromyalgia and Memory
Glass (2006) found that the fibromyalgia patients have memory complaints. Objective cognitive testing demonstrates long-term and working memory impairments.[14] Park et al (2001) found that fibromyalgia patients reported more memory complaints as compared to older or younger controls. Also , these complaints were correlated with poor cognitive performance.[13] In a study by Suhr (2003) it was found that the fibromyalgia patients reported more memory complaints and more depression, pain and fatigue than the other groups(chronic pain group and healthy control group). But, when controlled for pain, fatigue and depression, no difference was found between the groups. In a study by Katz et al (2004) it was found that memory decline and mental confusion were coupled more often in patients with fibromyalgia syndrome (50.9-8.8%).[27] Sephton et al(2003) examined relative influences of neuroendocrine function and psychological factors on declarative memory among 50 women with fibromyalgia. Neuroendocrine function and depression had significant independent associations with memory function. These findings suggest that a basic disorder of endocrine stress responses may contribute to the cognitive symptoms experienced by fibromyalgia patients.[28]Glass et al(2005) studied twenty-three Fibromyalgia patients, 23 age- and education-matched controls, and 22 older controls completed the Metamemory in Adulthood (MIA) questionnaire, which assessed beliefs about seven aspects of memory function. Group differences on the seven scales were assessed, and scores on the capacity scale were correlated with objective memory performance. Fibromyalgia patients reported lower memory capacity and more memory deterioration than did either control group.[29]Fibromyalgia and Information Processing
Glass (2006) found that CFS patients have slow information-processing.[14] Sletvold et al (1995) compared 25 patients of fibromyalgia with 22 patients of major depression and 18 healthy controls. The results indicated that the fibromyalgia patients showed non specific deficits in information processing capacity. However, the major depression patients showed a compromise in right hemisphere which was not found in fibromyalgia patients.[20] Eleven patients showed impairment on at least one task of cognition without stimulus and 30 showed impairment on the cognition with the stimulus competition. The findings validate the perception of failing memory in patients with fibromyalgia which is linked to a source of distraction.[16]
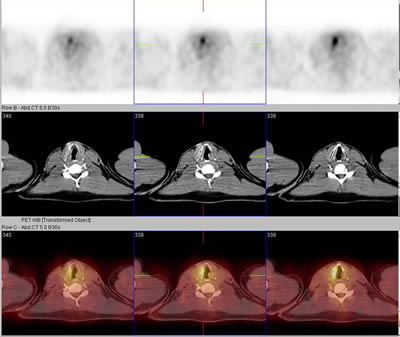
SPECT will demonstrate that there is a lack of perfusion (blood flow)
to a part of the brain, but it will not show the defect causing it.
Courtesy of http://neurotalk.psychcentral.com/thread10355-2.html
Neuroimaging studies demonstrate cerebral abnormalities and a pattern of increased neural recruitment during cognitive tasks.[14]
Fibromyalgia and Receptors
The study by Bazzichi et al.(2006) showed that there is an up-regulation of Peripheral benzodiazepine receptors on platelets of fibromyalgic patients and it seems to be related with the severity of fibromyalgia.[17]Fibromyalgia and Cognitive Behaviour Therapy
In most studies Cognitive Behaviour therapy (CBT) provided the worthwhile improvements in pain-related behaviour, self efficacy, coping strategies and overall physical function. Bennett and Nelson (2006) reviewed results from 13 programs using CBT, alone or in combination with other treatment. The analysis of the results showed that the CBT provided improvements in patients with fibromyalgia.[18]Fibromyalgia and Hypervigilance
Dohrenbusch (2001) found that most of the literature review does not show the trait like feature of hypervigilant information processing in patients with fibromyalgia.[21] On the other hand McDermid (1996) et al found that generalized hypervigilance is present in the patients with fibromyalgia. They studied 20 fibromyalgia, 20 patients with rheumatoid arthritis and 20 normal controls. The fibromyalgia patients have lower threshold and tolerance for pain than the rheumatoid arthritis patients but rheumatoid arthritis patients have lower thresholds than normals.[22] Lorenz et al (1998) studied 10 patients with fibromyalgia and matched normal controls. They found that amplitudes of middle-latency (N1) and long-latency (P2) laser evoked potentials (LEPs) were significantly higher in Fibromyalgia syndrome than in controls. And laser intensity at pain but not at sensation threshold was lower in Fibromyalgia syndrome than in controls.[23]Carrillo et al (2006) found that fibromyalgia patients presented shorter N1 and P2 latencies and a stronger intensity dependence of their auditory evoked potentials. Both results suggested that fibromyalgia patients may be hypervigilant to sensory stimuli, especially when very loud tones are used. The larger auditory evoked potentials suggested that defects in inhibitory system which protect against overstimulation is the crucial factor in the pathophysiology of fibromyalgia.[24]
References:
1. http://en.wikipedia.org/wiki/Cognition - 53k 2. www.nlm.nih.gov/medlineplus/fibromyalgia.html - 45ka
3. About Fibromyalgia. National Fibromyalgia Association.
4. http://en.wikipedia.org/wiki/Fibromyalgia - 115k -
5. Fibromyalgia med790 at e medicine.
6. McBride CR.Fibromyalgia Clinical Vignette. UCLA Department of Medicine. 03 Jul 2000.
7. www.mayoclinic.com/health/fibromyalgia/DS00079 - 23k
8. National Institute of Arthritis and Musculoskeletal and Skin Diseases. Questions and Answers About Fibromyalgia -- How Is Fibromyalgia Diagnosed?. National Institutes for Health. June 2004.
