Positive Health Online
Your Country

Neutrophil Reactivity - The NuTron Test
listed in allergy testing, originally published in issue 30 - July 1998
The subject of food “allergy” is highly contentious. Debate, though, rarely transcends the most basic question of existence. With nutrition almost absent from medical training (only one in four medical schools in the United States even bothers to offer a course) and no obvious financial beneficiary from research, investigation of a biochemical pathway is virtually non-existent. In place of clear understanding we have dramatic anecdotes countered by sterile and, at times hostile, scepticism. Although there are celebrated papers in the learned journals they have little impact on general practice. Most lay advocates’ knowledge is gleaned from the pages of women’s magazines and Sunday supplements and their efforts and results achieved in spite of, rather than because of, their GP.
 |
 |
 |
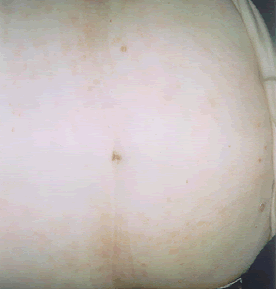 |
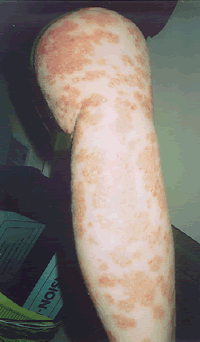
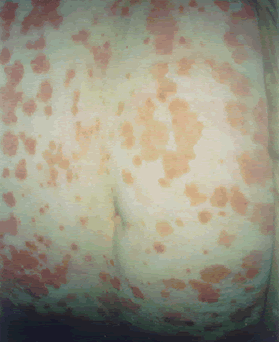
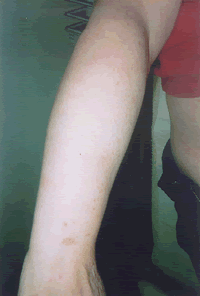
| Patient A. After a decade of suffering psoriasis and expenditure on allopathic treatments in excess of £10,000, dietary control eliminating foods which could be shown to stimulate the neutrophil response, cleared up in eight weeks. | |
Confusion is endemic, persuading the unaligned to steer clear. Examples abound. Take the term itself; “allergy” means different things to different people, hardly a situation likely to foster confidence. The classical allergists have their own definition based on raised levels of IgE. Where there is no raised IgE but symptoms respond to the removal of a suspect food, the term “non-IgE mediated allergy” or “food intolerance” is generally but, confusingly, not exclusively, used.[1] To many, the terms are synonymous. Others insist on further caveats. Food intolerance, they say, does not involve the immune system. So what of a reaction that does involve the immune system but does not cause raised level of IgE? A food reaction, perhaps? Does it really matter if the terms are muddled? The answer is quite simply, yes. An “allergic” reaction that results in anaphylaxis is extremely rare. A perfect opportunity for the sceptic to dismiss the subject as an intellectual sideshow. However, “food reactions” are very common.[2] More importantly, the latter, if prolonged, can result in inflammatory disease.[3,4,5] Discovering and removing these foods from a patient’s diet provides a potent opportunity for treatment across the spectrum of inflammatory conditions (see Table 1). The current confusion is actively preventing the development of this unique opportunity.
Testing methods used to detect food reactions, and the hardware upon which they rely, are a further example of a distinct lack of scientific rigour. Without an agreed and demonstrable biochemical pathway, tests have evolved which measure different responses yet purport to answer the same question, i.e. what foods should the individual avoid.
Most laboratory-based methods agree that an immune response is involved. Testing falls into three main categories. The oldest relies on a microscope to investigate the condition of the white cells,[6] this was augmented by the simple cell counter and, latterly, the development of the chemical marker assay.[7,8] Each, for its time, represented a technological advance but none really superseded its predecessor, consequently specialists continue to use the method to which they have become accustomed. This is analogous to a family choosing to buy a Model “T” Ford unaware of the existence of the Mondeo with its ABS, air bags and crumple zone safety features (not to mention 0-60 in 10 seconds rather than ten minutes!). As most authorities still refer to the elimination diet, featuring a period of fasting followed by structured reintroduction of foods over many weeks, as the “gold standard”, it would seem that none have captivated the professional user.
Without an agreed biochemical pathway it was impossible to judge the relative merits of the different techniques. Now a more complete understanding reveals serious deficiencies in each design.
It is generally accepted that food is broken down by the process of digestion to sustain and repair the body. This oversimplification is supported by a view of the gut as little more than a “hosepipe” connecting the mouth to the anus. Yet a growing body of evidence shows that both of these positions are now grossly incomplete.[9]
Not all food is subject to complete breakdown. Particles of partially digested foods can adhere to the gut wall, in particular within the crypts. Where sufficient amounts gather, absorption into the cells lining the gut can be affected.[10,11,12,13] Should the amount of food particulate overwhelm the lysosomal defences within the cell, the residue will be passed directly into the blood stream.[14,15] Furthermore, the release of stress chemicals locally or from the brain will cause the tight junctions joining the cells to separate widening the gap.[20]
This allows food particles to gain immediate access to the blood stream[14,15] and provides an opportunity for white cells to migrate into the gut lumen.[16,17,18,19] The resulting inflammation within the gut, can create the very conditions required for markedly increased gut permeability.[21,22] (Possibly why inflammatory conditions are often chronic and resolution so rapid once foods have been removed from the diet.)
Once in the bloodstream, a food particle can be carried to any organ or tissue – hence the array of inflammatory conditions that threaten the body. On entry it will be marked as an immune complex and attract the attention of the immune system[23,24] – initially the neutrophil. This cell is the key to the inflammatory response and to a new means of detecting problem foods. Unfortunately, the cell’s activities are swift and, in order to protect the host, is soon absorbed by macrophages – quite simply by the time most investigators have begun their observation the cell is long gone. This has led to its importance being overlooked, often in favour of more obscure members of the system.
As little as a decade ago the neutrophil was considered a rather dull, belligerent cell, a pawn in the company of aristocrats. Yet now researchers stand aghast at a cell that is recognised as containing more than fifty different types of inflammatory chemicals, that is capable of a wide range of subtle responses chosen to meet the needs of different circumstances.[25,26,27] Here is a cell that can react in an oxidative or a non-oxidative manner, create some of the most destructive chemicals in existence;[29] a cell that can recruit and orchestrate further assistance from others of its own kind.30 It even has the ability to delay its own preordained death in the service of the host.[31]
The comprehensive arsenal at the disposal of the neutrophil makes a mockery of cell counting as it can release its chemical load without destroying itself – as a result, the cell count remains the same but the damage is done. Equipment that measures single chemical markers is equally redundant for the cell is capable of using any number of different chemical to fulfil its function. Despite its capabilities, the neutrophil is tiny, has a diameter ranging from 8-13 microns, this makes the microscope virtually useless – as magnification is increased to a useful level the field diminishes to the point where viewing a reaction is a matter of luck.
The recent development of the automated haematology analyser provides a tool that can give a comprehensive measure of the neutrophil’s reaction to a food in vitro. The NuTron Test uses a haematology analyser (Sysmex NE-8000) to assess the degree and nature of the neutrophil response to a food from a sample of blood incubated with reconstituted food extract (as routinely used for intradermal “skin-prick” testing). The unique combination of Radio Frequency (RF) and Direct Current (DC) in addition to cell sizing allows the cell’s internal and external characteristics to be measured. This provides data on phagocytosis, aggregation, degranulation, vacuolation and surface activation (see Table 2).
By assessing the effect of a food extract on whole blood against a control sample of the same blood, it is possible to detect foods which do not activate the neutrophil. Constructing diet exclusively from such foods provides a simple and highly effective means of controlling inflammation. The implications of this discovery are far reaching. Inflammatory illnesses are costly in both quality of life and medical resources. Treatment is simple, involving little more than a change in food purchase and preparation habits. Clinical results are both dramatic and sustainable suggesting that as the closing years of the nineteenth century saw an end to the water-borne epidemics, the closing of the twentieth century may see an end to the epidemic of inflammatory disease.