9. Leavitt F, Katz RS, Mills M, Heard AR Cognitive and Dissociative Manifestations in Fibromyalgia. J Clin Rheumatol. 8 (2): 77-84. PMID 17041327. 2002.
10. Frank Leavitt. Fibrofog, Fibromyalgia and Dissociation -- Understanding why some memory-impaired patients with fibromyalgia score normally on neuropsychological testing.
11. Cote K.A, Molodfsky H. Sleep, daytime symptoms, and cognitive performance in patients with fibromyalgia. Journal of Rheumatology 24, (10,) 2014-2023. 1997.
12. Park D.C, Glass J.M,Minear M, Crofford L.J. Cognitive function in fibromyalgia patients 2001 Arthritis Rheum.44(9): 2125-33. Sep 2001.
13. www.emedicine.com/PMR/topic47.htm - 149k
14. Glass JM .Cognitive dysfunction in fibromyalgia and chronic fatigue syndrome: new trends and future directions Curr Rheumatol Rep. 8(6):425-9. 2006.
15. Suhr JA. Neuropsychological impairment in fibromyalgia: relation to depression, fatigue, and pain. J Psychosom Res. 55(4):321-9. 2003.
16. Leavitt F, Katz RS. Distraction as a key determinant of impaired memory in patients with fibromyalgia. J Rheumatol.33(1):127-32 PMID: 16395760. Jan 2006.
17. Bazzichi L, Giannaccini G, Betti L, Italiani P, Fabbrini L, Defeo F, Giacomelli C, Giuliano T, Rossi A, Uccelli A, Giusti L, Mascia G, Lucacchini A, Bombardieri S. Peripheral benzodiazepine receptors on platelets of fibromyalgic patients Clin Biochem. 39(9):867-72. Sep 2006.
18. Bennett R, Nelson D. Cognitive behavioral therapy for fibromyalgia. Nat Clin Pract Rheumatol. 2(8):416-24. 2006.
19. Elvin A, Siosteen AK, Nilsson A, Kosek E. Decreased muscle blood flow in fibromyalgia patients during standardised muscle exercise: a contrast media enhanced colour Doppler study. Eur J Pain. 10(2):137-44. Feb 2006.
20. Sletvold H, Stiles TC, Landrø NI. Information processing in primary fibromyalgia, major depression and healthy controls. J Rheumatol. 22(1):137-42. 1995.
21. Dohrenbusch R. Are patients with fibromyalgia "hypervigilant"? Schmerz. 15(1):38-47. PMID: 11810328. 2001.
22. McDermid AJ, Rollman GB, McCain GA. Generalized hypervigilance in fibromyalgia: evidence of perceptual amplification. Pain. 66(2-3):133-44. PMID: 8880834. 1996.
23. Lorenz J. Hyperalgesia or hypervigilance? An evoked potential approach to the study of fibromyalgia syndrome. Z Rheumatol.57 ( 2):19-22. PMID: 10025076. 1998.
24. Carrillo-de-la-Peña MT, Vallet M, Pérez MI, Gómez-Perretta C. Intensity dependence of auditory-evoked cortical potentials in fibromyalgia patients: a test of the generalized hypervigilance hypothesis. J Pain. 7(7):480-7. PMID: 16814687. Jul 2006.
25. www.fibromyalgia-symptoms.org/fibromyalgia_fibrofog.html -
26. Stuart Donaldson, Ph.D., "Fibromyalgia: A Retrospective Study of 252 Consecutive Referrals," Canadian Journal of Clinical Medicine 5( 6) :117. 1998.
27. Katz RS, Heard AR, Mills M, Leavitt F. The Prevalence and Clinical Impact of Reported Cognitive Difficulties (Fibrofog) in Patients With Rheumatic Disease With and Without Fibromyalgia. J Clin Rheumatol 10(2):53-58. Apr 2004.
28. Sephton SE, Studts JL, Hoover K, Weissbecker I, Lynch G, Ho I, McGuffin S, Salmon P. Biological and psychological factors associated with memory function in fibromyalgia syndrome Health Psychol.22(6):592-7. PMID: 14640856. Nov 2003.
29. Glass JM, Park DC, Minear M, Crofford LJ. Memory beliefs and function in fibromyalgia patients. J Psychosom Res. 58(3):263-9. Mar 2005.
30. Dick B,Eclleston C, Crombez G. Attentional functioning in fibromyalgia, rheumatoid arthritis, and musculoskeletal pain patients. Arthritis and Rheumatism 47(6): 639-644 [30]. 2002.
Comments:
-
No Article Comments available