|
TABLE 1 Conditions – General Conditione – Specifi to women Conditions – Children |
|
TABLE 2 Aggregation: Vacuolation: Phagocytosis: Degranulation |
References:
1. J. Pediatr. vol 121: S7 – S11 1992. Ferguson A2. Lancet 343: 1127-1130. 1994. Young E et al
3. Physiotherapy Vol 77: 1-12. 1991. Cooper J
4. Lancet p1419-1420. 1988. Corbeel L. et al
5. Lancet 2: 1115-1117. 1982 . Jones A et al
6. Lancet April 30 p989. 1983. Fennell P G S
7. J. Immunol. Meth. 3: 606. 1985. Husby S et al
8. Scand. J. Gastroenerol. 25: 287-292. 1990. Fausa H O et al
9. Recent Advances in Gastroenterol Chap 13 : 281-299. Jones A & Hunter J O
10. Am. J. Physiol. 267: G151-165. 1994. Perdue M H et al
11. Annals of Allergy Vol 59. pt 2 : 127-130. 1987. Andre C et al
12. Am. J. Physiol. 32: G467-475. 1995. Anderson J M et al
13. Lancet 1171-1173. 1984. Bjarnason I et al
14. Gastroenterol. 67: 531-550. 1974. Walker W A and Isselbacher K J
15. Gastroenterol. 104: 622-639. 1993. Sanderson I R and Walker W A
16. Can. J Comp. Med. Vol 38: 193-202. 1974. Bellamy J E C and Nielsen N O
17. Dig. Dis Sci. 33: 1383-90. 1988. Kordossis T et al
18. Scand J Gastroenterol. 27: 793-798. 1992. Roseth A G et al
19. Dig. Dis. Sci. 33: S6-S15. 1988. Grisham M B et al
20. Clin. Exp. Immunol. 97: 339-341. 1994. Mason D
21. Nature. 289: 646-650. 1981. Wedmore C V and Williams T J
22. Cancer Res. 50: 2172-2176. 1990. Mullin J M et al
23. Clin. Exp. Immunol. 43: 574-582. 1981. Mowat A M and Ferguson A
24. J. Exp. Med. 134: is-14s. 1971. Henson P M
25. J Immunol. 124: 885. 1980. Bentwood B J et al
26. J.Immunol. 119: 1068. 1977. Wright D G et al
27. Clin. Res. 32: 320. 1984. Gallin J I
28. Am. J. Pathol. 135: 435-38. 1989. Varani J et al
29. N.Eng. J. Med. 303: 27. 1980. Weissman G
30. Phil. Trans. R. Soc. London B. 345: 327-333. 1994. Haslett C et al
31. J Leuk. Biol. 54: 283-288. 1993. Lee A et al
Comments:
-
Cheryl Langley said..
Hi there. I live in jhb south africa and had a blood test done approx 12 years ago called Nutron Life. They took 2 vials of blood and sent it to a lab in UK who dropped the blood over 90 types of food to test which food I was "allergic/sensitive" to. I am wanting to know if this is what you do and if you have a representative in JHB South AFRICA. Please let me know
Many thanks
Cheryl
-
Z.M. said..
Having read the nutron diet and It's what I was looking for ,
where oh where can I find details of how to get the test?
-
Tania Joubert said..
Hi
I'm not feeling well the different doctors have given different diagnostics, IBS , leaky gut, colitis . I did the NuTron test in 2002 in South Africa - Nelspruit. I would like to repeat as I lost my results and many years passed. I am now leaving in Witbank a town close to Johannesburg 1h and 30 minutes drive.
I would like to redo the test as I am feeling ill. Where can I go to be tested? When I did the test 12 years ago the vials were sent to a lab on the UK. Can this still be done?
-
Tania Joubert said..
Hello
I have done this test 12 years ago in Nelspruit in South Africa. Two vials of blood were taken and the blood was sent to the UK. I would like to repeat the tests as I lost the original test results and time as passed by. I am now with gastrointestinal problems and feeling sick and I don't know what is causing it.
I stay now in Witbank a town close to Johannesburg about 1h 30 minutes drive.
Is there a place here in South Africa where I can be assisted? I would appreciate your reply
Kind regards
Tania